Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
The body microbiome is a complex ecosystem of trillions of microorganisms that organize our intestines and perform essential functions that keep the rest of the body healthy. Other than contributing to digestion, these microbes play a critical role in regulating metabolism, which encompasses blood sugar levels, fat storage, cholesterol count, and management of inflammation. With the rising cases of metabolic diseases like obesity, type 2 diabetes and heart diseases, it becomes imperative to understand the relationship between the gut and metabolism. It has been revealed that a healthy microbiome in the gut can have a significant influence on maintaining weight, the sensitivity of insulin and activities of the immune system, therefore, it is the major factor that can propel metabolic wellness in the long-term.
What Is the Gut Microbiome?
Gut microbiome is the complex community comprising bacteria, yeast and fungi etc inhabiting mainly in the big intestine that is part of the human gastrointestinal tract, specifically the large intestine. This community of diverse microbes is always considered as ‘hidden organ’ since it works differently to interact with various internal systems of the body and performs vital tasks in reference to health and disease. The combined genetic makeup of all these microbes is the gut microbiome (metagenome), which contains many genes as the human genome itself, overall.
Key Microbial Phyla
Most bacteria in the intestines are of a few major phyla:
- Firmicutes: It is one of the prevalent phyla, and it contains such significant genera as Clostridium, Lactobacillus, Faecalibacterium, and Ruminococcus. Firmicutes have members that ferment dietary fiber and thus produce short-chain fatty acids (SCFAs)
- Bacteroidetes: The other major phylum, encompassing both Bacteroides and Prevotella genera, has a particular aptitude to degrade complex carbohydrates and proteins.
- Actinobacteria: Though they are present in lower quantities, they contain good bacteria such as Bifidobacterium which is essential in keeping the gut healthy.
- Proteobacteria and Fusobacteria: The phyla find their way at lower levels and still are pronounced members of the gut microbiome.
- Verrucomicrobia: The other less prevalent yet pertinent set is Akkermansia muciniphila whose ability to degrade mucins is discussed as well as its role in performing gut barrier functions.
Collectively, Firmicutes and Bacteroidetes comprise an approximate average of 90 percent of the restriction of bacteria in the gut, although again, the specific makeup is highly variable in different people depending on diet, age, wellness, and much to the different germs in close vicinity.
Role in Digestion and Nutrient Extraction
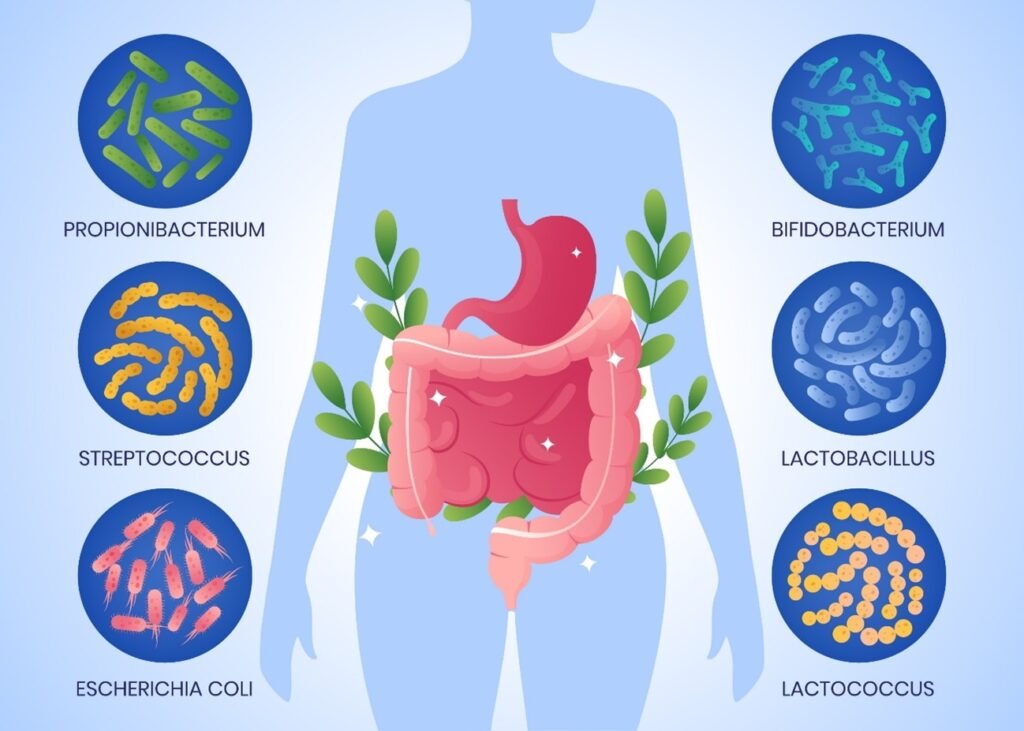
The microbiome of the gut is important in digestion and the extraction of nutrients that man alone could not do:
- Breakdown of Dietary Fiber and Polysaccharides: Human enzymes are unable to digest many of the plant fibers and complex carbohydrates. These substances are fermented by gut bacteria, producing SCFAs, like acetate, propionate and butyrate, which are consumed as the energy source by the gut lining, and have positive metabolic and anti-inflammatory outcomes.
