Dr Muizza Shahzad
BDS, Registered Dental Surgeon
Executive Member, LDF
Maintaining a healthy smile goes far beyond having bright, white teeth. Good oral care is closely linked to overall wellness, yet many people still underestimate its importance. If you’ve ever wondered why is oral hygiene important, the answer lies in its ability to prevent common dental problems like cavities, gum disease, and bad breath, while also protecting your heart, brain, and general health. By practicing simple daily habits such as brushing, flossing, and scheduling regular dental checkups, you can safeguard not only your mouth but also your entire body.
Understanding Oral Hygiene
Oral hygiene refers to the actual process of maintaining a healthy mouth, teeth, and gums, free of dental diseases and other issues such as bad breath. Regular tooth brushing and interdental cleaning (cleaning between the teeth) are some of the key aspects of oral hygiene.
Important aspects of oral hygiene include:
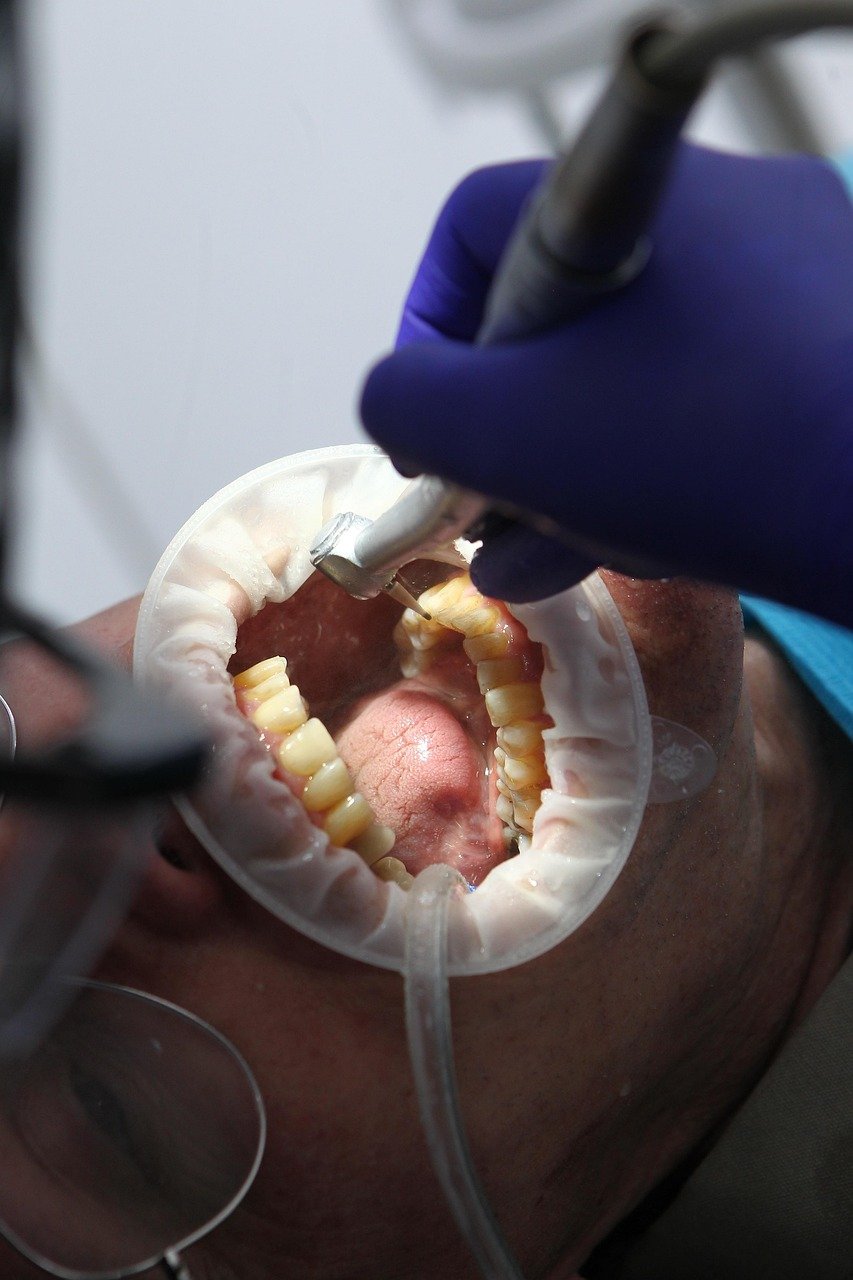
- Brushing Teeth: Brushing: Adults are advised to brush their teeth at least twice a day with fluoride toothpaste- i.e. one before going to bed at night and one after breakfast in the morning. Brushing correctly means cleaning all sides of teeth and brushing softly using small circular motions, hoping to spend at least 2 minutes per session to clean plaque off.
