Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
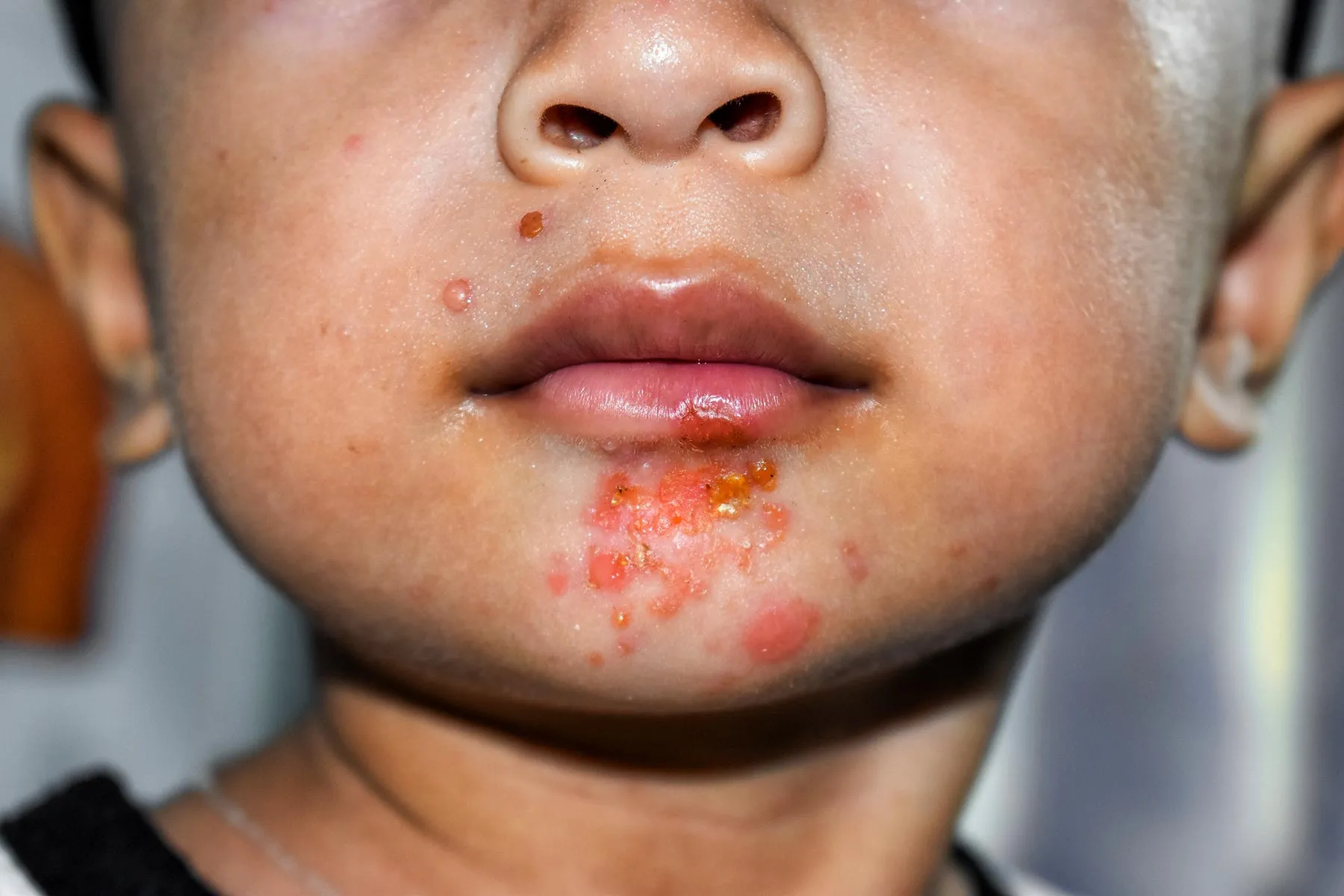
Impetigo is an infectious and widespread skin disease that occurs both in children and in adults, but in young children, it occurs most frequently. It starts with red sores/blisters and within a short time they become widespread and develop honey colored crusts often on the nose, mouth, hands or even on the open skin. Although impetigo might appear frightening, it is most often mild and is responsive to treatment at an early stage. It is important to know the causes, symptoms, and prevention measures to prevent the spread of the infection and guarantee a rapid cure.
What Is Impetigo?
Impetigo is a widespread, highly contagious bacterial dermatological infection of the epidermis. It occurs most commonly as itchy or painful sores and blisters that burst and leave yellowish or honey-colored crusts particularly on the face, arms, and legs. It is very common in young children between 2 to 5 years old but maybe at any age. Staphylococcus aureus or Streptococcus pyogenes bacteria cause the infection. Transmission of impetigo occurs readily by contact, particularly when there is a large crowd or the skin is torn by wounds, insect bites, or eczema. Therapy typically involves topical or oral antibiotics, and recovery tends to be without scarring. Most common forms include non-bullous impetigo (with tiny blisters and crusting), bullous impetigo (large blisters filled with fluid), and ecthyma (ulcers and severe).
