Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
One of the most frequent and severe effects of diabetes is diabetic retinopathy, which targets the minute blood vessels of the retina of the eye. When unattended, it may result in eye defects and even blindness. Knowing the causes, early symptoms, and the treatment options available are very crucial measures for safeguarding the eye health of any diabetic person.
What is Diabetic Retinopathy?
Diabetic retinopathy is a diabetes complication affecting the eyes. It is brought about by the injury of blood vessels in the sensitive tissue in the back of the eye known as the retina. The damage is because of the high blood sugar, which damages the small blood vessels in the retina, resulting in leakage, swelling, or irregular growth of blood vessels.
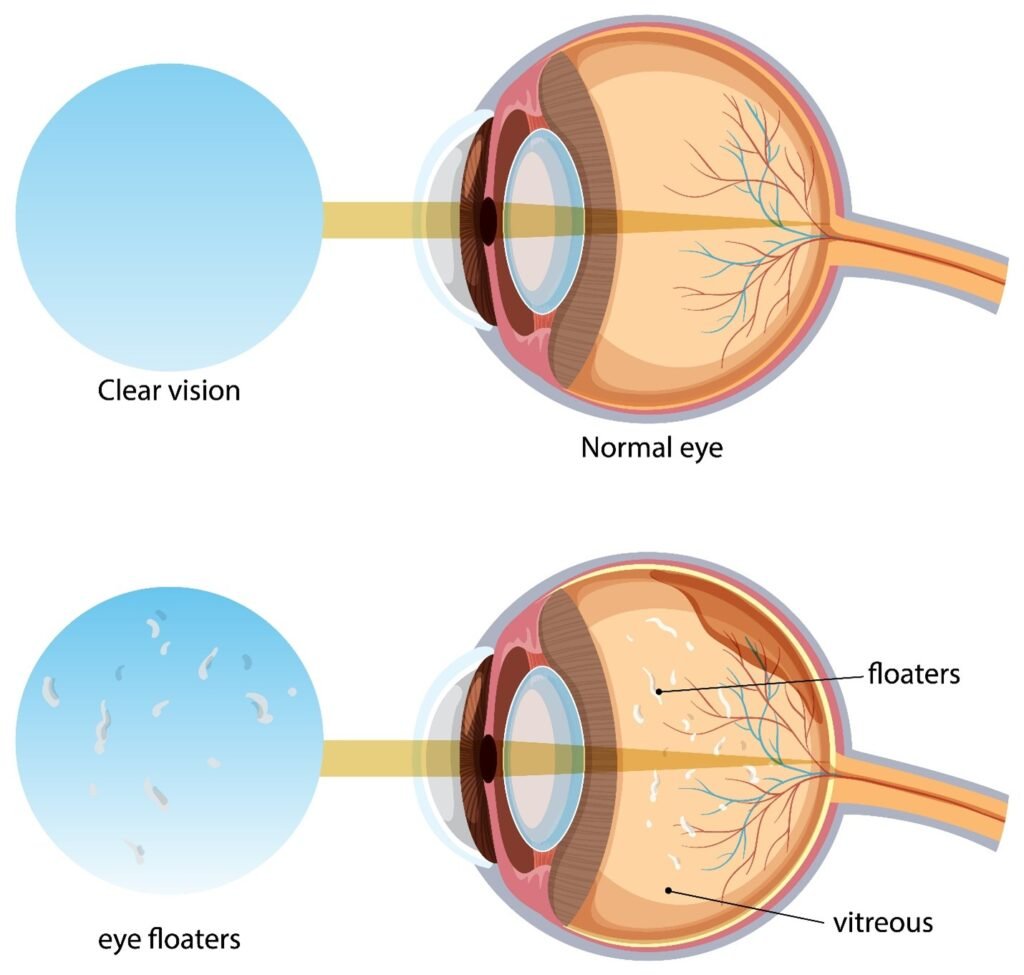
At its initial phases, diabetic retinopathy can have no symptoms or mild vision issues, which include floaters, blurred vision, or dark spots. When not treated, it may advance blindness or extreme loss of sight. The risk is augmented by the period of diabetes and the absence of control of blood sugar.
Causes
High blood sugar (glucose) levels, which are caused by diabetes, are the main cause of diabetic retinopathy. In the long run, this surplus sugar destroys the tiny blood vessels that supply the retina causing them to weaken, block and leak.