- Interdental Cleaning: A toothbrush can clean only the outward surfaces of teeth, and between teeth, we must clean with floss, interdental brushes, or dental tape to clean out dental plaque.
- Mouthwash: Mouthwash, either saline solutions, essential oils (e.g. Listerine), and chlorhexidine gluconate, may help to decrease plaque and inflammation of the gums. Others are short-term, as they have side effects such as staining of teeth.
- Role of Fluoride: Fluoridated toothpaste assists in preventing tooth decay by enhancing tooth enamel.
- Ventilation Story: Frequent dental check-ups and cleaning techniques by a dentist, and maintenance of oral health.
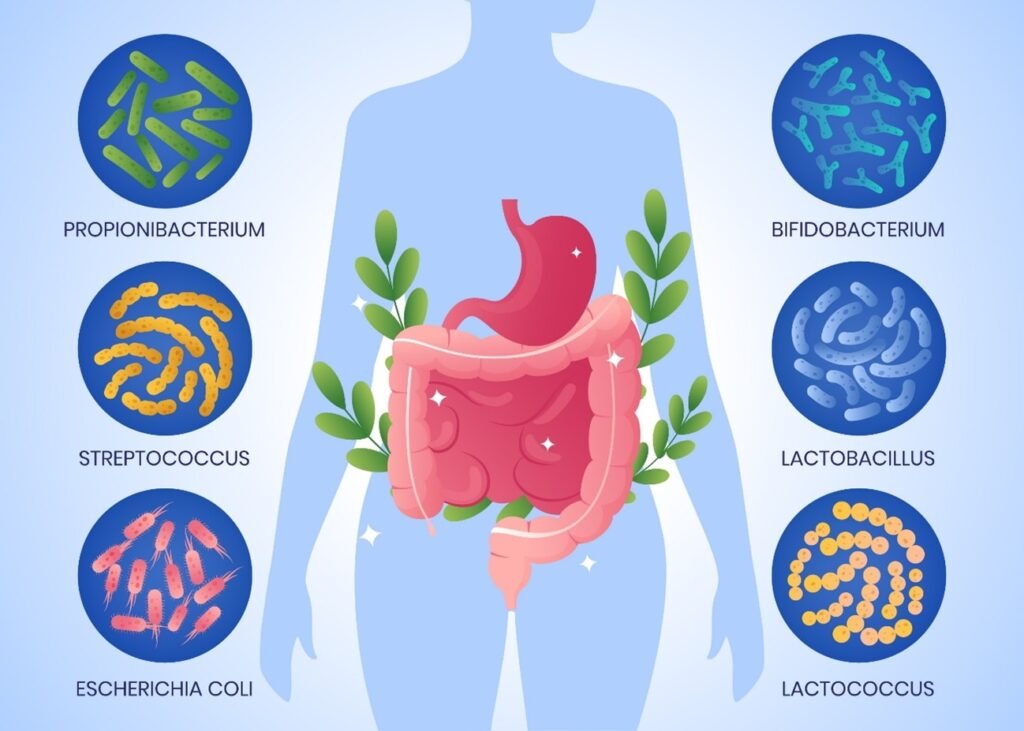
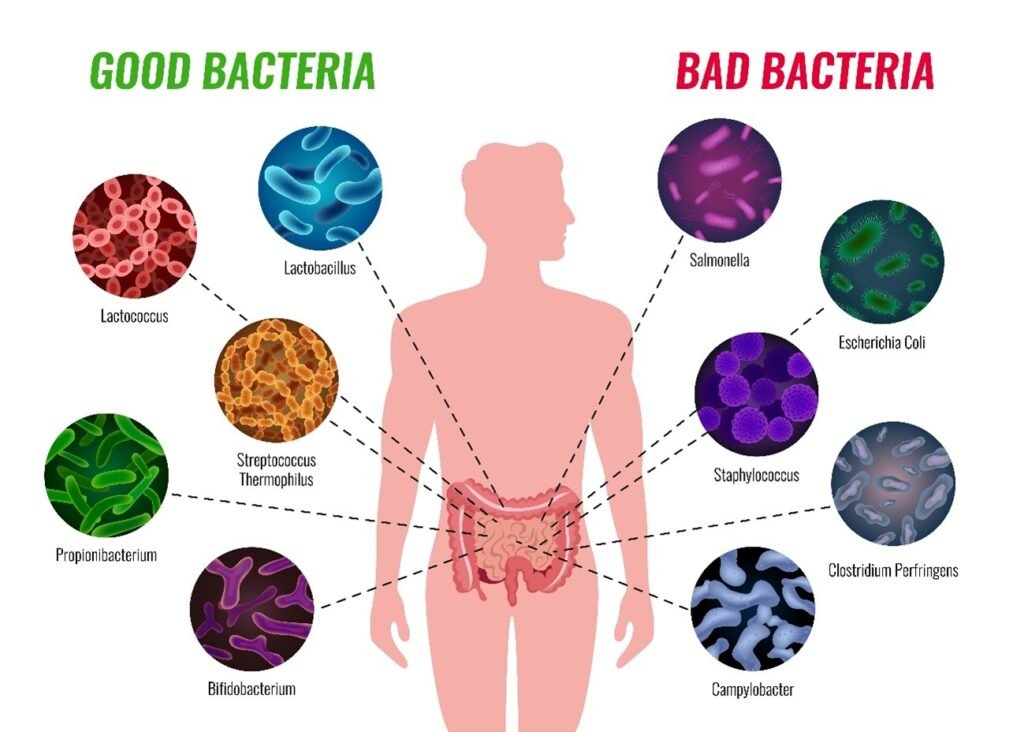
- Oral Microbiome: The ecosystem of microorganisms in the mouth plays a role in oral health. Body shifts of this balance can result in dental caries (cavities) and gum diseases like gingivitis and periodontitis.
- General Health Effects: Good mouth health is also associated with general health, which helps avoid infections that can spread to other body parts. Diseases such as diabetes and cardiovascular problems have been connected to poor oral health.