Types of Impetigo
The main types of impetigo are:
- The most common is non-bullous impetigo (also known as crusted impetigo). It begins with small blisters which burst rapidly, producing red wet spots of skin that form a yellowish-brown or honey-like crust. It normally appears near the mouth, forearms, nose, and hands. Staphylococcus aureus or group A streptococcus bacteria is the cause of most cases.
- Bullous impetigo results in greater fluid blisters that can be left intact. These blisters tend to be transparent or opaque and are common to the trunk, arms, and legs, particularly among infants and very young children. It is only caused by Staphylococcus aureus, which produces a toxin that causes the upper layer of skin to separate.
- A more serious and infrequent type is called ecthyma. It produces painful, pus-filled ulcers that go deeper into the skin under the surface, encircled by yellow or brown-black crusts. Ecthyma may leave scars and is a common complication of untreated impetigo.
Thus, impetigo includes these distinct forms: non-bullous (crusted), bullous (blistering), and ecthyma (ulcerative).
Causes and Risk Factors
Bacteria, particularly Staphylococcus aureus and group A Streptococcus (Streptococcus pyogenes) are the most common cause of impetigo. These bacteria enter the skin via breaks like cuts, scratches, insect bites, or any other trauma of the skin. Transmission occurs by direct contact with the sores of an infected individual or by indirect contact through contaminated towels, clothing, or bedding.
Key risk factors that increase the likelihood of developing impetigo include:
- Children between 2 and 5 years old because their immune system is not fully established.
- Residing in humid climates, which promotes the growth of bacteria.
- Open wounds or any other skin disorders like eczema, dermatitis, scabies, insect bites or infectious dermatitis.
- Bacterial spread is enabled by close living or playing conditions, like in schools, daycare centers or crowded areas.
- Poor hygiene and lack of hand, body or face washing.
- Weakened immune system or underlying health problems, including diabetes, HIV / AIDS, cancer therapies, liver or kidney issues, or injecting drugs.
Secondary impetigo may occur when the bacteria infect an already existing skin wound. Trauma, burns, scratching, and any other type of skin injury act as entrances to bacteria. Impetigo can cause complications without treatment, and it is extremely contagious when there are blisters or sores.
Symptoms of Impetigo
Impetigo symptoms vary slightly depending on the type but generally include:
- Blisters or reddened sores, usually of the area around the mouth and nose, but they may occur anywhere on the body, particularly on the face, arms, and legs.
- The sores can begin as tiny blisters, which can be itchy or painful and then burst, releasing fluid or pus.
- These ruptured blisters then develop an archetypal yellowish or honey-colored scab or crust.
- Scratching or touching may cause the spread of the rash to other parts of the body or nearby.
- The clusters of blisters may become larger and larger.
- Under the crust the affected skin can be moist and reddish.
- Bigger fluid-filled blisters are present in bullous impetigo, which break, leaving crusted sores, which tend to be more painful and swollen.
- A more severe form is called ecthyma and results in painful sores that go deeper into the skin with thick crusts and can leave behind scars.
- In more serious cases, some individuals can have swollen lymph nodes in the region or a mild fever.
- Itching and soreness are frequent but mild as a rule.
You may also like to read: Rhinovirus
How Impetigo Spreads
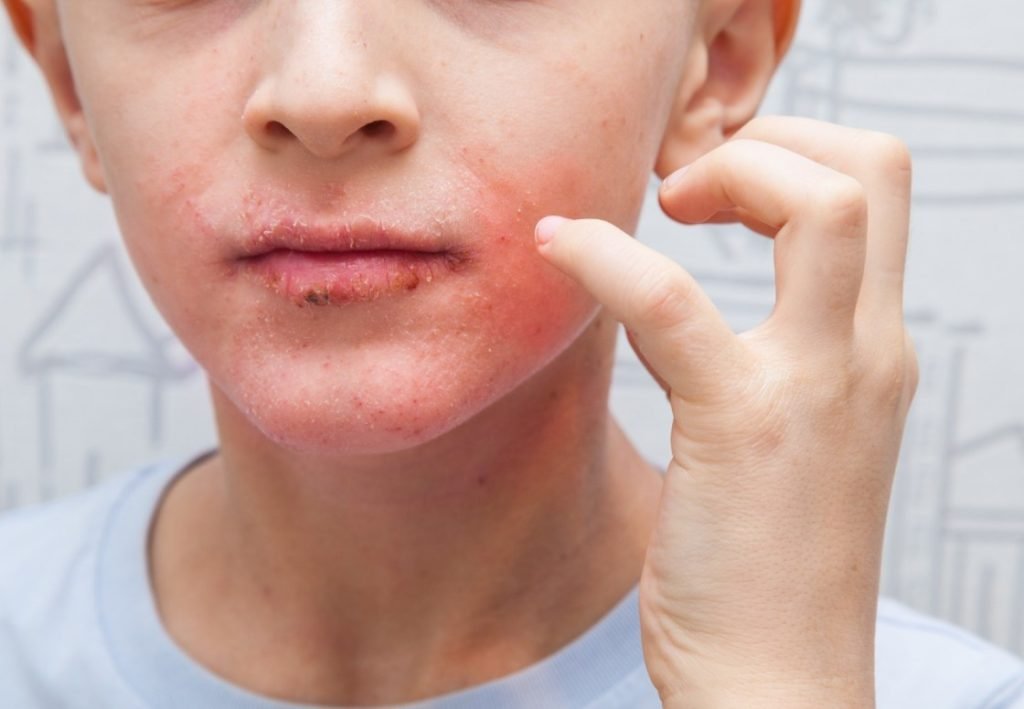
The transmission of impetigo occurs primarily during direct physical contact with an infected individual, particularly the sores, the blisters or the crusted lesions. It might also propagate indirectly by contact with substances contaminated with the bacteria, such as towels, clothing, bedding, toys or sports equipment. The bacteria causing it- Staphylococcus aureus and Streptococcus pyogenes can survive on these surfaces to infect others.
