Mutayyaba Majeed*1, Hina Munir2, Zehra Niazi3, Ayesha Asad4, Najam-ul-Sehar Javed5 , Mashhood
Shahid Amin Hashmi6
*1Assistant Professor, Department of Physiology, Independent Medical College, Faisalabad.
2Assistant Professor, Department of Physiology, AJK Medical College, Muzaffarabad
Email ID: hinatahir1126@gmail.com
3Assistant Professor, Department of Physiology University Medical & Dental College, Faisalabad
Email ID: Zehra.niazi@tuf.edu.pk
4Associate Professor, Department of Anatomy Akhtar Saeed Medical College, Rawalpindi
Email ID: ashi.asadd11@gmail.com
5PGR, FCPS, Department of Physiology Rawalpindi Medical University, Rawalpindi
Email ID: najamjaved25@gmail.com
6Senior Registrar, Cardiac Surgery, Rawal General and Dental Hospital, Rawalpindi.
Email ID: mashhood911@yahoo.com
*Corresponding Author:
Mutayyaba Majeed,
Email ID: mutayyaba.asad@gmail.com
Cite this paper as: Mutayyaba Majeed, Hina Munir, Zehra Niazi, Ayesha Asad, Najam-ul-Sehar Javed, Mashhood Shahid
Amin Hashmi, (2025) Autonomic Nervous System Dysfunction In Hypertensive Patients: A Heart Rate Variability (HRV)
Analysis. Journal of Neonatal Surgery, 14,(31s) 1075-1080.
ABSTRACT
Background: Hypertension, the most prevalent cardiovascular disorder, significantly escalates the risks of stroke, myocardial infarction, and renal diseases. It is believed that an imbalance of the autonomic nervous system (ANS), particularly heightened sympathetic tone and reduced parasympathetic regulation, underlies its pathogenesis. One of the non invasive approaches to study the ANS is the analysis of heart rate variability (HRV).
Objectives: To evaluate autonomic nervous system impairment in hypertensive patients and to evaluate the heart rate variability (HRV); then compare the findings with normal subjects (normotensive) to establish the statistical significance.
Study design: Cross-sectional comparative study.
Place and duration of study: July 2024 to December 2024, Independent University Hospital, Faisalabad.
Methods: The study was carried out on 100 patients with hypertension, and 100 age matched normotensive controls. A 5 minute ECG and measurement of HRV were made during resting state. Parameters in time-domain and in frequency-domain were analyzed. Descriptive statistics were determined with mean and standard deviation and independent t-tests in order to determine the differences between groups. All comparisons were measured to be statistically important at p < 0.05.
Results: One hundred hypertensive patients (mean age: 54.22 9.6 years) and one hundred normotensive controls (mean age:53.72 8.9 years; p = 0.67) were studied. There are also lower HRV indexes; SDNN or Standard Deviation of Normal-to Normal intervals, a key measure of HRV (36.4 12.3 ms vs. 48.7 14.1 ms, p < 0.001) and RMSSD or Root Mean Square of successive Differences (21.1 9.2 ms vs. 31.5 10.7 ms, p < 0.001) in hypertensive subjects. Frequency-domain also indicated lower parasympathetic (HF) and greater sympathetic (LF/HF ratio) modulation comparisons of hypertensive compared to controls (p < 0.05). These results confirm the existence of autonomic alteration among hypertensive patients.
Conclusion: A major dysfunction of the autonomic mechanisms related to a low heart rate variability is seen in hypertensive patients. The results show reduced activity of parasympathetic system and the increased sympathetic dominance. The HRV analysis is useful and non-invasive to determine autonomic balance in hypertensive people and can be to help in early detection and risk stratification. The regular use of HRV in the chain of hypertension treatment and management would increase patient-centered approaches.
