Dr Muizza Shahzad
BDS, Registered Dental Surgeon
Executive Member, LDF
Gum disease is the most widespread oral health issue in the world, with millions of people affected annually. The conditions are commonly known to stem from poor oral hygiene, plaque, and other bad habits, but the question remains whether the condition is hereditary as well. Is gum disease hereditary? There has been research that in fact, genetics can influence your susceptibility- how your body reacts to bacteria and inflammation of gums. This article will evaluate the science of the hereditary connection, the environment, and what you can do to keep your smile safe with or without gum disease in your family history.
Understanding Gum Disease
Periodontal, or gum disease, is an infection or inflammation of the bone tissue and the gums that hold the teeth. It is mainly triggered by the accumulation of dental plaque, i.e. sticky film of bacteria, as a result of poor oral hygiene. The plaque bacteria may infect the gums, causing gut symptoms like bleeding, swelling, redness, and bad breath.
Types and Stages of Gum Disease
- Gingivitis (Early Stage)
- Inflammation and swelling of the gums.
- Gums may bleed easily during brushing or flossing.
- Gums appear reddish and may be tender.
- This stage is reversible with proper oral hygiene and professional care.
- Periodontitis (Advanced Stage)
- The infection spreads below the gum line, affecting the bone that supports teeth.
- Leads to gum recession, the formation of pockets between teeth and gums, and loss of bone.
- Teeth may become loose or fall out.
- Requires professional treatment; damage at this stage may be irreversible.
- Associated symptoms include pus, bad breath, pain, and changes in tooth alignment.
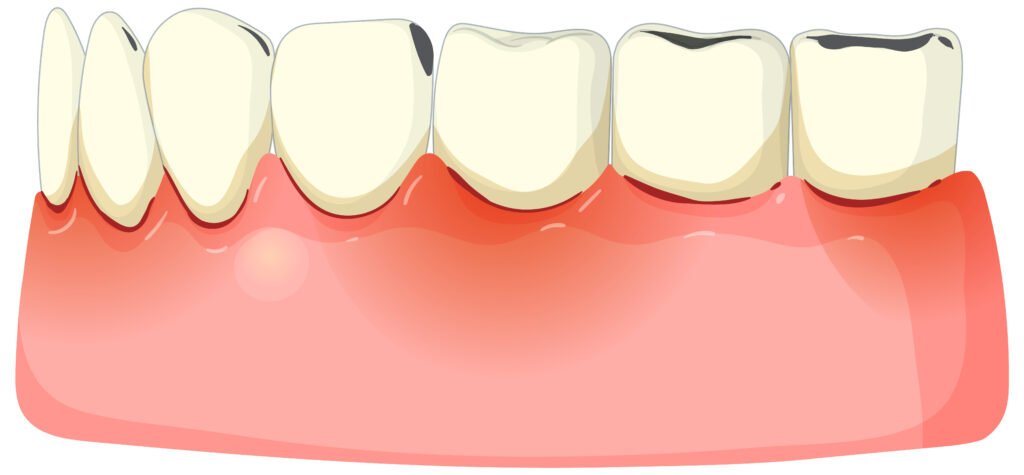
The Role of Genetics in Gum Disease
There is also a genetic contribution to the etiology and pathogenesis of gum disease (periodontal disease), in the way people react to bacterial infection and inflammation of their gums.
The main facts concerning the role of genetics are:
- Genetic Susceptibility Modulates Immune Response
Several genes determine the response of an individual to the bacteria that cause gum disease. Such as some variant of genes involved in the immune response, interleukin-1 (IL-1), interleukin-6 (IL-6), and interleukin-10 (IL-10), may result in a more vigorous inflammatory response in the gums, which heightens the possibility of tissue damage and progression to disease.
- Polygenic and Multifactorial Nature
Gum disease is a polygenic disease, implying that a lot of genes are involved, and the genetic risk is individual. The combination of these genetic defects with environmental factors, including oral hygiene, smoking, diet, and health in systemic maladies (e.g., diabetes), associates to the overall risk.