- Metabolizing Bile Acids and Sterols: Microbes break down Bile Acids and break down all sterols to help the body digest fat and absorb fat cells and to recycle these cells for effective usage.
- Synthesis of Vitamins and Amino Acids: Some bacteria in the gut microbiome can produce important micronutrients, such as different B vitamins (B1, B9, B12) and vitamin K, which are vomited on the host and serve to benefit your health in general
- Energy Harvest: Microbial digestion of undigested carbohydrates enhances the capacity of the host to obtain energy and store it in the diet. Research studies have demonstrated that food preferences in humans were also associated with variance in the composition of gut microbes and could result in obesity.
- Immune System and Barrier Function: The gut microbiota contributes towards the structural integrity of the gut lining, imparts education to the immune system and resistance to colonization of disease-causing pathogens by outcompeting or secreting antimicrobial substances.
How the Gut Microbiome Affects Metabolic Health
1. Production of Short‑Chain Fatty Acids (SCFAs)
The bacteria in the gut eat up dietary fibers and process them to produce some of the key metabolites, which are acetate, propionate, and butyrate, which are signals of this metabolism. Increased levels of systemic SCFA have been correlated with insulin sensitivity improvement and reduce fasting insulin and HOMA- IR indices in human meta-analyses. These SCFAs agonize Ffar2 and Ffar3 on enteroendocrine cells and enhance release of GLP-1 and PYY, which increase insulin level, feelings of fullness, and prolong gastric emptying. They also inhibit lipolysis, regulate fat storage, and decrease low ‑grade inflammation, all of which is important to the balance of metabolism
2. Regulation of Inflammation
Intact gut barrier contributes to a healthy microbiome by facilitating tight junctions, maintenance of mucus layer and the maintenance of immune homeostasis. Dysbiosis interferes with this and parts of bacteria, such as lipopolysaccharides (LPS), end up escaping into the circulation in something called a state of metabolic endotoxemia. These endotoxins stimulate the TLR and NF-kB pathways leading to the development of chronic low-grade inflammation leading to insulin resistance and fat increase.
3. Influence on Insulin Resistance and Blood Sugar
Another effect of the intestinal beneficial microbiome role in glucose homeostasis is the intestinal gluconeogenesis (IGN). Butyrate exerts its effect via cAMP-dependent signaling systems, but propionate has the effect of stimulating a neural circuit between the gut and the brain, which increases glucose homeostasis in animal models. Higher fasting circulating SCFA concentrations in humans correlates with high GLP-1 and enhanced insulin sensitivity in clamp-based measurement in such a way that circulating rather than fecal SCFA serves better markers of metabolic health
4. Gut–Liver Axis and Bile Acid Modulation
Primary bile acids are converted to secondary bile acids by using microbial enzymes (such as bile salt hydrolases and 7alpha-dehydroxylases) which include deoxycholic acid (DCA) or lithocholic acid which can activate FXR and TGR5 receptors. Ileal FXR activation and TGR5 stimulation stimulate the production of FGF19 and thermogenesis respectively and reduce hepatic lipid processing and de novo lipogenesis in brown fat and GLP-1-mediated insulin secretion, respectively.
