Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Diabetes may impact most of the body parts, but feet are more susceptible. A diabetic foot ulcer is one of the most dangerous complications that may cause a critical infection and long-term health issues in case of improper treatment. Regular care and attention can prevent most of the diabetic foot ulcer. Simple daily practices can mitigate the risk factors, including examining your feet, using the right footwear, and maintaining healthy skin. This paper will discuss effective foot care tips that are essential in avoiding diabetic foot ulcers and securing your general health.
What Are Diabetic Foot Ulcers?
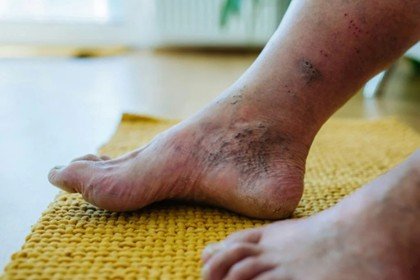
Diabetic foot ulcers are open wounds or sores which develop around the feet of diabetics. The cause of these wounds is the breakdown of skin tissue and the exposure of deeper tissue layers, usually a combination of nerve damage (neuropathy), poor circulation and high blood sugar levels, which inhibit healing. They usually show on the lower part of the foot like the big toes and the feet balls.
They are severe complications of diabetes and may result in infection, gangrene, or amputation unless they are treated. Approximately one-third of diabetics can experience a foot ulcer in their lifetime. The ulcers develop because of the loss of sensation caused by nerve damage, pressure or irritation caused by foot deformity, and low blood flow that slows healing. Therapy includes sugar regulation, wound management, pressure ulcers, and occasionally surgery or antibiotics in case of infection. Foot care and early diagnosis are essential in the prevention of such ulcers and severe outcomes.
Why Prevention Is Important
Diabetic foot ulcers prevention is of utmost importance since the ulcers are open sores, which is highly prone to infection. Foot ulcer infections may spread to the bone which endangers their health and can cause severe consequences, including the amputation of the foot. Because patients with diabetes tend to experience nerve damage (peripheral neuropathy), they are less likely to notice injuries or pain thus some minor injury can be neglected and develop into ulcers. As well, ulcers are more dangerous because of diabetes-induced poor circulation slowing healing.
Foot ulcer prevention will prevent complications such as infections, hospitalization, and amputation, which will save mobility and quality of life. Among the key prevention strategies are foot checks to identify early injury, blood sugar level control, managing risk factors such as smoking and cholesterol, wearing proper shoes, and regular podiatric care. Early diagnosis and adequate foot care will greatly lower the chances of the development of ulcers and expensive complications. Risk factor screening and patient education on foot also prevent ulcers and adjoining morbidity.
Daily Foot Care Tips for Prevention
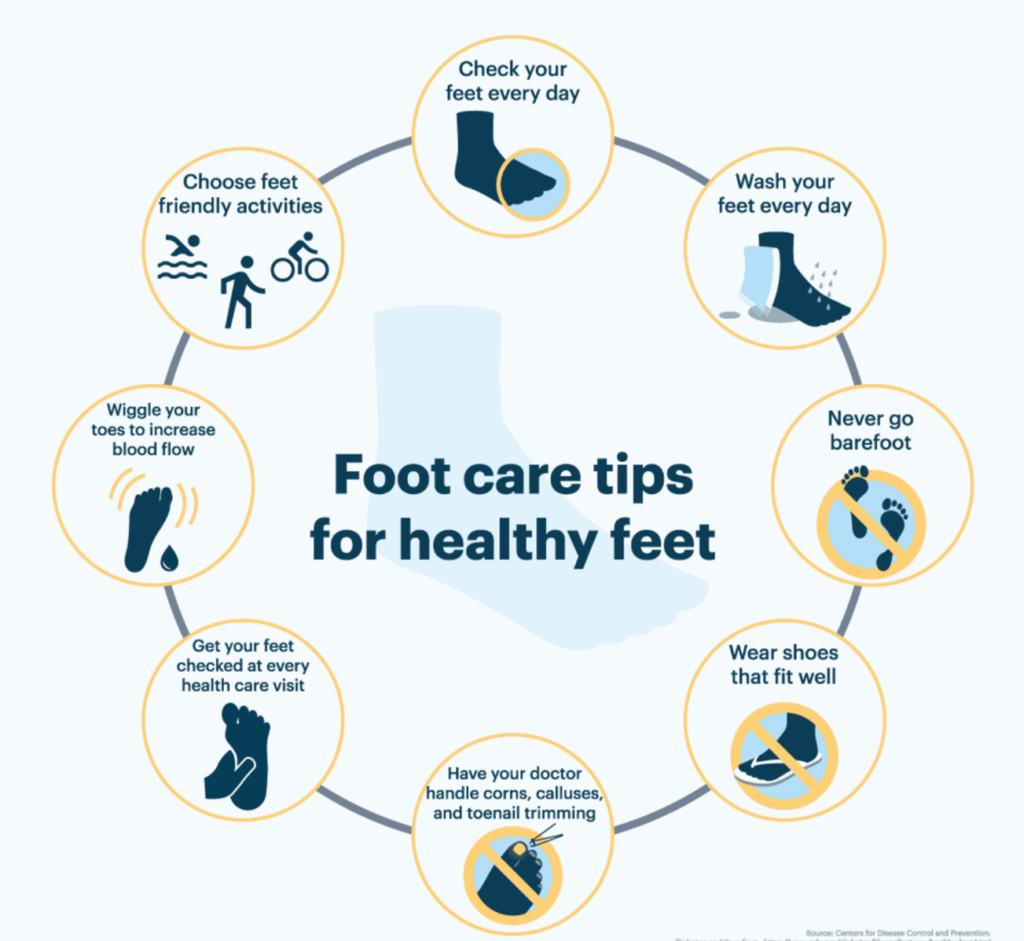
Diabetic foot ulcers and complications can be prevented with daily foot care. These are some important guidelines to follow in footcare every day to avoid these ulcers:
- Check feet daily: cuts, sores, redness, swelling, blisters, corns, or calluses. Have an inspection of every part such as soles, and between toes with a mirror or assistance.