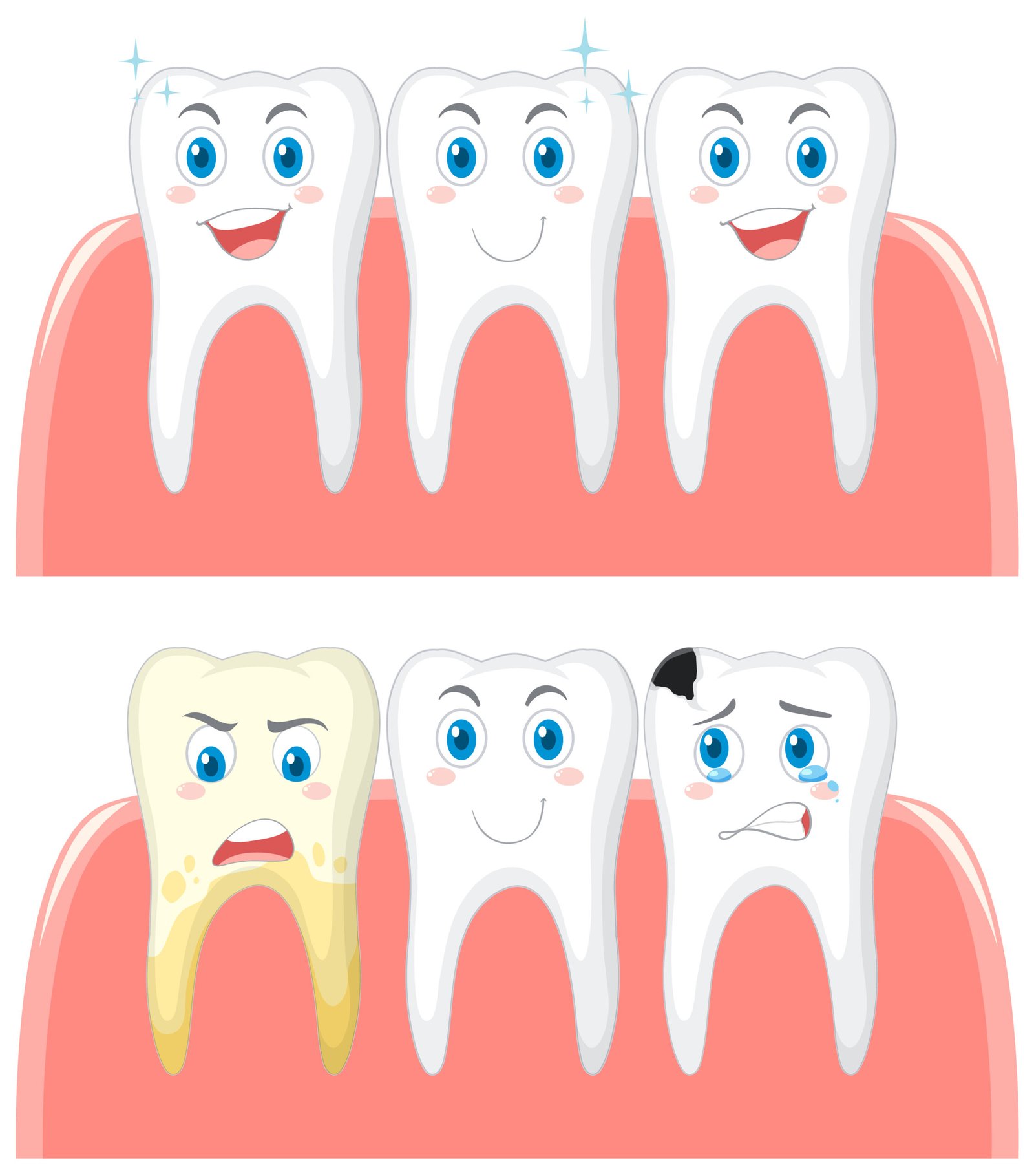
Good oral hygiene can prevent certain oral problems such as tooth decay, diseased gums, and bad breath. Such practices not only result in a healthy mouth but also result in overall well-being and quality of life because people can eat, speak, and socialize without any pain and embarrassment.
Preventing Dental Problems

The combination of good daily oral hygiene, lifestyle, and professional care is the key component to preventing dental problems. The following are the best ways to avoid general dental problems:
- Good Oral Health: Use an electric or manual toothbrush and a toothpaste with fluoride daily to brush twice to remove plaque and food debris. Clean in between the teeth (where a toothbrush cannot reach) by flossing on a daily basis. Mouthwash is also able to help reduce plaque and bacteria.
- Healthy Teeth Maintenance: Have your teeth cleaned professionally twice a year to prevent the onset of cavities or gum disease, as well as identify these problems early.
- Good Nutrition: Avoid sweet and sour food and drinks, which cause cavities and enamel loss. Drink acidic drinks using a straw so that it touches less of the teeth. Oral health is maintained by consuming a healthy diet high in vitamins and minerals.
- Avoid tobacco: Smoking increases the risk of gum disease and oral cancer by a large degree.
- Protective Treatments: Dental sealants, especially in children, act as a protective barrier on chewing surfaces and help prevent decay. Fluoride treatment may be used to make the enamel stronger resistant to attack by acid.
- Appropriate Techniques of Oral Care: Use a soft-bristle brush, brush gently and completely. Change your toothbrush every 4 months or when the bristles of frayed bristles.
- Treat Dental Trauma as Soon as Possible: Treatment of cracks and chipped teeth should be sought immediately so as to avoid infection.
- Promote Saliva output: By chewing sugar-free gum, they can boost saliva output and wash away acids and naturally clean the mouth.