- Different Genetic Impact by Age and Disease Type
Aggressive periodontitis is more likely to have genetic factors and typically in younger people, and the progression is faster. In the elderly, chronic periodontitis is most often influenced by environmental and lifestyle factors, although genetics plays a part as well.
- Genetic Influence on Tissue and Microbial Factors
The genetic make-up can affect collagen production, therefore making gum tissue less likely to repair itself. Also, genetic predisposition may play a role in determining the kind of bacteria that grow in the mouth, thus it may lead to pathogen susceptibility to bacterial biofilms.
- Hereditary Patterns and Family History
Genetic predisposition is very significant in a family history of gum disease. Patients who have relatives with the disease are more susceptible to getting the disease as a result of inherited genetic factors that influence immunity and the condition of tissues.
- Epigenetics and Lifelong Modifications
Genetic predisposition to gum disease can also be altered by epigenetics (through DNA methylation) and other mutations that may occur during the lifetime of a person and affect the severity of the disease.
- Implications for Prevention and Treatment
The personalization of dental care comes with identifying genetic risk predictors and symptoms to offer such patients more regular check-ups, optimal medications, and therapies. It focuses on reducing inflammatory response, and genetic testing reduces the number of cases with liable persons.
Aggressive vs. Chronic Gum Disease and Heredity
Generally, aggressive and chronic gum disease (periodontitis) has the following differences:
Aggressive Periodontitis
- Development: A fast disappearance of gum attachment and bone.
- Age of Onset: In general, it will occur in younger patients (usually under age 35).
- Heredity: large genetic factor, familial clustering. It has been associated with numerous gene alterations and can occur in autosomal patterns. The important risk factor is family history. The immune response and tissue destruction are genetically prone, and it is therefore important to diagnose and treat aggressively.
- Treatment: It needs early, invasive treatment of mechanical therapy and antibiotics; in some cases, surgery is required because it acts faster.
- Risk Factors: The risks are significant with smoking and family history.
- Clinical Pattern: Like chronic periodontitis, however, bone loss and attachment loss are more rapid.
Chronic Periodontitis
- Progression: Decreased, gradual inflammatory and tissue loss.
- Age of Onset: The preponderance of adults is more than 45 years.
- Heredity: There is a genetic influence, though it is not as dominant as in aggression cases. The environmental and lifestyle factors that contribute to the disease outcome include smoking and poor oral hygiene. There is a genetic predisposition that is polygenic and multifactorial.
- Treatment: Mainly involves enhancement of oral hygiene, scaling, and root planing; may be controlled by good oral care.
- Clinical Picture: Deepening of pockets between teeth and gums is very slowly progressive as time goes by, leading to loss of bone.
- Genetics: In total, about one-third of the risk of periodontitis can be ascribed to genetic matters; the heritability is higher in severe and early-onset disease; heredity-environment relationships, such as smoking, are significant.
Environmental and Lifestyle Factors
Environmental and lifestyle factors contribute significantly to the risk of progression and severity of gum disease (periodontal disease). The main factors are the following:
- Smoking and Tobacco Use: Smoking is an environmental risk factor. Smoking kills periodontal tissue, impairs the immune system, encourages the growth of harmful bacteria, stimulates more inflammation, and leads to rapid bone loss. Smokers are found to be much more prone to getting gum disease, it is also less likely to respond once a smoker have it.
- Poor Oral Hygiene: Gum disease is commonly caused by poor brushing and flossing habits that cause the buildup of plaque. Nondisposal of plaque permits the harmful bacteria to attack the gums.
- Systemic Illness and Conditions: The presence of diseases like diabetes makes the body vulnerable to infections as well as gum disease. These conditions can be managed properly and avert risk.
- Age: The risk of getting gum disease rises with age because of plaque and other factors accumulating.
- Psychological Stress: Stressful events can change the immune response and make one more susceptible to periodontal disease, mainly through changing the virulence of bacteria and host response.
- Hormonal: Hormonal fluctuations (during puberty, before menstruation, pregnancy, menopause, and with taking oral contraceptives) make the gums more sensitive and prone to inflammation.
- Environmental Pollutants and Unsafe Living Environment: Oral health is also influenced indirectly by environmental pollution, unclean water, sanitation and cooking fuel smoke, and other indoor air pollutants, which instigate the risks of diseases in the developing world.
