Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Paralysis refers to severe illnesses which result in loss of muscles in any or all parts of the body. It arises when the linking of the brain and the muscles are impaired by nerve damage, spinal cord injury or neurodegenerative diseases. Understanding the different types of paralysis—from monoplegia affecting a single limb to quadriplegia involving the entire body—is essential for recognizing symptoms and seeking timely treatment. This article will discuss the primary types, causes, and the existing therapies to assist in creating awareness and assistance to help those affected.
What Is Paralysis?
Paralysis is the inability of a section of your body to use its muscles due to an issue with the nerve messages that connect your brain and your muscles. It may be transient or permanent and may affect any part of the body.
Main Types of Paralysis
The most common forms of paralysis are classified according to the affected area of the body or the effect on muscle tone.
Types by affected body part
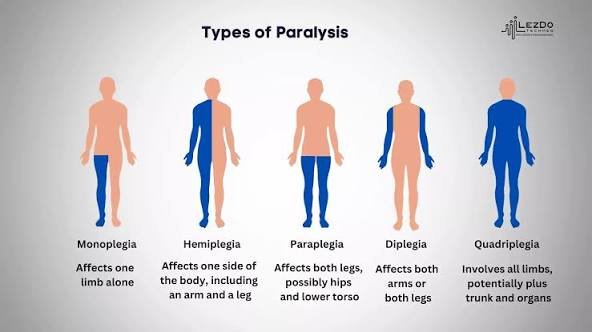
- Monoplegia: It involves only one limb, e.g. one arm or one leg.
- Hemiplegia: This occurs in an arm and a leg that are on the same side and can as well affect the face. Stroke often leads to hemiplegia.
- Paraplegia: It is one that involves both legs and in some cases the torso. It is normally due to a spinal cord injury at the thoracic area, lumbar or sacral.
- Quadriplegia (or Tetraplegia): This refers to any loss of movement in all 4 limbs (both arms and both legs) as well as in the torso. It is brought about by a high injury of the spinal cord, normally the neck.
- Diplegia: This affects the same side of the body on both sides, like both legs or both sides of the face.
- Locked-in syndrome: This is a very rare disorder, which an individual loses all of his or her muscles except those controlling eye movement.
Types by muscle tone
- Flaccid paralysis: Muscles are weak and limp as they can even slump. This occurs when nerves that trigger the muscles are killed. Flaccid paralysis was a typical symptom of polio.
- Spastic paralysis: The involuntary jerks or spasms cause tightening and stiffness of the muscles. It is a result of the destruction of upper motor neurons which relay brain signals to spinal cord. Cerebral palsy is known to cause spastic paralysis.
Causes of Different Types of Paralysis
Different forms of paralysis are as a result of damage to the nervous system which impairs the ability to communicate between the brain, the spinal cord and the muscles. The nature and location of this damage can define the areas of the body that are impacted and the response of the muscles.
The causes of different types of paralysis vary depending on which type is involved:
- Monoplegia: This is usually due to cerebral palsy, brain, spinal cord, or limb injury or trauma. Others are stroke, tumor, inflammation of the nerve, neuropathy, multiple sclerosis, single-limb motor neuron disease.
- Hemiplegia: It is typically due to brain injury or spinal cord injury (cerebrovascular accident), transient ischemic attacks, intracranial hemorrhage, brain trauma, brain tumor, cerebral palsy, encephalitis, multiple sclerosis, and other diseases of the nervous system.
- Paraplegia: This is typically caused by either a spinal cord injury or disease of the thoracic, lumbar, or sacral portion. The causes are spinal cord trauma, tumors, infections, multiple sclerosis, lupus myelopathy, congenital malformations such as spina bifida, metabolic disorders, and cerebral palsy.
- Quadriplegia (tetraplegia): The greatest cause is neck region spinal cord injury, trauma to the brain, nontraumatic brain damage, muscular dystrophies, stroke, cerebral palsy, and spinal cord or brain pathology.
- Diplegia: It is frequently linked with brain damage or cerebral palsy before, during or soon after birth. Genetic predispositions, maternal infections, toxin exposure; perinatal/postnatal causes such as oxygen deprivation, meningitis, traumatic brain injuries, and vascular disorders affecting brain regions that perform motor control.
Symptoms and Diagnosis

The symptoms of paralysis may include the inability to move a limb to the absence of muscle control. Symptoms may be immediate, as with a stroke or spinal injury or may develop over time with such conditions as multiple sclerosis.
Primary symptoms
- Weakness of muscles: This is the most prevalent symptom. It may be total paralysis of the stricken part or partial paralysis, which is paresis.
- Changes in sensation: A lot of individuals who have paralysis lose sensation in part or all of the injured part.
- Abnormal muscle tone: This depends on the type of paralysis.
- Flaccid paralysis: Causes muscles to become weak and limp.
- Spastic paralysis: Causes muscles to become tight, stiff, and prone to involuntary jerks or spasms.
