Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
A diabetic foot can be described as a variety of foot issues, which arise in diabetic patients because of the damage to the nerves (neuropathy), limited blood flow and difficulty fighting infections. It is a serious complication that may cause foot ulcers, infections as well as in severe cases may cause amputations unless they are managed in a proper manner. Due to a lack of sensitivity in the feet, diabetes patients often cannot detect minor trauma, and it becomes more severe within a very short period. The key to preventing diabetic foot-related complications and maintaining general mobility and health is daily foot care, early detection, and respective check-ups.
What Is Diabetic Foot?
A diabetic foot is any foot infection or affliction in an individual with existing or priorly experienced diabetes and is usually associated with nerve damage and vascular insufficiency. This involves sores (ulcers), infection, tissue destruction, gangrene (tissue death) and deformity (like Charcot foot). These issues could arise gradually and with no proper diagnosis and treatment in the early stages they may require amputation.
Common Conditions Associated with Diabetic Foot
- Ulcers:
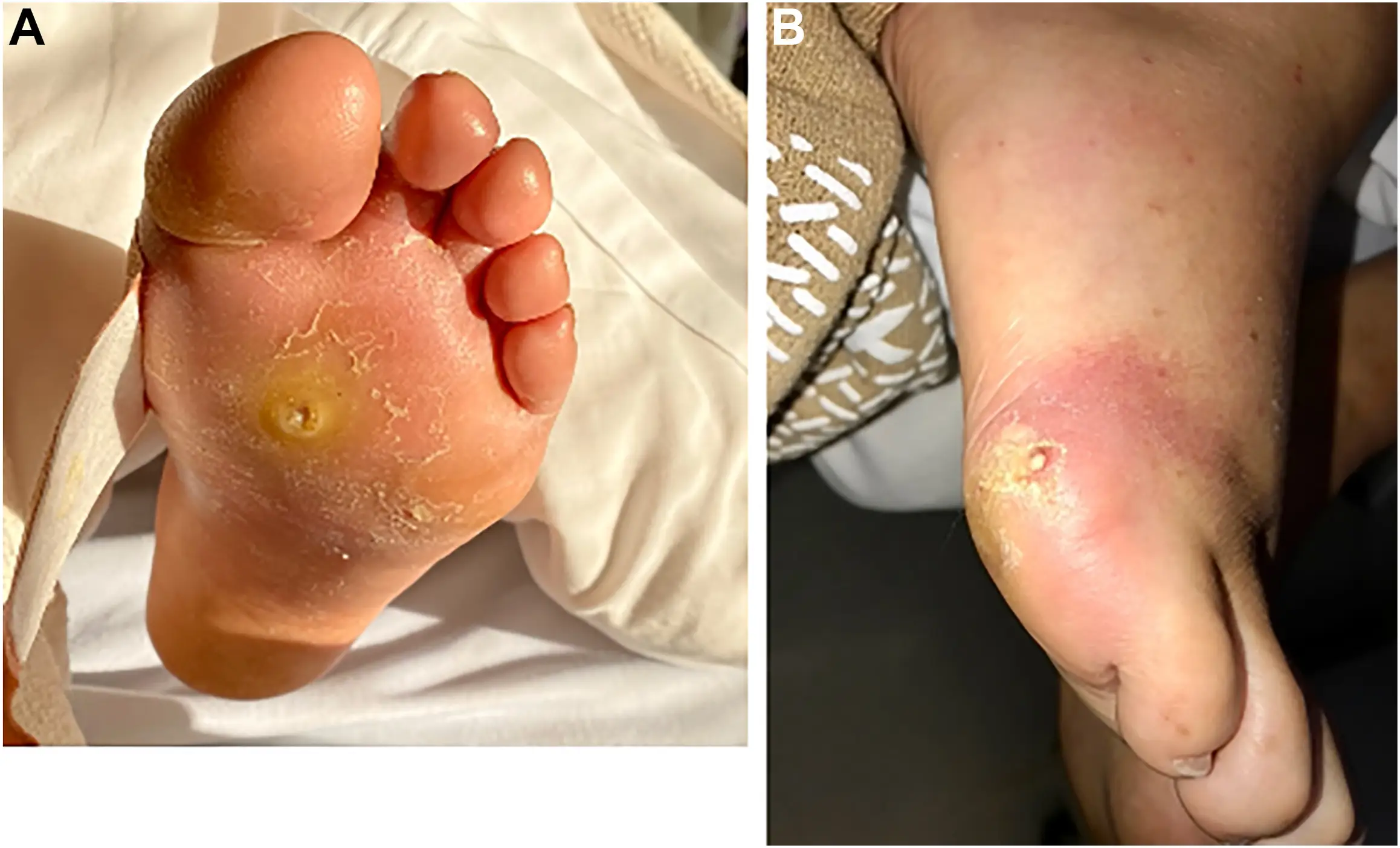
Open sores or wounds—most often on the bottom of the foot—resulting from the combination of nerve damage (loss of feeling) and poor circulation. Around 15–25% of people with diabetes will develop a foot ulcer in their lifetime. Ulcers can become severe and hard to heal, sometimes exposing bone or deeper tissue.
