Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Graves disease is an autoimmune disease that makes the thyroid gland overproduce a hormone and results in hyperthyroidism. It is a thyroid disorder that is one of the most prevalent in the world, and mostly among women. The condition may lead to a plethora of symptoms, including weight loss and rapid heartbeat, eye issues, and skin alterations. It is important to know its causes, signs, and treatment options to manage it and live a better life.
What is Graves Disease?
Graves Disease is an autoimmune condition that mainly attacks the thyroid gland, making it overactive (so-called hyperthyroidism). The immune system in this disease forms antibodies known as thyroid-stimulating immunoglobulins (TSI) incorrectly and binds to the thyroid-stimulating hormone (TSH) receptors, which causes the thyroid to secrete too much thyroid hormone. This excessive production stimulates the body’s metabolism and results in numerous symptoms and health problems. In some cases, it may involve the eyes and the skin.
Key Points About Graves Disease:
- It is a chronic autoimmune hyperthyroidism.
- It is characterized by weight loss, fast heart rhythms, irritability, fatigue, heat intolerance, muscle weakness, eye symptoms, like bulging eyes (Graves’ ophthalmopathy).
- Thyroid gland usually swells, which is referred to as goiter.
- It predominates in women over men and is commonplace in the age range of 30-60 years.
- The exact etiology is uncertain but it is associated with genetic and environmental factors, with a family history predisposing.
- Unchecked, it may cause severe complications such as heart and bone issues.
Causes and Risk Factors
Graves Disease is an autoimmune disorder triggered by both genetics and the environment.
Causes:
- Autoimmune response: The immune system secretes thyroid-stimulating immunoglobulin (TSI) antibodies that imitate thyroid-stimulating hormone (TSH), which causes the overproduction of thyroid hormone.
- Genetics: Graves Disease has a genetic predisposition, and some variations of certain genes (including human leukocyte antigen DR3 and other genes associated with the immune system) predispose people to having the disease. It is also familial and prevalent in identical twins compared to fraternal twins.
- Environmental triggers: Potential environmental triggers of the disease among genetically-prone individuals are infection (viral or bacterial), excess of iodine, emotional stress, smoking, pregnancy (particularly postpartum), exposure to certain medications or therapies, including interferon alfa or highly active antiretroviral therapy (HAART).
Risk Factors:
- Family history: Family history of Graves Disease or other autoimmune disease increases the risk.
- Sex: Women are much more prone to Graves Disease than men.
- Age: It mostly happens in the age band 20 to 50 but it can also affect other ages.
- Other autoimmune conditions: Individuals with autoimmune diseases like type 1 diabetes, rheumatoid arthritis, autoimmune gastritis, and vitiligo are at increased risk.
- Smoking: Cigarette smoke is a risk factor, and it also exacerbates Graves ophthalmopathy (eye involvement).
- Pregnancy/post partum: The disease may be triggered by hormonal changes during and after pregnancy.
- Stress: The immune response can result from emotional or physical stress.
The intricate interplay of these genetic predispositions and environmental factors leads to the development and progression of Graves Disease.
Signs and Symptoms of Graves Disease

Graves Disease causes a range of symptoms primarily due to overactive thyroid (hyperthyroidism) and can also affect the eyes and skin.
Hyperthyroidism Symptoms
- Weight loss despite increased appetite
- Rapid or irregular heartbeat (palpitations)
- Nervousness, irritability, anxiety
- Tremor or shaking hands
- Fatigue or muscle weakness
- Heat intolerance and excessive sweating
- Trouble sleeping (insomnia)
- Frequent bowel movements or diarrhea
- Enlarged thyroid gland (goiter), visible as swelling in the neck
- Changes in menstrual cycles and sexual dysfunction
Eye-related Symptoms (Graves’ Ophthalmopathy)
- Bulging eyes (exophthalmos)
- Puffy or irritated eyes
- Gritty or watery eyes
- Sensitivity to light
- Pressure or pain in or around the eyes
- Redness and swelling of eyelids
- Blurred or double vision
- Eyelids may retract or fail to close completely
Skin-related Symptoms (Less Common)
- Thickening and redness of skin, typically on the shins (Graves’ dermopathy)
- Clubbing of fingers and toes (thyroid acropachy; rare)
The symptoms may take many weeks or months to commence, occasionally days. One-third of individuals with Graves Disease develop eye problems. It is exquisitely sensitive to skin symptoms and finger clubbing. Since the symptoms involve several systems, diagnosis and treatment are needed.