Associated symptoms
- Numbness or tingling in the limbs
- Muscle cramps
- Changes in sexual function
- Loss of bowel or bladder control
- Difficulty with balance or walking
- Trouble breathing, speaking, or swallowing, especially with high spinal cord injuries
- Pain or a stinging sensation caused by nerve damage
Diagnosis of paralysis
Diagnosis of paralysis is done by firstly confirming that the muscle control is lost and then finding the cause and the extent of the problem.
Initial evaluation
- Physical examination: A medical professional will conduct a complete neurological check-up, which involves determination of muscle strength, muscles, reflexes, tone, and sensation.
- Medical history: The doctor will enquire as to when the symptoms started, when the injuries were suffered, or the medical conditions that might be involved.
Diagnostic tests
- X-ray: Utilised to detect fractured bones or any other skeletal conditions that may be leading to nerve damage.
- Imaging scan (CT and MRI): This will give out-of-depth images of the brain, the spinal cord, and adjacent tissues. They can show symptoms of a stroke, a spinal cord injury, or other nerve damage.
- Myelogram: Refers to a procedure where a special dye is injected into the spine column to identify the spinal cord and nerves on X-ray, CT or MRI.
- Electromyogram (EMG) and Nerve Conduction Study (NCS): This is the test of electrical activity of nerves and muscles. They are able to assist a physician in deciding whether the problem is a muscle problem or nerve injury.
- Spinal tap (lumbar puncture): A cerebrospinal fluid is taken and examined to avert any infection, inflammation, or ailment such as multiple sclerosis.
- Blood tests: Could be performed to seek signs of inflammation or infections; other underlying conditions.
Treatment and Rehabilitation
The aim of treatment and rehabilitation of paralysis includes the maximum residual functioning, avoidance, and quality of life. Complete paralysis is incurable nowadays, although therapies that encourage recovery and adaptation have helped many.
Treatment Approaches
- Physical therapy is designed to enhance muscle strength, range of motion and mobility using specific exercises. It also assists in muscle length and joint performance to avoid contractures and stiffness. Neuroplasticity or the capacity of the nervous system to rewire and adapt is promoted by task specific and repetitive exercises.
- Occupational therapy aims at assisting one to feel independent in daily life activities like dressing, eating, grooming, and work. Therapists instruct adaptive skills, prescribe assistive aids and joint protective measures.
- Drugs can be taken to treat either spasticity or pain, or inflammation of the muscles due to paralysis.
- In other instances, surgery such as nerve repair, nerve transfer, or amputation can be taken into consideration depending on the cause of paralysis and its severity.
- New treatment methods are stem cell therapy to repair the damaged nerve tissue and epidural electrical stimulation to aid recovery of voluntary motion below the level of injury. Brain-computer interfaces and robotics are also potential technologies being developed.
You may also like to read: Cardiometabolic Disease
Rehabilitation Focus
The rehabilitation programs focus on neuroplasticity with intensive training and exercise of the injured muscles and nerves, which can restore some motor control even many years post-injury.
- Physical therapies can be enhanced by using mental practice, electrical stimulation, and other measures such as acupuncture.
- Social and emotional support should be discussed to overcome the psychological effects and promote active involvement in recovery.
On the whole, the treatment plans are multidisciplinary and individualized, involving physical and occupational therapy, medical therapy, and the latest technologies in order to maximize the results of people with various forms of paralysis.
Bottom Line
In conclusion, paralysis can take many forms, each varying in severity, cause, and impact on daily life. By understanding the different types of paralysis, individuals and caregivers can better recognize symptoms, seek early medical help, and explore effective treatment options. Although in some cases it is permanent, technology, rehabilitation, and progress in therapy have been made to enhance mobility and quality of life giving hope and independence to the living case of paralysis.
FAQs
What is the difference between flaccid and placid?
A flaccid cell is one placed in an isotonic solution, where no net inflow or efflux of water into or out of the cell takes place. A plasmolysed cell on the other hand is a situation where a plant cell is exposed to a hypertonic solution and the cell membrane drags away the cell wall as the water is lost.
What is a placid person like?
Developed out of the Latin placidus meaning pleasing or gentle, placid is most often applied to someone not readily irritated or of water like a lake that lacks waves to cause ripples. In both senses, placid is a synonym of calm, serene and tranquil.
Can a person recover from paralysis?
A full recovery can be possible within a short period in case of mild strokes whereas the patient can be left paralyzed or die in case of the severe strokes. Location of the Stroke: This is of great significance in the process of recovery.
What is paralysis in medical terms?
(puh-RA-lih-sis) Loss of ability to move all or part of the body.
Can high BP cause paralysis?
A stroke affects your thinking, movement, and functioning since the brain takes control of these. Stroke may result in brain damage, paralysis or even death unless immediate treatment is administered. According to neurologists, the greatest risk of stroke is high blood pressure.