- Infections:
Foot ulcers are predisposed to infections given that they have poor immunity and blood flow. This may superficially become cellulitis or severe bone infections (osteomyelitis) and may become the reason of amputation unless appropriately addressed immediately.
- Gangrene:
This is cell death because of the extremely low blood flow or an absence of it. Failure to heal an early infection or ulcer may result in gangrene which can result in what amounts to partial or complete amputation of the foot.
- Charcot Foot:
A very serious form of complications of diabetic neuropathy in which bones and joints of the foot become weak and break – usually causing deformity and tendencies to change the way of walking. Early Charcot foot is marked by swelling, redness and warmth-later stages may result in the foot collapsing into a rocker-bottom configuration.
Common Causes of Diabetic Foot Problems
Diabetic foot issues are a combination of ongoing high blood sugar, the impact it has on nerves, blood vessels, and overall foot related health. The causes that are of greatest importance are:
1. Peripheral Neuropathy (Nerve Damage)
- Long-term high blood sugar destroys the nerves (especially pains in the feet and legs), which leads to such symptoms as numbness, tingling, pain, or loss of sensation.
- This decreased sensation implies that minor injuries, say, cuts, blisters, pressure on the feet due to the shoes, typically remain unnoticed and thus predispose to the wounds and infections.
2. Poor Blood Circulation (Peripheral Arterial Disease)
- The blood vessels in the body harden and narrow because of fat deposits (atherosclerosis), which slackens the circulation of blood to the feet brought about by diabetes.
- Inadequate circulation hinders wound healing, exposes the person to the danger of infections and leads to the occurrence of ulcers and gangrene.
- Peripheral arterial disease (PAD) occurs far more frequently in diabetics and is one of the main foot complication risk factors.
3. High Blood Sugar Levels Over Time
- The high level of blood sugar directly harms blood vessels and nerves chronically.
- It dampens the immune system, hinders healing, and enables foot problems that might be minor but soon develop into bigger infections or ulcers.
4. Foot Injuries and Pressure Points
- Due to neuropathy, individuals who are diabetic are not likely to feel pressure points, friction, or trauma under pressure because of tight shoes or ill-fitting footwear.
- Injuries that go unnoticed may grow into serious ulcers and infections- especially when the pressure is not tended or the injury is not observed in a timely manner.
5. Lack of Proper Foot Care
Poor self-inspection, hygiene, nail or callus trimming are three major causes that aggravate risk of ulcers, infections, and other foot issues.
Failure to visit the feet daily implies the lack of minor issues until they reach serious levels. A major preventable factor to serious diabetic foot complications is poorly managed foot care.
Symptoms of Diabetic Foot
- Tingling, Burning, or Numbness:
It leads to damage to nerves and causes a lingering tingling, burning sensation or numbness – typically in the toes and feet. People may begin to be numb to the point where they cannot sense temperature changes, painful injuries, etc.
- Swelling, Redness, or Unusual Warmth:
It may be associated with color changes and warmth, edema (swelling), or redness, suggesting that the process is inflammatory, infected, or that of a diabetic foot ulcer. These may involve slight but serious red flags.