- Wipe feet every day in warm (not hot) water with mild soap. Wipe feet completely and between toes to avoid fungi.
- Wet daily and do not touch the areas between toes to avoid cracks and drying without excessive moisture.
- Clean toenails straight at the edges and file them to avoid ingrowth. Do not cut corn or calluses yourself.
- Do not walk barefoot, not even indoors. Wear breathable socks and well-fitting shoes with cushioned soles to save feet.
- Wear natural-fiber (cotton, wool) socks, without seams fractioning. Change socks daily.
- Select shoes that have a wide toe space and lack tight seams; custom orthotics may be advised by a podiatrist.
- Manage blood sugar levels to enhance healing and decrease nerve and circulation injury.
- Regularly visit a healthcare provider to have their feet examined and treated early.
These everyday routines assist in the timely detection and elimination of dangers to prevent foot ulcers and other severe issues, such as infection and amputation.
Choosing Proper Footwear
The use of appropriate footwear plays a vital role in the prevention of diabetic foot ulcers and the preservation of the health of the feet of diabetics. These are some of the major factors and guidelines in choosing the right shoe:
Good Fit: The shoes must fit snugly, with no more than half an inch between the longest toe and the tip of the shoe (1.3-1.6 cm). They must fit the foot shape (width, depth, and volume) without creating pressure points or tightness.
Support and Cushioning: Shoes should be well-cushioned and supportive particularly in the sole and arch to minimize pressure and shear forces on the feet. High-risk individuals are proposed to use therapeutic or orthotic footwear with custom insoles.
Heel height: 2.5-5 cm heel height is ideal. Heels more than 5 cm elevate the pressure on the forefoot and should be avoided.
Materials: Breathable soft fabrics such as leather or mesh do not cause irritation and keep feet dry. Seamless-soled shoes minimize friction that leads to blisters or ulcers.
Sole and Pressure Offloading: Rigid rocker soles special soles may be used to minimize pressure applied to ulcer-prone regions and aid healing by preventing the foot and shear.
Adjustable Closures: Velcro straps or laces permit a secure, adjustable fit to swelling or foot changes over the day.
When to Shop: Shopping for shoes later in the day when feet are likely to swell is best so that they fit well under normal conditions.
Professional Advice: It is advisable to visit a podiatrist or foot care specialist to obtain personalized footwear suggestions, particularly to patients with a history of foot deformities or ulcers.
Digital feet wear minimizes the threat of ulcers as it prevents skin pressure, friction and damage, and can appropriately adapt to the demands of diabetic feet.
You may also like to read: Importance of Foot Care
Managing Minor Foot Problems Quickly
To treat minor cases of diabetic foot promptly and efficiently, the following measures are prescribed:
- Wash and dry the place: Check feet daily about the possibility of cuts, blisters, sores, redness, or swelling. Wash minuscule injuries with tepid water and gentle soap, without using hot water or saturation.
- Dry well: Dry feet after washing, in-between toes, to prevent fungal infections.
- Keep the skin moist: Rub lotion on to keep the skin dry and cracked but not between toes because moisture may cause infections.
- Keep minor cuts or sores clean: Use clean dry dressing on small wounds and change it frequently to keep that area clean and heal.
- No pressure and irritation: Take pressure off the affected part by wearing loose shoes or walking without shoes. Wear cushions, snug shoes or padding.
- Signs of infection: Observe redness, swelling, warmth, foul odor, or discharge, which should be reported immediately.
- Clip toenails neatly: To avoid ingrown nails, trim nails and smooth edges.
- Early professional assistance: When wounds do not improve, deteriorate, or there are symptoms of infection, contact a health professional to avoid severe complications.
Early awareness of minor foot problems via extensive daily observation, wound management, pressure relief, and early medical treatment assistance in avoiding the development of severe diabetic foot ulcers and infections.
When to Seek Medical Help
Diabetic foot issues should also be medically assisted as soon as any suspicious signs or symptoms are present, which means that it may be ulcerated or infected. Major causes to consult a doctor include:
- Unhealing open foot ulcers or sores or not getting better.
- Symptoms of infection: redness, swelling, warmth, pus, foul odor or discharge of a wound.
- Foot pain or tenderness, particularly new or aggravated.
- Foot tissue discoloring, such as whiteness, blue, black or dead tissue (gangrene).
- Blood or hemorrhage on socks or shoes.
- Ulcer-precursors on big toes such as big calluses, blisters or cracked heels.
- Numbness, tingling, or numbness with new wounds or injuries.
- Fever or chills with the indication of systemic infection.
- Foot defects or alteration of foot form, such as swelling or heat, which can be signs of Charcot foot.
Gangrene (dead tissue because of no blood flow) or deep infections may also be life or limb-threatening, requiring immediate emergency care. Timely recognition and management of diabetic foot ulcers and infections greatly lower chances of hospitalization, amputations and mortality. Foot checks should be performed by medical professionals regularly to prevent and risk-assess.
Final Thoughts
Simple yet regular foot care is the beginning of diabetic foot ulcer prevention. Footwear, proper hygiene, and daily inspections can help a lot in preventing severe complications. Proactive measures and visiting a doctor when necessary can help individuals with diabetes preserve their feet, move around, and sustain their health.