The microbiome of the gut is an epicenter in metabolic control via the coordination of nutrient-derived metabolite, barrier protection, and hormone production as well as downstream bile acid signaling. The adjustments of those pathways caused by fiber-poor diets, antibiotics exposure, or imbalance of major taxa may shift the system towards insulin resistance, fat over storage and inflammation.
Signs of an Unhealthy Gut and Its Link to Metabolic Disorders
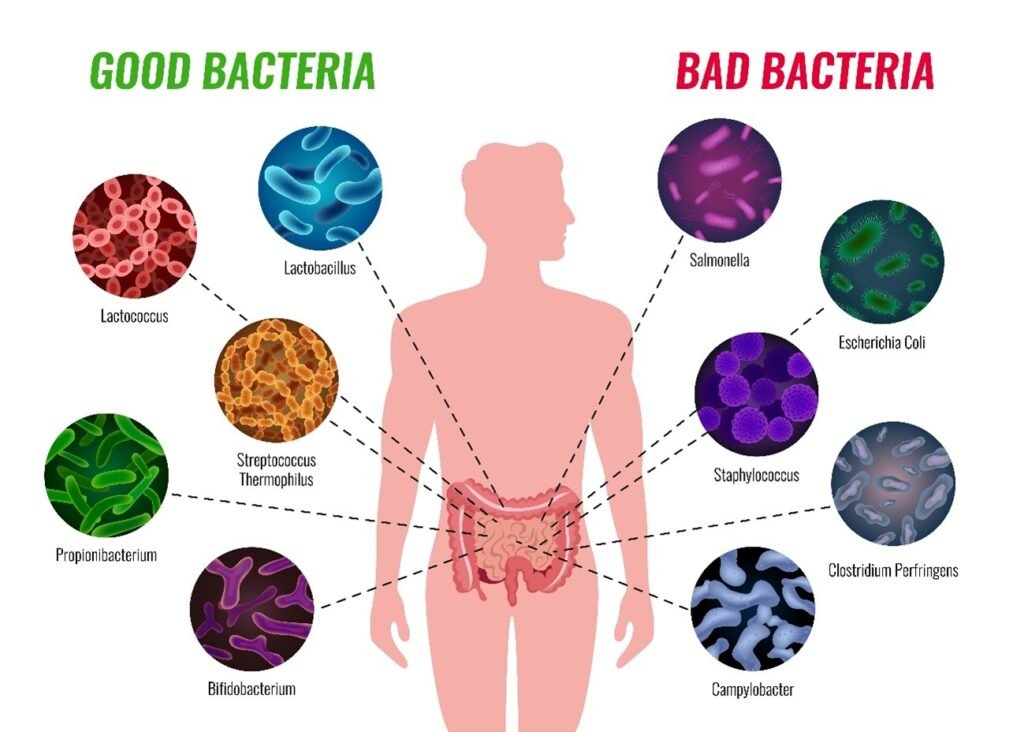
Symptoms of Dysbiosis
Gut dysbiosis is an imbalance of the composition of the gut microbiome, which is sometimes characterized by a reduction in beneficial microorganisms, an overgrowth of harmful ones or a loss in diversity. The typical symptoms are:
- Digestive Problems Include Bloating; excess gas, diarrhea, constipation, heart burn and pains in the abdomen are also strong indications of a dysbalanced intestinal flora.
- Fatigue: Chronic fatigue or tiredness is a frequent complaint of people with gut problems, and a study has linked energy levels with the microbial balance in the digestive tract.
- Sugar Cravings: There may be imbalances that can influence the desire to eat sugar and processed foods which could be due to bacteria affecting food preferences.
- Accidental Changes in Weight: Weight changes can occur undesirably due to spontaneous weight gain or loss because of the other factors of how the body absorbs and stocks fat.
- Skin Problems: Acne, eczema, rashes, psoriasis, and skin issues of other sorts may be the products of gut inflammation and its effect on the immune system.
- Mental and Cognitive: Anxiety, depression, brain fog, and difficulty concentration have all been clinically shown to relate to poor gut health because of the connection between the brain and the gut.
Other: Bad breath, joint pain, food intolerances and they become more vulnerable to inflammatory conditions or infections.