- Open Sores or Ulcers That Don’t Heal:
Frequent wounds, blisters, or ulcers (more so on pressure points such as the soles, toes, or sides of the foot) are often non-healing. Such ulcers may look like red sores that are slow to heal because of weak blood circulation and numbness of nerves.
- Foul-Smelling Discharge or Pus:
Foul odor coming from an ulcer or wound, pus, or drainage that’s clear or colored, usually indicates an infection that needs immediate medical care. Socks or shoes may as well get stained.
- Changes in Skin Color or Texture:
Seek discoloration (red, blue, purple, black), shiny tight skin, thick clauses or skin breakdown areas. Changes in color may indicate having poor circulation, infection or gangrene.
- Foot Deformities or Difficulty Walking:
Chronic diabetes may modify the shape of the foot leading to architectural changes in the shape of the foot to include hammer toes, claw toes, Charcot foot, flattened arches, or bony prominences. The risk raises in the case of muscle weakness and the loss of sensation. These modifications lead to gait and make walking painful or difficult.
You may also like to read: Mounjaro Side Effects
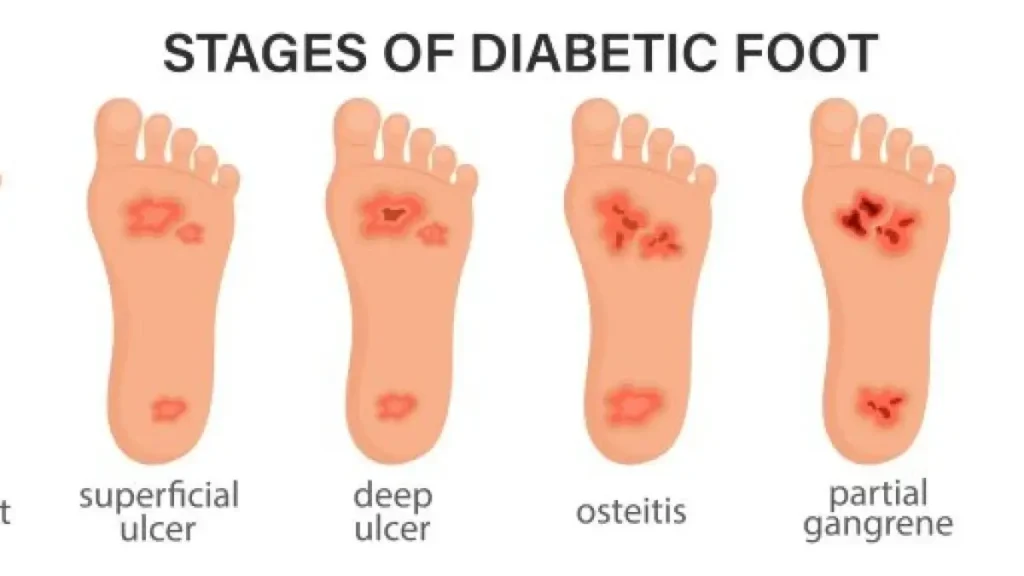
Stages of Diabetic Foot Complications
| Stage | Description | Key Features | Treatment Focus |
| Neuropathy Stage | Nerve damage → loss of sensation | Tingling, numbness, unrecognized trauma, deformities | Prevention, education, footwear |
| Ulcer Formation | Skin breakdown causing sores or ulcers | Calluses, blisters, open wounds | Wound care, pressure relief, vascular assessment |
| Infection and Tissue Damage | Infection of ulcers spreads causing cellulitis or osteomyelitis | Redness, swelling, pus, foul odor | Antibiotics, surgery, debridement |
| Risk of Amputation | Severe necrosis or infection threatening foot viability | Necrosis, gangrene, systemic infection | Surgical amputation, aggressive infection control |
How to Prevent Diabetic Foot Problems
As a preventative measure against diabetic foot issues, practice a habit of inspecting your feet daily- look at cuts, blisters, redness, swelling, and corns or calluses (mirror may be used). Practice proper hygiene by washing your feet daily with lukewarm (not hot) water, drying thoroughly—especially between toes—and applying moisturizer only to the tops and soles—never between toes.