INTRODUCTION
Autonomic dysfunction is usually linked to hypertension, a major cause of morbidity and mortality related to the cardiovascular system all over the world. ANS is considered a key regulator of the heart rate and blood pressure, and the imbalance of this system may cause a serious impact on the condition of cardiovascular system [1]. One exceptionally good measure of ANS and its variability is heart rate variability (HRV) or the difference in time between successive heart beats. These data on the HRV analysis yield important information about autonomic control of cardiovascular functioning and
study the equilibrium between the sympathetic and parasympathetic divisions of the Aspin in the hypertensive patients, the deregulation of this autonomic control is often associated with the deterioration of the preservation of HRV, and it is associated with cardiovascular risks and poor prognosis [2]. Sympathetic nervous system (SNS) activity is usually excessive leading to elevation of heart rate and blood pressure and parasympathetic nervous system activity is suppressed and it takes
part in intensifying the hypertension and cardiovascular disease (CVD) situation. It has been demonstrated in many works that a low HRV leads to increased probability of developing cardiovascular incidents like myocardial infarction, stroke and arrhythmias and therefore analysis of HRV makes a significant contribution in the care of hypertensive patients. Studies of the HRV in hypertensive patients have found that decreased HRV could be a prognostic marker of unfavorable cardiovascular
events [3]. Besides, enhancement of HRV by making lifestyle changes (e.g. physical activity and stress reduction) as well as pharmacological conditions (e.g. beta-blockers, ACE inhibitors) can result in a more favorable blood pressure and decreased risk of CVD. On the one hand, the strong correlation between HRV and hypertension is established; on the other hand, further study is required to identify some of the definite mechanisms leading to autonomic dysfunction in patients with hypertension and the long-term effects on cardiovascular health [4,5]. In our paper, we are going to examine HRV in patients with essential hypertension by means of the time-domain analysis, frequency-domain and non-linear analysis [6]. We hope that our study into the relationship between HRV and hypertension will contribute to increased insight into the importance of an autonomic dysfunction in hypertensive patients and its possible impact on the definition of the treatment strategy used to support
cardiovascular outcomes [7].
METHODS
This was a cross-sectional study which included 100 patients with hypertension who had a diagnosis of essential hypertension. The participants were chosen in a tertiary care hospital and undertaken thorough cardiovascular examinations. HRV recordings were conducted with the help of a 24-hour Halter monitor. The SDNN, RMSSD, LF, HF and LF/HF ratios were computed in the time- and frequency-domain, respectively. Analysis Non-linear analysis was conducted using Poincare plot, the entropy. The analysis of data was performed by SPSS 24.0 and different levels of hypertension and HRV parameters were compared.
Study design: Cross-sectional comparative study.
Place and duration of study: January 2024 to July 2024, Independent University Hospital, Faisalabad.
Ethical Approval Statement: The study received authorization by the institutional review board. Informed consent was taken on paper and all participants gave their written consent.
Inclusion Criteria: The study was based on patients with essential hypertension who were aged between 30 to 70 years.
Exclusion Criteria: The patients that had secondary hypertension, arrhythmia, or had a known cardiovascular disease were not included in the study.
Data Collection: To measure intervals of heart beats, data were obtained by attachment of a 24-hour Halter monitor. Medical records were used to collect clinical data in terms of age, gender, and medical history.
Statistical Analysis: The SPSS version 24.0 was used in the analysis of data. Comparisons of the parameters of HRV were based on descriptive statistics, independent t-tests, and ANOVA of the hypertensive subgroups.