The other spread factors are those in close contact such as schools, daycare centers, gyms, and sports teams, in particular wrestlers and athletes with a lot of skin contact. Cuts, scrapes, insect bites, or skin diseases like eczema weaken the skin’s defenses by allowing the entry of bacteria.
Impetigo bacteria might also be transmitted through respiratory droplets through coughing or sneezing, and contact with the mucous membranes or skin.
Infection is contagious until the sores are completely cured and the crusts dry out. Hygiene, not sharing personal objects, covering sores, washing hands frequently, and disinfecting surfaces are useful in preventing transmission.
Diagnosis
The diagnosis of impetigo is mostly based on a history and physical examination. Impetigo is normally diagnosed by a healthcare provider looking at the typical look of the sores, blisters, and crusts on the skin-honey-colored crusts in non-bullous impetigo or bigger, fluid-filled blisters in bullous impetigo. The location and nature of lesions are important diagnostic indicators.
Additional diagnostic methods include:
- Bacterial culture or swab in the pustules, blisters or crusts may be obtained when there is a suspicion of antibiotic resistance (e.g., MRSA), or when the patient does not respond to conventional therapy. This assists in determining the causal bacteria and in informing the selection of antibiotics.
- A rare but possible use of skin biopsy is with refractory or atypical cases.
- Impetigo is not regularly tested with serologic tests of streptococcal antibodies but could be helpful in the event of post-streptococcal complications.
- Lab testing is not typically required as impetigo diagnosis can be determined through clinical examination.
Differential diagnosis includes other blistering or crusting skin conditions like eczema, herpes simplex, insect bites, contact dermatitis, and fungal infections, so careful skin examination is important.
Treatment Options
The treatment options for impetigo include both topical and systemic antibiotics depending on the severity and extent of the infection.
- Topical antibiotics are the first option to localized, simple non-bullous impetigo. Topical agents are typically mupirocin, retapamulin, and fusidic acid (not in every country). The crusts must be washed with soap and water before using them to ensure maximum medication absorption.
- In the case of bullous impetigo, non-bullous impetigo with over five lesions, deep tissue involvement, or systemic (fever, lymphadenopathy) signs, oral antibiotics are prescribed. Typical oral antibiotics are cephalexin, dicloxacillin or amoxicillin-clavulanate. In case culture demonstrates the presence of methicillin-resistant Staphylococcus aureus (MRSA), clindamycin, doxycycline, or trimethoprim-sulfamethoxazole can be used in place of it.
- General hygiene should also be adhered to: it is important to keep lesions clean, cover sores with bandages to prevent transmission, wash hands regularly, wash clothes and linens, and not to interact with other people during contagious periods.
- The average length of treatment is 5-10 days, and the patient must continue the full course despite symptom improvement to avoid resistance and relapse.
- In recurrent or chronic cases, bacteria carried in the nose is tested and treated with mupirocin nasal ointment.
- In the case of small, minor diseases, over-the-counter antibiotic creams like bacitracin can be tried, although prescription antibiotics usually work better.
Final Thoughts
Impetigo can be a very contagious skin infection that can be effectively treated with proper awareness, early diagnosis and prompt treatment. The right care clears most of cases in a few weeks with no long-term consequences. The best way to control its spread is by practicing good hygiene, not sharing personal items, and seeking medical assistance whenever symptoms emerge. Knowing the causes, symptoms, and prevention, children and adults can remain safe and get through impetigo soon.