You may also like to read: Role of Insulin Resistance in Metabolic Health
Conditions Associated with Poor Gut Health
Dysbiosis is closely linked to several metabolic disorders:
Obesity: Due to alterations in gut microbiota, alterations can affect energy harvesting, fat storage, and hunger/satiety signals and therefore act as a factor in the development and maintenance of obesity.
Type 2 Diabetes: Unhealthy Gut microbiome may lead to insulin resistance, alterations to the pathways involved in carbohydrate metabolism, and, lastly, propagating unrelenting inflammation, each of which is in central to type 2 diabetes.
Metabolic Syndrome: Such a combination of conditions (insulin resistance, high blood pressure, abnormal blood fats, and large waist circumference) makes up this syndrome that well correlates with gut dysbiosis leading to low-grade inflammation and affecting metabolism in various ways.
Mechanism Underlying the Link
- Increased Gut Permeability (“Leaky Gut”): Dysbiosis can also damage the lining of the gut, allowing pro-inflammatory molecules and toxins to enter the bloodstream and set up systemic inflammatory reactions and failure to regulate metabolism.
- Low-grade chronic inflammation Insulin resistance, obesity and metabolic syndrome caused by low grade chronic inflammation of gut imbalance.
- Perturbed hormonal and immune signaling: Microbial metabolites influence such hormones as insulin, leptin, and GLP-1 as well as the activity of immune cells that are important to metabolic health.
Taking care of a healthy gut-through diet and lifestyle and sometimes probiotics or prebiotics is becoming one of the approaches to prevention or management of metabolic disorders and its complications.
How to Support a Healthy Gut for Metabolic Wellness
Here is how to support a healthy gut for metabolic wellness:
Eat More Fiber and Prebiotics
Why: The reason is dietary fiber serves as food to good bacteria in the gut and helps them to grow and diversify which is central to metabolic and gut health.
Examples of Fiber- and Prebiotic-Rich Foods:
- Whole grains: oats, quinoa, barley
- Legumes: chickpeas, lentils, beans
- Fruits: bananas, apples, peaches (also rich in polyphenols)
- Vegetables: garlic, onions, leeks, asparagus, broccoli
- Nuts: almonds, pistachios, cashews
Prebiotics represent a particular type of fiber which is like fertilizers to our good bacteria, and can be found in onions, garlic, leeks, and chicory as well as bananas.
Include Fermented Foods and Probiotics
Fermented foods have developed beneficial microorganisms (probiotics), which have the capability of increasing microbial diversity and improving gut function.
- Examples:
- Yogurt with live cultures
- Kefir
- Sauerkraut
- Kimchi
- Kombucha
- Miso and tempeh
A consistent intake of foods can be beneficial in the establishment of healthier gut and general health.
Limit Processed Foods and Refined Sugars
- Sugar and processed foods impair microbial flora because they support the proliferation of detrimental bacteria.
- The ultra-processed foods are where they include a lot of unhealthy fats, additives, and sugars which decrease the gut biodiversity and inflammation.
Consider Supplementation
There are specific probiotic strains that show potential regarding metabolic and gut health which however needs to be individualized and taken with medical guidance.
- Remarkable strains are since,
- Akkermansia muciniphila – associated with metabolic and enhanced gut barrier.
- Anaerobutyricum soehngenii – butyrate-producing bacterium advantageous in terms of gut health.
- Supplementation is also a new field of study and must supplement a healthy eating lifestyle.
By maintaining a fiber-rich, diverse plant-based diet, probiotic fermented foods, and reduced intake of destructive processed foods, the gut microbiome can be maintained very well and requires metabolic wellness. Proper advice can be obtained from doctors which can help to customize probiotic supplementation where necessary.
Conclusion
The gut microbiome plays a crucial role in regulating key aspects of metabolic health, including blood sugar control, fat storage, inflammation, and energy balance. Disruptions in microbial diversity and function can contribute to serious conditions like obesity, type 2 diabetes, and metabolic syndrome. Fortunately, you can support a healthier gut—and a healthier metabolism—through simple yet powerful changes in your diet and lifestyle. Start today by incorporating more fiber-rich, gut-friendly foods like fruits, vegetables, legumes, and fermented products into your meals to nourish your microbiome and boost your overall well-being.