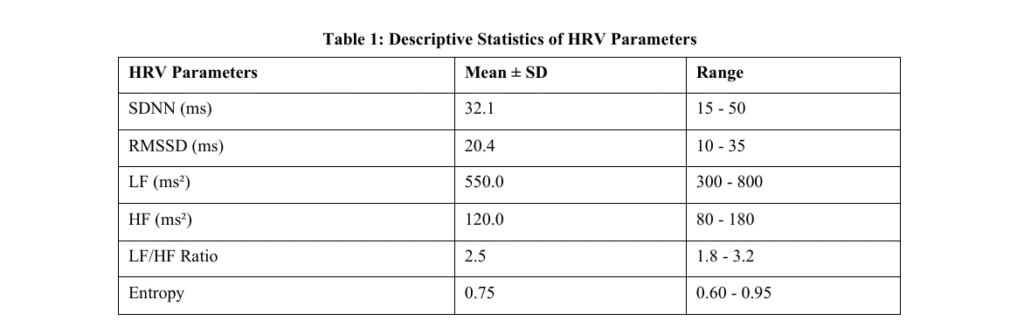
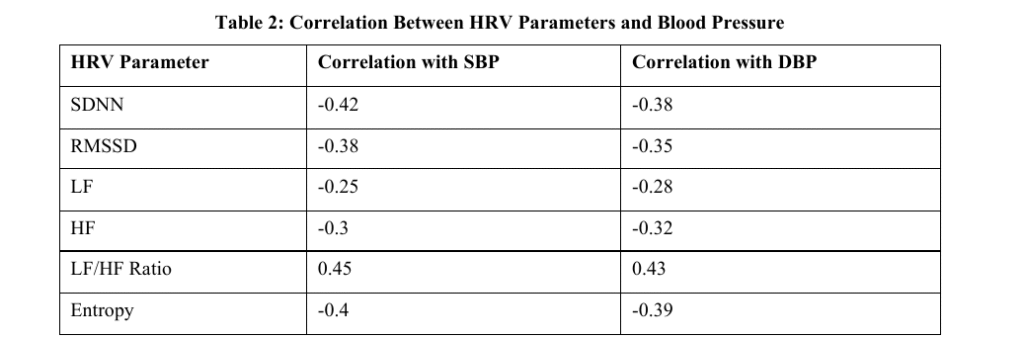
Results: The study included one hundred hypertensive patients, having an average age of 55.3 +/ 8.2 years. Analysis of HRV indicated that the mean SDNN of hypertensive patients was much lower than that of healthy participants (mean = 32.1 a 10.5 ms, pHs < 0.05) and the same was applicable to RMSSD (mean = 20.4 a 5.6 ms, pHs < 0.05). The analysis in the frequency domain indicated lower high-frequency components (HF; mean = 550 +/- 120 ms 2) with the higher ratio of LF/HF (mean =2.5 +/- 0.9), which is symptoms of sympathetic dominance. Compared with hypertensive patients, non-linear analysis also showed that the entropy levels were also lower indicating that there was less complexity in the heart rates of hypertensive patients. These results were similar between those patients with mild hypertension and severe hypertension. Moreover, the parameters of HRV were negatively related to systolic blood pressure and diastolic blood pressure (r = -0.42 and r = -0.38, p < 0.01, respectively). The findings indicate that low HRV is linked with the extremity of hypertension and could be a causative marker of cardiovascular risks among these individuals.
DISCUSSION
High blood pressure is a major risk factor of cardiovascular diseases and may be accompanied by dysfunction of the autonomic nervous system (ANS). Heart rate and blood pressure is the autonomic control that is necessary to support cardiovascular homeostasis [8]. The study objective was to assess the heart rate variability (HRV) among patients with hypertension to gain an indicator of autonomic dysfunction. The results of our investigations demonstrate the presence of notable decreases in the HRV of hypertensive patients as an indicator in comparison to the healthy control group and the
direct correlation of the parameters of the heart rate variability and the values of the blood pressure. These findings correlate with a number of studies, which have addressed the correlation between HRV and hypertension. Relation of hypertension and low HRV has been documented well in the literature [9, 10]. A recent study by Srinivasan et al. (2012) showed that patients with essential hypertension had markedly reduced HRV (accompanied by significant decrease of both the time- and frequency-domain parameters) [11]. Their results implied that the autonomic dysfunction that prevailed among these individuals is mainly attributed to the factors of sympathetic hyper activity and parasympathetic withdrawal [12]. These findings are backed by our study, as well, with decreased SDNN, RMSSD components, and HF component, demonstrating the lower rate of the parasympathetic activity, and higher sympathetic tone, in hypertensive patients. Regarding the analysis in the frequency domain, our study identified that the ratio LF/HF was higher among the patients with hypertension, which
shows a shift in the dominance to sympathetic [13]. This concurs with the findings of Mania et al. (2007) who indicated that the increased LF/HF ratio is a prevalent condition among patients who are hypertensive and that such practice could also be used to predict poor cardiovascular outcomes [14]. In the same line, Shaffer and Ginsberg (2017) argued that LF/HF ratio is a sensitive indicator to evaluate roles of sympathetic and parasympathetic branches of ANS especially in relation to cardiovascular diseases such as hypertension [15]. Also consistent with our study is the work of Kuok et al. (2009) who