Complications
If Graves Disease is left untreated, it can lead to serious complications affecting various organs and systems in the body:
Complications of Untreated Graves Disease
- Thyroid Eye Disease (Graves Ophthalmopathy): It may lead to serious eye conditions such as bulging eye, eye dryness, irritation, and in severe cases, blindness.
- Heart Problems: Excess thyroid hormone causes the heart to overwork and overexert itself, and it may result in:
- Irregular heart rhythms (arrhythmias)
- Rapid heartbeat (tachycardia)
- Heart failure due to the heart’s inability to pump effectively
- High blood pressure and increased risk of stroke and blood clots
- Thyroid Storm: It is a life-threatening disorder in which the levels of thyroid hormones abruptly and drastically grow. High fever, vomiting, diarrhea, delirium and coma are symptoms of the disease. This is a life-threatening medical emergency.
- Goiter: The thyroid can become very big resulting in the swelling of the neck and potentially inability to swallow, breathe, or voice.
- Osteoporosis (Brittle Bones): Oversupply of thyroid hormone results in rapid bone degradation, exposing a person to fractures, particularly in postmenopausal women.
- Pregnancy Complications: Untreated Graves Disease during pregnancy may lead to miscarriage, preterm labor, fetal growth retardation, preeclampsia, maternal heart failure.
- Blood Disorders: Pancytopenia (low blood cell levels) and agranulocytosis (low white blood cells) are rare complications, which make the risk of infections higher.
- Skin Problems: Some cases have thickened, red skin (pretibial myxedema), mostly on the shins.
Without treatment, the risk of these complications increases, highlighting the importance of early diagnosis and management of Graves Disease to prevent severe health consequences.
Diagnosis
The clinical examination is the basis of diagnosis of Graves Disease with the help of laboratory and imaging diagnostic tests.
Clinical Examination:
- Physical symptoms like an enlarged thyroid gland (goiter), fast heartbeat, tremor and the Graves eye signs (exophthalmos and eye swelling) are examined.
- Symptoms of hyperthyroidism include weight loss, heat intolerance and nervousness.
Blood Tests:
- Thyroid hormone levels: TSH is typically very low or not measurable at all because it is inhibited by excess thyroid hormone.
- Free T4 and Free T3: High levels are a positive evidence of hyperthyroidism.
- Thyroid antibodies: Thyroid-stimulating immunoglobulins (TSI) or TSH receptor antibodies are a strong indication of Graves Disease.
- Autoimmune thyroid disease may also be assessed by antibodies to thyroid peroxidase (TPO) and to thyroglobulin.
Radioactive Iodine Uptake (RAIU) Test:
- Radioactive iodine in small doses is given, and a scan is done to check the absorption of iodine by the thyroid.
- The diffuse uptake of iodine is normally high in Graves Disease, which can help distinguish it among the causes of hyperthyroidism.
Imaging:
- Doppler thyroid ultrasound can be done to assess the size, structure, and circulation of the gland.
- In cases of Graves ophthalmopathy eye imaging (ultrasound, CT scan, MRI) can be utilized to check the eye muscle swelling and orbital involvement.
Additional Tests:
- In atypical or complex cases, further testing or consultation with endocrinologists may be required.
- Biopsy of the thyroid is rarely needed.
The combination of these clinical signs, hormone tests, antibody tests, and radioactive iodine uptake has enabled a good diagnosis of Graves Disease and separation from other thyroid conditions.