The major mechanisms and causes are:
- Damage and weakening of blood vessels in the retina resulting in small dots (microaneurysms) that can leak fluid or blood into the retina.
- Obstruction of blood vessels in the retina resulting in ischemia in the retina.
- In reaction to obstructed vessels, new abnormal blood vessels develop (proliferative diabetic retinopathy). These are the new vessels which are weak and liable to leakage and bleeding.
- Macula edema (fluid in the macula) leads to swelling and vision loss.
- Chronic high glycemia activates processes leading to oxidative stress, inflammation, and vascular impairment in retinal tissue.
Other risk factors that lead to the development and progression of diabetic retinopathy are poor glycemic control, high blood pressure, obesity, elevated cholesterol, smoking, nephropathy, hormonal effects, and genetic factors.
Symptoms
The symptoms of diabetic retinopathy often do not appear in the early stages. When symptoms develop, they can include:
- Spots or dark strings floating in the field of vision, called floaters.
- Blurred or distorted vision.
- Changes in vision quality, including difficulty seeing in low light or darkness.
- Dark or empty areas in vision.
- Impaired color vision, including colors appearing faded or washed out.
- Poor peripheral (side) vision.
- Nearsightedness or farsightedness and fluctuating vision.
- Gradual worsening of eyesight, which can eventually lead to vision loss.
It can affect one eye or both eyes and the symptoms are likely to exacerbate as the disease advances. Blurry or spotty vision, sudden changes in vision are symptoms to be taken to the doctor. Early detection through frequent eye tests is crucial because the symptoms at early stages could either be absent or mild.
Diagnosis of Diabetic Retinopathy

Diabetic retinopathy is mostly diagnosed by thorough dilated eye examination where eye care specialists apply drops to dilate the eyes to aid in further inspection of the retina to assess any signs of damage.
Common diagnostic methods include:
- Dilated Eye Exam: Drops are used to enlarge the pupils to enable a closer look at the retina and blood vessels detecting abnormalities such as microaneurysms, hemorrhages and leakage.
- Optical Coherence Tomography (OCT): This is a non-invasive test of the retina, which forms cross-sectional images of the retina, visualizing its thickness and fluid accumulation or swelling (macular edema).
- Fluorescein Angiography: A dye is given into an arm into a vein, and images are made as the dye passes through the blood vessels in the retina indicating blocked, broken or leaking vessels.
- Visual Acuity Testing: Tests the clearness and sharpness of the vision.
- Slit Lamp Examination and Ophthalmoscopy: To take a closer look at the various aspects of the eye such as the retina and the existence of unwanted blood vessels.
Further examinations can determine systemic variables such as HbA1c results to check blood sugar regulation and retinopathy developmental risk factors.
You may also like to read: Role of Artificial Intelligence in Diabetes Management
Treatment Options
Diabetic retinopathy can be treated based on severity and presentation. Common treatments include:
· Laser Photocoagulation: Diabetic retinopathy (PDR)- Proliferative-type-only; diabetic macular edema (DME). Panretinal photocoagulation (PRP) uses laser spots on the peripheral retina to inhibit the abnormal growth of vessels whereas focal/grid laser uses laser on leaking blood vessels in the macula to reduce swelling. This cure allows one to avoid serious vision loss.
· Intravitreal Injections: VEGF-inhibitory drugs (anti-VEGF) (e.g., ranibizumab, aflibercept, bevacizumab) are injected into the eye to prevent VEGF, which stimulates abnormal vessel development and leakage. To inhibit inflammation and macular edema, corticosteroid injections could also be applied. These injections are frequently repeated.
· Vitrectomy Surgery: It is done in severe cases when there is vitreous bleeding or detachment of the retina. The doctor removes blood/scar tissue out of the vitreous cavity and fixes the retina. This is normally used in cases of serious diseases where other medicine proves to be ineffective.
· Medications: Oral medications such as fenofibrate can reduce the risk of progression, particularly in non-proliferative diabetic retinopathy.
Systemic treatment of blood sugar, blood pressure, and cholesterol is also essential in the management of these eye treatments to reduce the rate of disease progression.
Bottom Line
Diabetic retinopathy is a gradual eye disease that may be very severe unless treated in its early stages. With proper control of the blood sugar levels, regular eye check-ups, and prompt treatment, diabetes patients can significantly lower the chances of losing their sight. Concern and active care are the best instruments in maintaining healthy eyesight.