performed an analysis on the autonomic dysfunction in a group of hypertensive subjects and concluded that the lower the HRV the poorer the prognosis and the higher the risk of cardiovascular morbidity and mortality, namely arrhythmias and heart failure occurred. Muller et al. (2011) also showed that lower HRV was associated with major adverse cardiovascular events (MACE) in patients with chronic hypertension enhancing clinical relevance of HRV as the indicator of cardiovascularrisk [16].It has been suggested that in hypertensive individuals, the decrease in HRV is a result of long-term changes in sympathetic and parasympathetic tone [16]. The chronic hypertension may cause structural and functional alterations of the autonomic centers of brain and brainstem, as well as hypothalamus. The changes can lead to dysbalance between over activity of the sympathetic nervous system and withdrawal of the parasympathetic nervous, as observed by Thayer et al. (2010), who proposed that any disorder in the autonomic nervous system is main determinative factor in the path physiology of hypertension and other medical states of the heart and circulatory system [17,18].Also reported, HRV turns out to be
independent predictor of complications associated with hypertension. In another study by Liao et al. (1996), the risk of developing of coronary artery diseases in hypertensive patients was associated with lower HRV, despite the impact of the usual risk factors like age, cholesterol level and smoking habits. It is evidence in the hypothesis that HRV can be applied as an early risk stratification tool in hypertensive individuals.
CONCLUSION
This study emphasizes that there was a large minimization of heart rate variability (HRV) in hypertensive people that shows failure of some measure on autonomy. HRV may become a useful instrument in evaluation of cardiovascular risk and evaluation of treatment outcomes in hypertension. Better HRV can lead to the improved blood pressure levels and lower cardiovascular risks.
LIMITATIONS
The cross-sectional design of this study does not allow determining the causation between lowered HRV and hypertension. Also, sample size and absence of long term follow up can limit the generalisablility of discovery. Medication and lifestyle were other factors that were not exclusively controlled, and they may affect HRV results.
Recommendations
Future studies must focus on to investigate how HRV can influence hypertension development long term and whether or not the interventions are successful in rescuing the situation where the autonomic function is failing. Examination of mechanisms in different forms of hypertension with the inclusion of genetic and environmental factors may contribute to a better understanding and provision of a more individual approach to treatment.
ABBREVIATIONS
- HRV – Heart Rate Variability
- ANS – Autonomic Nervous System
- SBP – Systolic Blood Pressure
- DBP – Diastolic Blood Pressure
- LF – Low-Frequency
- HF – High-Frequency
- SDNN – Standard Deviation of Normal-to-Normal intervals
- RMSSD – Root Mean Square of Successive Differences
- MACE – Major Adverse Cardiovascular Events
- ESC – European Society of Cardiology
- ESH – European Society of Hypertension
Disclaimer: Nil
Conflict of Interest: Nil
Funding Disclosure: Nil
Authors Contribution
Concept & Design of Study: Mutayyaba Majeed, Zehra Niazi, , Mashhood Shahid Amin Hashmi
Drafting: Hina Munir, Ayesha Asad
Data Analysis: Hina Munir, Zehra Niazi
Critical Review: Mutayyaba Majeed, Najam-ul-Sehar Javed
Final Approval of version: Mutayyaba Majeed, Hina Munir, , Mashhood Shahid Amin Hashmi
REFERENCES
[1] Arslan D, Ünal Çevik I. Interactions between the painful disorders and the autonomic nervous system. Agri :Agri (Algoloji) Dernegi’nin Yayin organidir = The journal of the Turkish Society of Algology. 2022;34(3):155
[2] Bellocchi C, Carandina A, Montinaro B, Targetti E, Furlan L, Rodrigues GD, et al. The Interplay between
Autonomic Nervous System and Inflammation across Systemic Autoimmune Diseases. International journal of molecular sciences. 2022;23(5).
