Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
First developed to treat type 2 diabetes, Mounjaro (tirzepatide) was very popular among non-diabetics because of its strong weight-loss outcomes. Although taking the drug off-label might be tempting, it is essential to know that there are risks involved. In this article, I will explain Mounjaro side effects in non-diabetics and detail the complications and health issues that may present themselves during use of the medication without having a medical emergency.
What is Mounjaro and How Does It Work?
Tirzepatide, a drug that is prescribed for people who have type 2 diabetes, was given the name Mounjaro. The first certified it to control blood sugar along with diet and exercise. An intradermal injection of tirzepatide is given once a week.
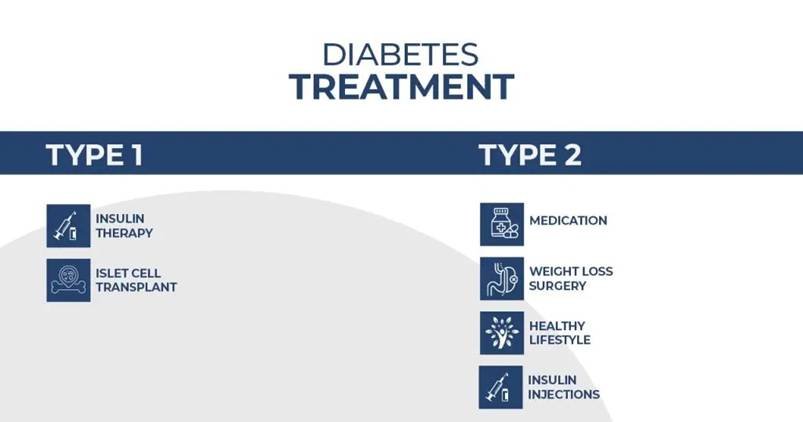
Original Purpose: Type 2 Diabetes Treatment
· Authorized to improve glycemic (blood sugar) controls among type 2 diabetics.
· Decreases the levels of glucagon being produced by liver, increases the amount of insulin being produced, and reduces the rate at which food exits the stomach to reduce the levels of glucose in blood.
Mechanism: Dual GIP/GLP-1 Receptor Agonist
Tirzepatide targets only two hormones:
- GIP (glucose-dependent insulinotropic polypeptide) receptor
- GLP-1 (glucagon-like peptide-1) receptor
This dual action means it can:
- With an elevated level of glucose, it promotes the production of insulin.
- Prevent excessive output of glucose in the liver.
- Remarkably reduces post-meal increases of blood sugar by decreasing the pace of stomach emptying.
- Less desire and food intake through an increase in satiety, or satisfaction.
- Have greater effects than the drugs targeting only GLP-1, namely in relation to the weight loss.
Why it’s being used by non-diabetics (especially for weight loss)
Tirzepatide (Mounjaro), despite being prescribed for type 2 diabetes, has caught attention for its impact on weight loss, even in those without the disease:
- Significant weight loss is reported by many non-diabetics, sometimes going beyond what is observed with equivalent medications.
- Clinical research has demonstrated that taking it as a weight reduction drug can help people without diabetes lose up to 13% of their initial body weight in six months.
- Because it mimics hormones related to satiety and glucose regulation, the medication lowers appetite and calorie intake, making it intriguing to those who are obese.
- By 2023-2024, it was certified under a different brand (Zepbound) for the treatment of obesity and chronic weight loss.
Off-label use disclaimer
- Off-label use alludes to the prescription of a drug for a use that has not been formally authorized by regulatory bodies.
- Not everyone approves of Mounjaro for weight loss alone. For non-diabetics looking to control their weight, doctors may prescribe it “off-label” in some circumstances or nation, specifically if previous treatments haven’t worked.
- While there is growing evidence that it can help non-diabetics lose weight, research on its long-term effects and safety is still ongoing.
- To be certain, medically appropriate use and to assess potential risks and benefits, anybody thinking about using Mounjaro for weight loss should speak with a healthcare provider.
Common Side Effects in Non-Diabetic Users
Tirzepatide is a very famous drug with weight loss properties, however, its non-diabetic users largely tolerate it but has few side effects that are also apparently common. These are most commonly mild to moderate and may happen as the body is getting used to medication especially when the dosage is increased.
Gastrointestinal issues
The commonest side effect, observed in up to 20.4 percent of clinical trials.
- Nausea: Incidence of nausea, diarrhea, and vomiting is common in diabetic and non-diabetic users.