Select comfortable diabetic socks that fit properly and provide cushioning and wicking and should not be caused by rigid seams or tight elastic cuffs. Clip toenails straight across and with smooth edges, meaning filing; remove corns, calluses and cuticles the home remedies way; go to the doctor.
Have regular checkups with a podiatrist at least once a year (and more frequently e.g. every three to six months) with any foot problems or a dry nail (neuropathy) or circulation issues.
Finally, it is important to have good control of blood glucose levels and ensure that cardiovascular risk factors such as hypertension and smoking are kept in check, because a well-controlled diabetes will greatly reduce the chances of developing foot complications.
Treatment Options for Diabetic Foot
Treatment of diabetic foot problems should be multi-factorial in nature and should focus on several goals including promoting healing, avoiding infection, and complications like amputation. The following are the major treatment modalities:
1. Cleaning and Dressing Wounds
- Ulcers and wounds need to be cleaned up to eliminate dirt and debris on a regular basis.
- The wounds are properly designed to ensure that a moist environment develops which helps in healing.
- Special dressings (e.g. hydrocolloid, calcium alginate) assist in the absorption of exudate and allow less bacterial growth.
2. Antibiotics for Infections
- In case the ulcer or wound is infected then specific antibiotics are ordered based on culture results.
- There is a possibility of severe infections which would need hospitalization and intravenous antibiotics.
- It is important to take early and appropriate antibiotic therapy to remedy infection and commence before it spreads to deeper tissues or bone (osteomyelitis).3. Offloading Techniques
- Offloading the damaged foot is crucial in alleviating the pressure on the ulcer to enable the wound to heal.
- Methods refer to total contact casting, specialized shoes, braces or even admission to bed rest.
- Offloading aids in stopping additional trauma to the wound and the restoration of the tissue.
3. Debridement (Removal of Dead Tissue)
- Debridement of calluses and dead (necrotic) tissue is beneficial as this reduces the chances of infection, and it accelerates healing.
- It may be surgical, enzymatic or biological (e.g. maggot therapy).
- It should be continuous in keeping the wound clean and encourage the initiation of fibrous tissues.
4. Surgery for Advanced Cases
- Surgery might also be required to drain abscesses, eliminate infected bone or tissue or to correct deformities that may create complex inciting factors.
- In its worst form where there has been massive tissue death or a non-responsive infection there could be partial or complete amputation to help save the life of the patient.
5. Advanced Therapies
- High-end treatments include hydrogels, photodynamic therapy, negative pressure wound therapy and hyperbaric oxygen therapy.
- These methods stimulate epithelialization in hard-to-heal ulcers by increasing oxygenation, decrease bacterial load and enhancing healing in tissue –
- Since helpful, they do typically complement regular care rather than supplant it.
In general, diabetic feet should be treated through the complex approach of wound treatment, infection treatment, pressure reduction and even operations. Multidisciplinary care and early intervention are very effective in increasing results and diminishing chance of extreme complications. Monitoring and following treatment plans are a must because it leads to successful healing.
When to See a Doctor
You should seek medical care promptly if you notice any of the following warning signs:
- Tingling and burning sensations or pain, or abnormal loss of sensation in your feet.
- An extreme to a skin area-such as the foot is red, pale, cold, or extremely warm.
- Dry and cracked skin, especially when it is red or it bleeds between and/or on the bottom of your feet.
- Blisters, non-healing sores, ulcers or ingrown toenails (even minor ones).
- Thickened toenails yellow in color, or suspected whitish spots of the nail due to fungi.
- Obvious physical defects or figure distortions, e.g. hammertoes, fallen arches.
- The presence of infection redness, swelling, warmth, drainage, or unpleasant odor at wounds or ulcers.
Conclusion
To sum up, it is important to consider adequate diabetic foot care as a means of preventing severe complications that include infections, ulcers, and even amputation. Daily inspection of feet, ensuring good hygiene, wearing proper shoes, and keeping blood sugar level under control, provide individuals with diabetes with their best hope to avoid causing foot problems. Long-term foot health largely depends on the early diagnosis of any health issue and the subsequent visits to healthcare professionals. Call your healthcare professional now to organize a foot examination and ensure the health of your feet and well-being in general is not put at risk by the dangers of diabetic foot.