- Other Factors: Tooth position and malalignment may make plaque retention heightened and complicate the process of oral hygiene, elevating risk.
How to Know if You’re at Risk
To know if you’re at risk of gum disease, watch for symptoms and consider key risk factors:
Symptoms That May Indicate Gum Disease Risk
- Gums that are red, swollen, sore, or bleed while brushing, flossing.
- Gums that are off of the teeth and the teeth look longer (gum recession).
- Belly blowing bad breath or foul taste inside the mouth.
- Loose or shifting teeth, or the way your teeth fit together when you bite.
- Pooling of gums and teeth deep pockets.
- Gums pus.
- Pain or soreness when you eat.
Major Risk Factors to Be Aware Of
- Bad oral health: Failure to brush and floss daily to get rid of the plaque.
- Tobacco or smoking: This multiplies the risk and further deteriorates the results of treatment.
- Genetics: A family history of the disease predisposes gum disease.
- Age: As you mount the years, so does risk.
- Diabetes and other systemic diseases: Decrease immune response, and increase the risk of infection.
- Hormonal variations: Like in pregnancy, monthly periods, or menopause that make gums sensitive.
- Medications: Certain ones make the mouth dry or raise overgrowth of the gums.
- Stress: May inhibit the immune system and may predispose.
- Malnutrition: Sugar and carbohydrate-rich diets stimulate the growth of dangerous bacteria.
Prevention Strategies for High-Risk Individuals
In those with a high risk of gum disease, strategies to prevent progression are based on careful oral hygiene, lifestyle adjustments, and frequent professional surveillance to minimize risk and control early manifestations. The most important prevention measures of high-risk member involve:
1. Enhanced Oral Hygiene Practices
- Clean teeth and gums using clear and gentle circular motions, all the surfaces of teeth, and brush properly twice a day with the help of fluoride toothpaste.
- Use floss to clean between your teeth and along the gum line, where the action of the brush cannot penetrate, daily.
- Follow recommendations on antimicrobial mouthwash use to decrease the amount of bacteria in the mouth.
- Wash the tongue since bacteria may be deposited on the tongue, which may lead to gum problems.
2. Regular Professional Dental Care
- Visit a dentist regularly, at least twice a year, or according to recommendations you get from your dentist.
- Removal of hardened plaque (tartar) cannot be removed by brushing or flossing – hence, removal by professional cleaning.
- Through dental checkups, and particularly, periodontal tests, one can screen early before the disease advances considerably.
- Due to high-risk conditions, more visits or special periodontal treatment with the periodontist may be necessary.
3. Lifestyle and Behavioral Modifications
- Stop drinking and avoid the use of tobacco as a hazardous abuse that exacerbates the condition of the disease and healing.
- Diet needs to be balanced, with lots of fruits and vegetables, lean protein, and limited sugary, processed foods that allow bad plaque to form.
- Treat any systemic illnesses, particularly diabetes, as improper glycemic control elevates the gum disease.
- Reduce the intake of alcohol, which would help in oral inflammation.
- Relax to deal with stress, because sustained stress inhibits the immune system and increases vulnerability to gum disease.
- Having a healthy body weight by being physically active routinely, and obesity increases the risk factor.
4. Specific Preventive Measures for High-Risk Groups
- Patients with a genetic predisposition or their systemic conditions should report their risks to dentists to have an individual care plan.
- Others might require further treatment, like antimicrobial therapy or further testing.
- Monitor and immediately notify dental care providers about such symptoms as throat bleeding, swollen gums, bad breath, or loose teeth.