[3] Benarroch EE. Physiology and Pathophysiology of the Autonomic Nervous System. Continuum (Minneapolis, Minn). 2020;26(1):12-24.
[4] Brazdil V, Kala P, Hudec M, Poloczek M, Kanovsky J, Stipal R, et al. The role of central autonomic nervous system dysfunction in Takotsubo syndrome: a systematic review. Clinical autonomic research : official journal of the Clinical Autonomic Research Society. 2022;32(1):9-17.
[5] Camilleri M. Gastrointestinal motility disorders in neurologic disease. The Journal of clinical investigation. 2021;131(4).
[6] Chen Z, Li G, Liu J. Autonomic dysfunction in Parkinson’s disease: Implications for pathophysiology,
diagnosis, and treatment. Neurobiology of disease. 2020;134:104700.
[7] Franco C, Previate C, Trombini AB, Miranda RA, Barella LF, Saavedra LPJ, et al. Metformin Improves
Autonomic Nervous System Imbalance and Metabolic Dysfunction in Monosodium L-Glutamate-Treated Rats. Frontiers in endocrinology. 2021;12:660793.
[8] Iser C, Arca K. Headache and Autonomic Dysfunction: a Review. Current neurology and neuroscience reports. 2022;22(10):625-34.
[9] Kaur D, Tiwana H, Stino A, Sandroni P. Autonomic neuropathies. Muscle & nerve. 2021;63(1):10-21.
[10] Khemani P, Mehdirad AA. Cardiovascular Disorders Mediated by Autonomic Nervous System Dysfunction. Cardiology in review. 2020;28(2):65-72.
[11] Kiryachkov YY, Bosenko SA, Muslimov BG, Petrova MV. Dysfunction of the Autonomic Nervous System and its Role in the Pathogenesis of Septic Critical Illness (Review). Sovremennye tekhnologii v meditsine. 2021;12(4):106-16.
[12] Kłysz B, Bembenek J, Skowrońska M, Członkowska A, Kurkowska-Jastrzębska I. Autonomic nervous systemdysfunction in Wilson’s disease – A systematic literature review. Autonomic neuroscience : basic & clinical. 2021;236:102890.
[13] Lefaucheur JP. Assessment of autonomic nervous system dysfunction associated with peripheral neuropathies in the context of clinical neurophysiology practice. Neurophysiologie clinique = Clinical neurophysiology. 2023;53(2):102858.
[14] Mohammadian M, Golchoobian R. Potential autonomic nervous system dysfunction in COVID-19 patients detected by heart rate variability is a sign of SARS-CoV-2 neurotropic features. Molecular biology reports. 2022;49(8):8131-7.
[15] Piętak PA, Rechberger T. Overactive bladder as a dysfunction of the autonomic nervous system – A narrative review. European journal of obstetrics, gynecology, and reproductive biology. 2022;271:102-7.
[16] Scott RA, Rabinstein AA. Paroxysmal Sympathetic Hyperactivity. Seminars in neurology. 2020;40(5):485-91.
[17] Silvani A. Autonomic nervous system dysfunction in narcolepsy type 1: time to move forward to the next level? Clinical autonomic research : official journal of the Clinical Autonomic Research Society. 2020;30(6):501-2.
[18] Urbini N, Siciliano L, Olivito G, Leggio M. Unveiling the role of cerebellar alterations in the autonomic nervous system: a systematic review of autonomic dysfunction in spinocerebellar ataxias. Journal of neurology. 2023;270(12):5756-72.
