Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Diabetes is a status that repeatedly influences how the body handles and utilizes blood sugar, or glucose-the most critical energy provider to our cells. Be it Type 1 diabetes or Type 2, or gestational diabetes, it is important that the level of blood sugar remains within a healthy range to avoid the short-term complications of hypo and hyperglycemia, and long-term effects on the heart, kidneys, neurons, and eyes. The importance of blood sugar monitoring in diabetes cannot be overstated, as it provides valuable insights into how diet, physical activity, medication, and lifestyle choices impact glucose control. When individuals monitor such patterns over time, they will be able to make informed choices that will have positive health implications and a good quality of life.
Understanding Blood Sugar and Diabetes
The primary sugar in your blood, also known as blood glucose, is the energy source that the body uses. It is provided through what you eat, especially the carbs which is dissimulated into glucose that changes into the bloodstream. Insulin is one of the pancreatic hormones, which facilitate transport of glucose in the blood to the cells where it acts as energy source.
Diabetes is a condition in which the amount of glucose in the blood is abnormally high due to lack of production or use of insulin, or both. This results in glucose remaining in the blood, resulting in several health effects in the long-term.
Blood glucose targets for people with diabetes typically are:
- 80 to 130 mg/dL before meals
- Less than 180 mg/dL two hours after starting a meal
Regulating blood sugar level in target ranges is the key in management and prevention of diabetes complications including deteriorated eyes, kidney, nerve, and heart issues. Monitoring includes frequent blood glucose checks. In some cases, hemoglobin A1c in order to get a gauge of the average blood sugar level over several months.
Why Blood Sugar Monitoring is Essential
Monitoring of blood sugar is critical in managing diabetes due to several reasons:
- It guides you to learn which factors such as food, physical activity, medication, and stress influence your blood sugar levels during the day. This information would enable you to make informed change of lifestyle or treatment.
- Constant checking can ensure you monitor the patterns and fluctuations in your blood sugar and stay within your levels of your desired target range. Remaining in this range minimizes the chances of adverse, short-term issues (such as hypoglycemia and hyperglycemia) and long-term complications to the eye, kidney, nerve, and heart.
- Monitoring also helps healthcare providers to decide on a treatment plan to deal with your diabetes, including any change in medication or insulin doses.
- It enables early warning of excessive and insufficient blood sugar levels, which can cause severe health problems in case of timely treatment.
- Regular self-blood sugar tests represent the day-to-day variability that can be missed in average blood sugar tests temporary, but this is essential in managing diabetes daily.
- People on insulin should monitor themselves prior to meals, following meals, before going to bed, and when symptoms of low or high sugar manifest themselves, particularly to achieve safe and effective control.
Methods of Blood Sugar Monitoring
There are several common methods for monitoring blood sugar, especially for people with diabetes:
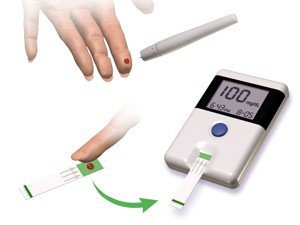
Self-Monitoring with a Blood Glucose Meter (Finger Stick Test)
· This is where the side of the fingertip is pricked using a lancet to release a little blood.
· A drop of blood is dropped on disposable test strip and fitted into a glucose meter which measures and displays the blood sugar concentration.
· It gives a measure of blood sugar at that time and is the most employed home-type of monitoring.
Continuous Glucose Monitoring (CGM)
· CGM -This approach measures the level of glucose in the fluid between cells every few minutes with a small sensor that is implanted under the skin.
· Data is transmitted wirelessly to real-time glucose monitoring receiver, smartphone or insulin pump.
· CGMs have the capacity to offer high and low blood sugar warnings, monitor trends and offer comprehensive data on diabetes management.
· Sensors usually require replacement out in 7-14 days, but certain implanted sensors can last several months.
Flash Glucose Monitoring (e.g., FreeStyle Libre)
· Like CGM but must scan a sensor on the skin into a reader or smart phone to obtain glucose results.
· It is not alarm-based and allows glucose trends and recent history upon scan.
A1C Blood Test (Laboratory Test)
- Determines the average blood glucose in the past 2-3 months is determined based on the glucose bound to hemoglobin in red blood cells.
- It is done on a regular basis by a medical practitioner to check the long-term control of glucose as opposed to daily variations.
How to Interpret Blood Sugar Readings
Blood sugar readings have ranges that represent normal blood sugar, prediabetes and diabetes. This is a simple guide on how to read blood sugar results:
Blood Sugar Levels (in mg/dL)
- Fasting (before meals):
- Normal: 70 to 99 mg/dL
- Prediabetes: 100 to 125 mg/dL
- Diabetes: 126 mg/dL or higher (on two separate tests)
- Two hours after eating:
- Normal: Less than 140 mg/dL
- Prediabetes: 140 to 199 mg/dL
- Diabetes: 200 mg/dL or higher
- Random blood sugar test (any time of day):
- Diabetes likely if 200 mg/dL or higher with symptoms of diabetes
- Low blood sugar (hypoglycemia):
- Below 70 mg/dL can be considered low and may cause symptoms needing prompt treatment
Why These Numbers Matter
- Maintaining blood sugar in the target range can prevent or delay such complications as nerve damage, vision difficulties, kidney disease, and heart problems.
- Very high readings can mean changing medications, food and/or exercise.
- Low readings need right away care to avoid severe symptoms.
Checking your levels regularly and collaborating with medical personnel to know your target levels and how your numbers compare with your health is a major factor in successful management of diabetes.
You may also like to read: Diabetes Management
Tips for Effective Blood Sugar Monitoring
Here are some key tips for effective blood sugar monitoring to help manage diabetes properly:
Prepare your tools: Ensure your meter has power, strips are valid, and your hands are clean and dry.
Use proper technique: Prick the side of your fingertip, apply blood as instructed, and avoid squeezing too hard.
Test at the right times: Follow your provider’s advice on when to test for accurate patterns.
Log your readings: Record results with date, time, and notes, or use apps for tracking.
Store supplies safely: Keep strips and lancets cool, dry, and out of direct sunlight.
Don’t share equipment: Use only your own meter and lancets; dispose of lancets properly.
Warm cold hands: Improve blood flow before testing for easier sampling.
Review trends: Check patterns over time and discuss them with your healthcare team.
Seek guidance: Get professional help when learning to monitor blood sugar.
Consider technology: Use CGMs or flash monitors if recommended for continuous data.
Bottom Line
Monitoring is one of the pillars of an effective management of diabetes, as it allows individuals to manage the rise or fall of their blood sugar level. With proper technique, record-keeping consistency, and professional healthcare support, people with diabetes can implement informed decisions with regards to their own longevity. In the end, checking the level of sugar in the blood not only excludes the risks of complications but also leads to more active and healthy life and a feeling of confidence.