You may also like to read: How to Prevent Dental Plaque
Treatment Options if Gum Disease Develops
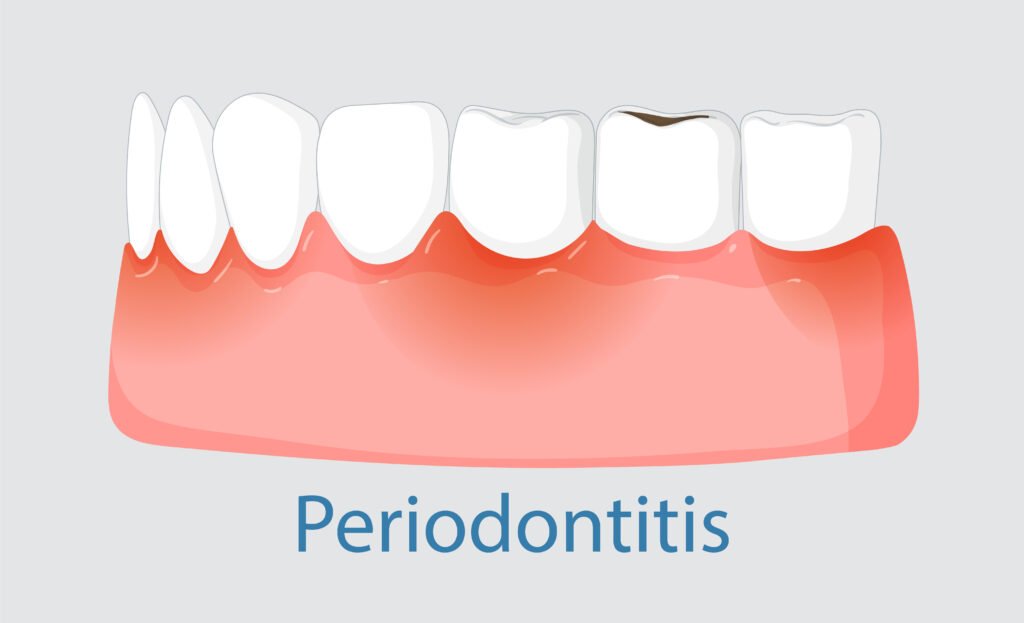
The forms of treatment of gum disease vary depending on the level and degree of the disease. The following is a breakdown of the stages of progression:
1. Early Stage (Gingivitis)
- This is the initial, reversible stage with gum inflammation and bleeding.
- Treatments include:
- Professional dental cleanings to remove plaque and tartar.
- Improved home oral hygiene: brushing twice daily, daily flossing.
- Use of antimicrobial mouthwashes.
- Gingivitis can be fully reversed with appropriate care before it progresses.
2. Mild to Moderate Periodontitis (Early Stage Periodontitis)
- At this level, there is mild to moderate attachment loss and pocket formation by infection involving supporting bone and tissues.
- Treatments include:
- Scaling and root planing (deep cleaning) to get rid of plaque and tartar under the gumline and rough root surfaces.
- Localised antibiotics or antimicrobial mouthwashes to decrease the bacteria.
- Better oral care and lifestyle changes.
- In some cases, surgery such as flap surgery is used to minimize the depth of pockets.
- Timely treatment can halt progression and potentially reverse damage.
3. Moderate to Advanced Periodontitis
- Marked by significant gum recession, bone loss, and deeper pockets.
- May involve symptoms like loose teeth, pain, and bad breath.
- Treatments become more intensive:
- Root planing and scaling in depth.
- Consumption of antibiotics, either systemic or topical.
- Flap surgery, bone grafting to regrow lost gum, and gum grafting to grow back lost gum.
- The injured tissue could also be removed using laser therapy and healing induced.
- The goal is to control infection, stop further damage, and preserve teeth.
4. Advanced Periodontitis (Severe Disease)
- Severe bone and tissue destruction, deep pockets, loose teeth, and possible tooth loss.
- Treatments focus on:
- Large volumes of surgery (pocket reduction surgery, bone grafts, and gum grafts).
- Antimicrobial treatment and other complex interventions such as laser and laser treatment.
- In other situations, removal of the badly damaged teeth and use of implants or dentures.
- Regular maintenance therapy and monitoring are critical to prevent recurrence.
Final Thoughts
Though gum disease is mostly avoidable with the help of oral care and healthy behaviors, genetics may expose you to a higher risk. It has been revealed that gum issues in the family history may increase your susceptibility to bacteria and inflammation of the gums, causing an increased likelihood of gingivitis or periodontitis. Nonetheless, genetic predisposition does not predetermine gum disease.