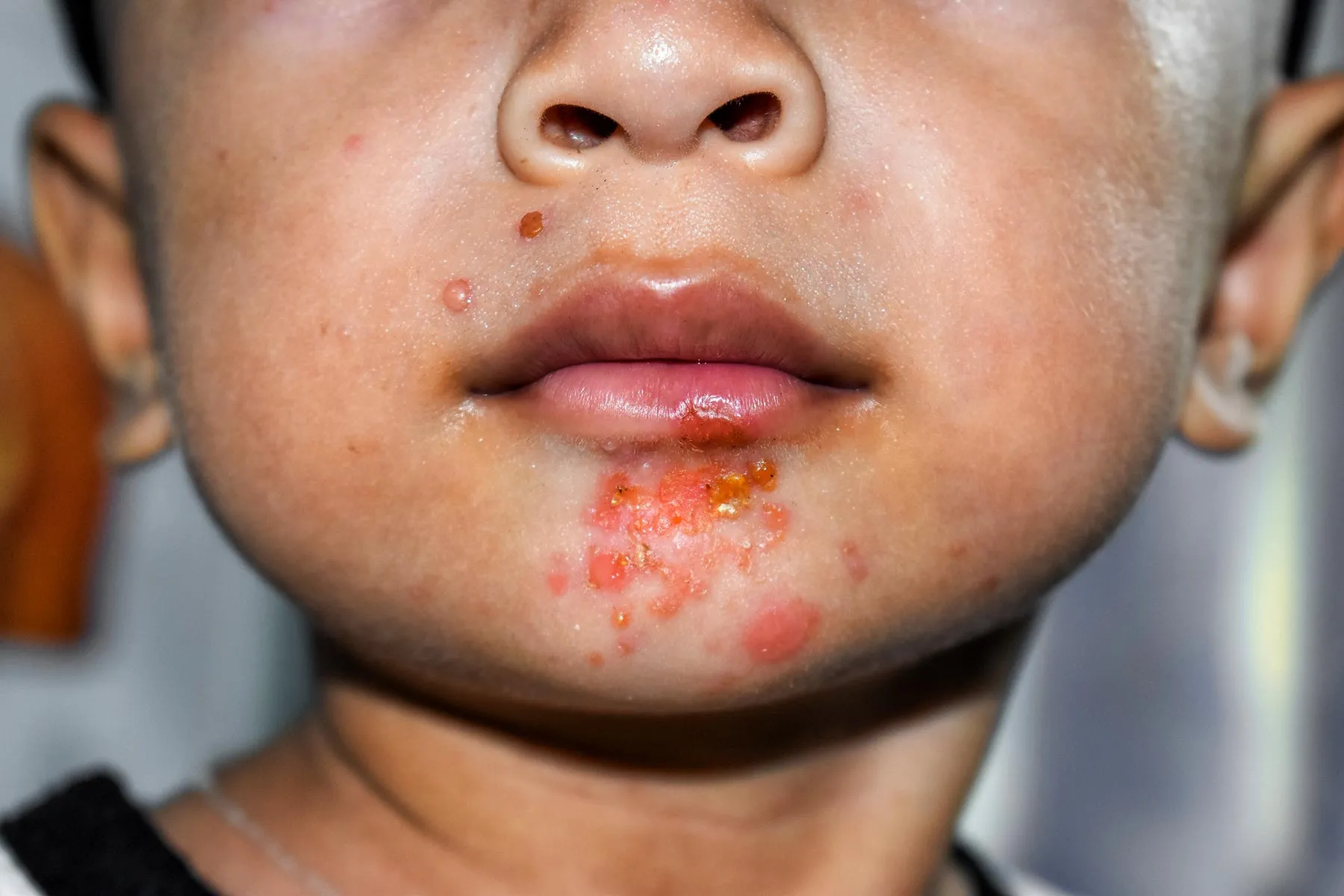
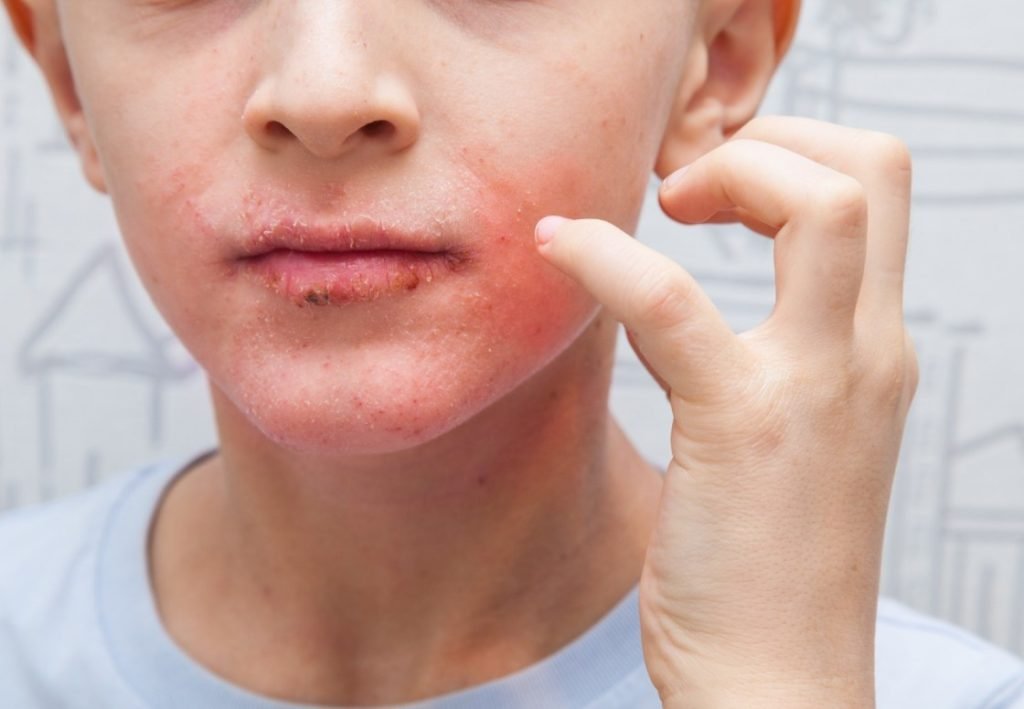
You may also like to read: Impetigo
Treatment Options
Graves Disease treatment options are intended to regulate the excessive production of thyroid hormone, alleviate the symptoms, and avoid complications. The major lines of treatment are medication, radioactive iodine therapy and surgery.