- Vomiting: Found in approximately 9 percent of trial patients.
- Diarrhea: It was reported by the participants (16.2%) taking tirzepatide vs. 8.6% taking other therapies.
- Constipation: Appears in 2.5 percent of the users appear and comparatively very high amongst comparators.
- Other GI effects: Indigestion (dyspepsia), belching and abdominal pains as well are observed
Neurological and Fatigue-related effects
- Headache: Although headaches are not the most common, nonetheless it is found in a group of individuals, mostly attributable to the GI effects of dehydration or change in blood sugar levels.
- Fatigue: A minority of users complained of unusual fatigue at the beginning of tirzepatide treatment, most frequently on the first few weeks of treatment.
- Dizziness: Common, particularly with rapid weight loss, lower blood sugar level or dehydration caused by gastrointestinal effects.
Appetite Changes and Rapid Weight Loss
- Appetite Suppression: Hallmark effect up to 9.6% report decreased appetite, much more common than the other medications of similar purpose. This loss of appetite enhances massive weight loss.
- Weight Loss: Fast and considerable. Clinical research indicates that non-diabetic users should be able to lose approximately 13 per cent of their initial weight after six months.
Discussion by many users include wild appetite suppression that causes them to fast without intending to lose weight unintentionally afterwards.
Important Notes
- Majority of side effects are of short duration and occur due to the body adapting to tirzepatide.
- Major side effects are seldom witnessed, and people are advised to see a medical professional immediately when dire or proficient indications (like those of dehydration, continuous regurgitating or any severe headaches) are transpired.
These side effects and figures are based on studies on both diabetic and non-diabetic adults; non-diabetic users ought to understand that the figures in fact can vary on an individual level about occurrence and severity.
Differences in Side Effects Between Diabetics and Non-Diabetics
| Side Effect | Non-Diabetics | Diabetics |
| Nausea | 31% (high dose) | 23% (high dose) |
| Diarrhea | 23% | 19% |
| Vomiting | 12% | 13% |
| Weight Loss | Up to 21% of weight | Up to 15% of weight |
| Hypoglycemic Events | Occasional/possible | Less frequent |
| Ketoacidosis | Rare, reported | Not typically reported |
Key Takeaways:
- The condition in non-diabetics may be accompanied by more GI side effects, further weight loss and unexpected decreases in blood sugar or scarcely any ketoacidosis.
- Diabetics have controlled blood sugar that gives insulation to some of these dangers.
- Non-diabetic users also lack long-term safety data indicating the need to obtain medical supervision and additional studies.
It is highly recommended to have consultations with medical workers in case of starting to take tirzepatide or to continue taking it, more so when one is taking it as an off-label medication to lose weight.
You may also like to read: Diabetes Medications
Precautions & Medical Supervision
To be entirely safe and informative before taking Mounjaro (tirzepatide), and particularly, as a non‑diabetic, it is important to discuss the treatment with an expert medical professional and make an informed decision based on your past medical history and risk group.
It is highly advisable to adopt a low dose increase scheme. The treatment usually starts at a dose of 2.5mg once weekly and the dose is increased by 2.5mg every 4 weeks up to a maximum dose of 15mg with the aim of limiting gastrointestinal symptoms as also to maximize tolerability.
Monitoring is essential, especially in the period of titrating the dose, and relevant during the entire treatment. After the initial assessment, follow up visits after 4 weeks should assess the side effects, (e.g. nausea, vomiting), renal function (in case there is dehydration due to GI side effects), mood or psychiatric abnormalities, and weight response.
Notably, it should not be used in patients having personal or family history of medicinal Thyroid carcinoma (MTC) or Multiple Endocrine neoplasia syndrome type 2 (MEN 2) because there is a boxed note about thyroid C-cell Tumors in animals of Mounjaro usage.
Conclusion
Although Mounjaro has proved to be effective in weight loss, administration and utilization of this effect among non-diabetic populations are also associated with a variety of unwanted side effects and possible severe health complications. Ranging between gastrointestinal problems and more serious ones such as lowering blood sugar, pancreatitis, and thyroid complications, the dangers cannot be ignored. It is necessary to keep in mind the idea that Mounjaro is not a prescription that can be taken as a weight loss approved medication among individuals without diabetes type 2, and the off use can only be undertaken strictly at the control of the medical specialist. It is never advisable to take or even proceed with any form of medicine without consulting a prescribed medical health professional, more so one that has powerful impacts. The priority should be your safety, as well as your long-term health.