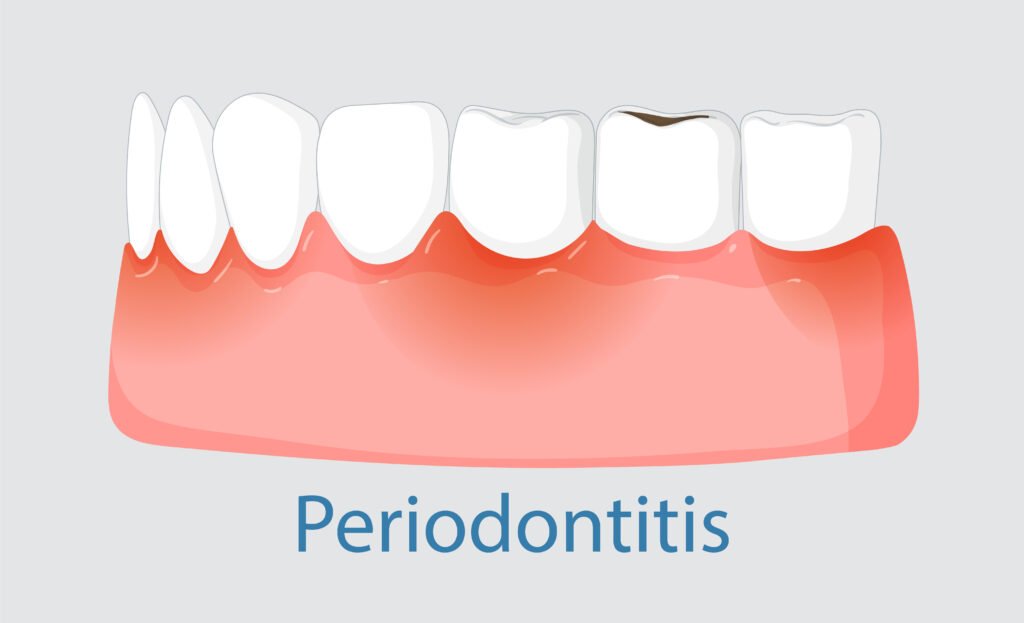
Using these pre-emptive steps, you can minimize the occurrence of cavities, gum disease (gingivitis and periodontitis), tooth erosion, and tooth infections such as a tooth abscess. Preventive dentistry not only maintains your smile, but it also prevents the long-term and expensive dental treatments later in life. Patient education and professional guidance are central in facilitating good preventive behaviors.
You may also like to read: Mouth Bacteria Metabolism Impact
Oral Health and Overall Body Health
There exist close and deep-rooted links between oral health and body health. It has been seen that oral infections particularly periodontal (gum) disease may have an impact or be associated with the onset and progression of many systemic diseases by various pathophysiological mechanisms. The following are the important aspects regarding this relationship:
- Periodontal Disease and Systemic Effects: Periodontal disease, which is a bacterial infection in the dental plaque, causes inflammation and degradation of gum tissue and bone, which support the teeth. Infections and inflammation of gums may transiently enter the bloodstream (transient bacteremia), distributing bacteria, microbial toxins, and inflammatory mediators to the body.
- Associated Systemic Diseases: Oral infections and periodontal disease have been associated with cardiovascular diseases (including heart disease), diabetes mellitus (the relationship is bi-directional, with both conditionstennis elbows prompts affecting the other), respiratory diseases, rheumatoid arthritis, adverse pregnancy outcomes, obesity, metabolic syndrome, liver disease, Alzheimer’s disease, and some cancers.
- Mechanisms of Influence: Mechanisms through which oral infections may have systemic consequences include the translocation of bacteria throughout the body, transmission of bacterial toxins, and systemic inflammation initiated by oral bacteria. These can aggravate chronic inflammation and immune responses that lead to systemic illnesses.
- Common Risk Factors and Immune Response: Genetics, smoking, diet, stress, and immune alterations are risk factors in the oral health problem and in systemic illness, providing complicated interrelationships.
- Evidence and Research: On the one hand, there is solid evidence of strong associations, but the causality is still being elucidated in continuous research. Periodontal disease treatment has also been found useful in systemic diseases such as diabetes.
- Clinical Significance: Dental care is part of health care. Good oral care and dental hygiene can lower the possibility or severity of body illnesses
Final Thoughts
In summary, the answer to why is oral hygiene important goes far beyond keeping your teeth clean. Proper oral health can prevent dental cavities, gum disease, and bad breath, and reduce the potential of dangerous conditions like heart disease, diabetes complications, and even dementia. It helps self-esteem, quality of life, and confidence, in addition to the physical benefits. When you brush, floss, eat a balanced diet, and see the dentist regularly, you not only make a positive investment in a better mouth, but you also invest in a stronger body. Caring about your mouth health today is one of the easiest ways to care about your future health.