Medications
- Antithyroid Drugs: Methimazole and propylthiouracil (PTU) are widely used to inhibit the production of thyroid hormones. Methimazole is used unless in pregnancy, in the first trimester, PTU is better. Assessing remission often takes 12-18 months, although treatment can require some patients more time. Side effects may include rash, sore joints, liver issues and a rare possibility of low white blood cell count.
- Beta Blockers: These do not influence thyroid levels but are useful in managing such symptoms as rapid heartbeat, tremor, anxiety and heat intolerance. Widespread beta blockers are propranol and atenol.
Radioactive Iodine Therapy (RAI)
- Radioactive iodine (I-131) is administered orally, and over weeks or months destroys overactive thyroid cells causing reduced synthesis of thyroid hormones.
- RAI is a definite therapy that is usually applied when medication fails or in cases of recurrence.
- It usually leads to hypothyroidism in the future, which needs lifelong replacement of thyroid hormones.
- It is mostly not used during pregnancy and breastfeeding.
- It can aggravate or cause thyroid eye disease in patients.
Surgery
- Thyroidectomy: This is surgical removal of the entire or part of thyroid gland.
- Surgery can be suggested when the patient is unable to bear antithyroid medicines, has large goiters that lead to compression and in those with severe eye disease.
- Patients should be put on lifelong thyroid hormone replacement therapy after surgery.
- Damage to the parathyroid glands (calcium levels) and injury to the vocal cord nerve are the risks, but they are not common in the hands of skilled surgeons.
Choosing Treatment
- Treatment is determined by patient factors such as age, severity, pregnancy, eye involvement, and patient preference.
- Others can begin with medications to stabilize, followed by final treatments such as RAI or surgery.
- Follow-up is necessary to make changes to therapy and complications management.
Lifestyle and Self-Care Tips
Lifestyle and self-care is a supportive aspects to treat Graves Disease along with medical treatment. Major guidelines to enhance the well-being and symptom control are:
Stress Management
- Use relaxation methods like deep breathing, meditation, journaling or your pleasure causes.
- Learn to say no and manage time to reduce stress, do not overload oneself.
- Mood wellness promotes immune homeostasis and may assist with symptoms.
Healthy Sleep and Rest
- Make getting adequate and regular sleep a priority in order to fight fatigue and enhance general health.
- Do not stay up late or wear oneself out.
Diet and Nutrition
- Consume a healthy diet full of antioxidants in fresh vegetables and fruits to alleviate inflammation.
- Take a sufficient amount of calcium and vitamin D to maintain bone strength and prevent osteoporosis.
- Add protein-rich foods such as fish, poultry, eggs, and plant proteins to build muscle.
- Restrict or watch the intake of iodine as recommended by a medical professional, as too much of iodine may increase symptoms.
- Limit caffeine-based products (coffee, tea, chocolate, soft drinks), which can aggravate palpitations and anxiety.
- Avoid foods that are highly processed, include sugars, and solid fats; eat whole grains, olive oil, and baked or broiled items.
Exercise
- Do light exercise every day.
- Do not overexert, particularly when the heart rate is high.
Social Support and Advocacy
- Get family, friend, or support group support.
- Educate yourself on the disease and promote proper care.
Other Tips
- Adhere to medical regimens.
- Smoking should be avoided because it aggravates Graves eye disease.
- Check with health practitioners on thyroid levels and symptoms regularly.
The lifestyle changes can alleviate symptoms, enhance quality of life, and complement the medical therapy of Graves Disease.
Final Thoughts
Graves disease is a complicated autoimmune disorder of the thyroid and may cause severe health problems when unchecked. Majority with early diagnosis, appropriate treatment, and lifestyle changes can easily control their symptoms and lead a good life. Monitoring and collaborating with medical professionals is the principle of managing Graves disease and avoiding chronic problems.