Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
The monitoring of blood glucose (SMBG) is a crucial aspect of successful diabetes management. It enables patients to monitor their own blood sugar levels, enabling them to learn how their diet, physical activity, stress, and medications affect their blood sugar levels. Patients can make informed choices and notice changes before they occur as they check and record their readings on a regular basis. Finally, SMBG will enable individuals with diabetes to actively manage their health and avoid long-term complications.
Understanding Self-Monitoring of Blood Glucose (SMBG)
Self-Monitoring of Blood Glucose (SMBG) is a type of monitoring that allows those with diabetes to check their sugar levels at home with a glucometer that assists them in managing their condition by making decisions related to diet, physical activity, and drugs. Consistent monitoring will give blood sugar profile, enable treating high or low blood sugar immediately, improve glycemic control, and enhance communication with health care providers.
How SMBG works
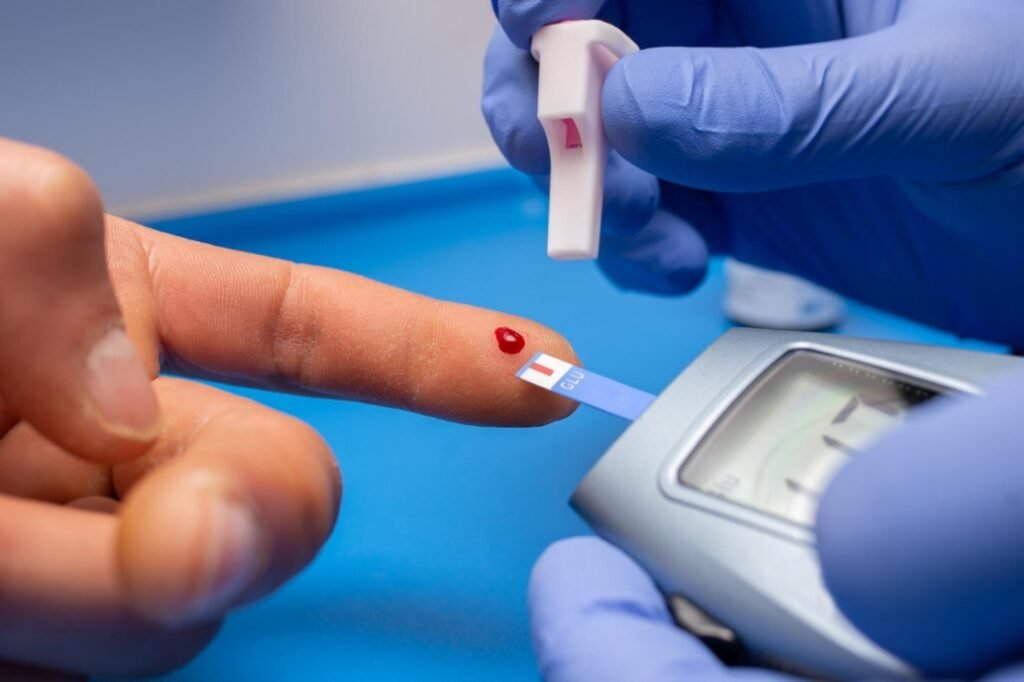
- A prick of blood is taken (usually a finger) (or occasionally otherwise).
- A blood sample is put in a test strip, and a meter will give a reading of blood glucose in a few seconds.
- Most meters archive results and can provide trend over time.
Why SMBG is important
- Improves glycemic control: With blood glucose monitoring, one can make wise decisions regarding his or her diet, exercise and pharmacology, which results in improved glycemic control.
- Assist in recognizing trends: SMBG helps individuals with diabetes and their medical caregivers to know how various factors influence the process of blood glucose levels.
- Avoids complications: Long-term diabetes complications may be avoided through regular monitoring, which makes the blood sugar level within the target range.
- Issues with hypoglycemia and hyperglycemia: It is vital in diagnosing and managing the dangerous low and high sugar levels promptly.
- Facilitates individualized treatment regimens: The data collected can be used to adjust doses of insulin, diet and exercise to produce an individualized treatment regimen.
The Role of Healthcare Providers in SMBG
Self-monitoring of blood glucose (SMBG) depends on healthcare providers, who, through educating patients, ensure they set personalized goals and use data to inform and modify treatment plans. Their role involves initial training, ongoing support, and assisting patients to interpret and make use of SMBG results to regulate diet, exercise, and medication which leads to improved glycemic control and empowerment.
Key roles of healthcare providers in SMBG
- Patient education:
- Give the first training on how to carry out SMBG properly, the use of meter and ketone test when necessary.
- Train patients to understand how to interpret their readings and how food exercise among other factors influences their blood glucose.
- Goal setting and personalization:
- The partnership with patients to develop personalized SMBG guidelines (frequency and intensity) according to their needs and treatment objectives.
- Concur with the reason of SMBG with the patient and record such objectives.
- Therapeutic adjustments:
- Utilize the SMBG data to make informed and timely decisions on whether to make changes in the areas of medication, lifestyle, and diet.
- Help patients to cope with acute conditions such as sickness by monitoring SMBG more often.
- Ongoing support and monitoring:
- Offer post-training follow-up (follow-up calls, emails, visits).
- Proactively examine SMBG with the patient and give feedback and motivation, particularly when outcomes are disheartening.
- Empowerment and partnership:
- Empower patient-provider relationship: promote patient autonomy and make them feel they have control over their diabetes.
- Role- Have patients make the right day-to-day treatment decisions using SMBG.
You may also like to read: Impact of Diabetes on Relationships and Daily Life
Technological Advances in Glucose Monitoring
Technological advances in glucose monitoring include the development of Continuous Glucose Monitors (CGM) and Flash Glucose Monitors (FGM), which are more convenient and less invasive than traditional finger pricks. Other key advancements are the integration of CGMs with automated insulin delivery (AID) systems, the development of more accurate and smaller sensors, and the exploration of non-invasive and self-powered technologies. These innovations improve glycemic control, reduce hypoglycemia, and provide users with real-time data and alerts.
Final Thoughts
In conclusion, self-monitoring of blood glucose plays a crucial role in achieving better diabetes control and overall well-being. By consistently tracking blood sugar levels, individuals can recognize patterns, make timely adjustments, and work more effectively with their healthcare providers. Regular monitoring not only helps prevent complications but also fosters greater confidence and independence in managing diabetes.
FAQs
What is self-monitoring of blood glucose levels?
Self-monitoring of blood glucose (SMBG) can be a useful tool in the management of diabetes mellitus. Patients with diabetes often measure their blood glucose to detect hypoglycemia and to adjust insulin dose as needed.
What is the 15 minute rule for diabetes?
If your blood sugar is low, follow the 15-15 rule: Have 15 grams of carbs, then wait 15 minutes. Check your blood sugar again. If it’s still less than 70 mg/dL, repeat this process.
What is the 3-hour rule for diabetics? The “three-hour rule” for rapid-acting insulin (aka “Insulin Stacking”) Rapid-acting insulin begins to work about 15 minutes after injection, peaks in about 1 hour, and continues to work for 2 to 4 hours. The three-hour rule prevents “insulin stacking” and a low blood glucose (BG) or hypoglycemia.