Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
The term “Type 3 diabetes” arouses interest and perplexity in both medical discourse and public searches. Although not classified by major health organization as a separate form of diabetes, it is frequently used in two different contexts. First, it discusses a hypothesis that indicates reduced glucose metabolism that may be a contributing factor to cognitive loss and links Alzheimer’s disease to insulin resistance in the brain.
Second, it is usually misdiagnosed as Type 3c Diabetes, known illness brought on by pancreatic damage. Patients and even healthcare professionals misunderstand each other because of this language overlap. Raising awareness, promoting early diagnosis, and enhancing proactive health management all depend on an understanding of the variances and the research underlying each interpretation. This article examines the true definition of Type 3 Diabetes, it relates to pancreatogenic diabetes and Alzheimer’s disease, and the latest finding.
What is Type 3 Diabetes?
When pancreatic damage affects both its endocrine (hormone) and exocrine (digestive enzyme) functions, type 3c diabetes, also known as pancreatogenic diabetes, occurs.
Major health organizations like the ADA and WHO do not formally recognize type 3 diabetes, regardless of its common use. This term frequently brings confusion among people and even healthcare providers because it traverses two completely different medical contexts. This is a more vivid breakdown:
Informal Usage in Medical and Academic Circles
In casual scientific discussion, this type of diabetes is used to refer to either:
- Alzheimer’s disease may be exacerbated by an insulin-resistant brain (a descriptive theory, not a formal diagnosis).
- Type 3c diabetes, also known as pancreatogenic diabetes, is a real ailment that results from injury to the pancreas.
Overlap in Terminology
- Although glucose dysregulation is present in both situations, the underlying causes, signs, and therapies are entirely different.
- To prevent misdiagnosis, it is crucial to distinguish between pancreatic illness and the brain-related theory because they have the same informal term.
Causes
Common triggers include:
- Cystic fibrosis
- Pancreatic cancer
- Chronic or acute pancreatitis (most common cause)
- Pancreatic surgery or removal (partial or total pancreatectomy)
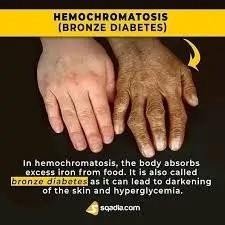
- Hemochromatosis (iron overload)
Signs and Symptoms
Individuals who have type 3c diabetes frequently have a combination of:
Typical diabetes symptoms:
- Increased thirst, frequent urination, unexplainable weight loss, fatigue, and blurred vision, etc.
Digestive/exocrine symptoms due to pancreatic insufficiency:
- Bloating, abdominal pain, gas, diarrhea or oily (fatty) stools and unintended weight loss.
Diagnosis and Management
Diagnosis
Step 1: Use tests such as the HbA1c or fasting blood sugar to confirm diabetes.
Step 2: Use imaging (CT, MRI, or endoscopic ultrasonography) and signs of exocrine insufficiency (such as low faecal elastase) to confirm pancreatic injury.
Step 3: Use autoantibody testing to rule out Type 1 diabetes.
Management
- Insulin therapy and/or oral drugs (like metformin) to manage blood sugar, depending on residual function.
- Support for digestion with pancreatic enzyme replacement treatment, specifically in cases of exocrine insufficiency.
- Handle underlying damage by treating conditions like cancer, cystic fibrosis, or pancreatitis.
You may also like to read: Is Diabetes a Disability?
Key Differences Between Alzheimer’s-Type and Type 3c Diabetes
Although both disorders are sometimes referred to as “Type 3 Diabetes”, their signs, causes, and therapies are completely different. Understanding the difference is essential for precious diagnosis and suitable treatment. Here is a thorough comparison:
| Aspect | Alzheimer’s-Type Diabetes | Type 3c Diabetes (Pancreatogenic Diabetes) |
| Recognition Status | Not officially recognized as a medical condition | Officially recognized type of diabetes |
| Cause | Insulin resistance in the brain; possibly linked to Alzheimer’s | Damage to the pancreas due to pancreatitis, cancer, or surgery |
| Primary Organ Affected | Brain | Pancreas |
| Symptoms | Memory loss, cognitive decline, confusion | High blood sugar, digestive issues (diarrhea, weight loss) |
| Diagnosis Method | No formal diagnostic criteria; based on Alzheimer’s and diabetes link | Blood tests, pancreatic imaging, enzyme analysis |
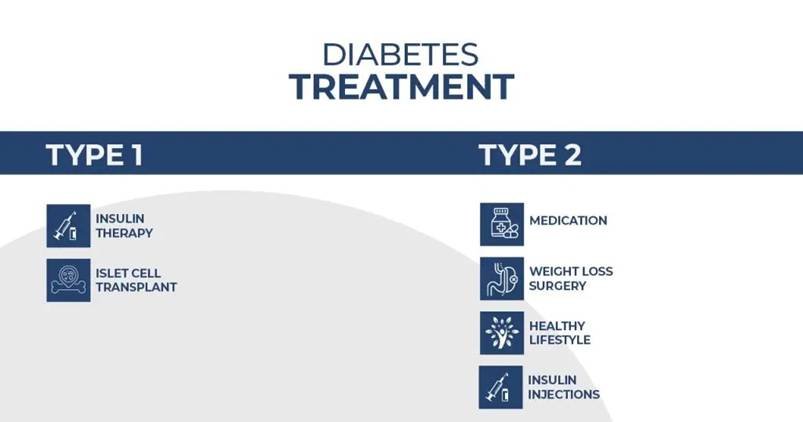
| Treatment | Alzheimer’s-specific treatment; lifestyle changes for insulin sensitivity | Insulin therapy, pancreatic enzyme replacement, diet adjustments |
| Medical Term Used | Descriptive term only | Also called Type 3c Diabetes or pancreatogenic diabetes |
| Common in | Older adults, especially those with type 2 diabetes | People with a history of pancreatic disease or surgery |
How to Manage and Reduce Risk
The following are proven strategies for managing and lowering the risk of Type 3 diabetes, which is linked to Alzheimer’s disease, and Type 3c (pancreatogenic) diabetes:
Lifestyle for Brain Health
Reducing insulin resistance in the brain and possibly delaying cognitive decline can be attained by leading a brain-focused lifestyle:
Healthy Diet:
- Diets high in fruits, vegetables, whole grain, fish, olive oil, and nuts, sometimes known as the Mediterranean or MIND diet, relate to enhanced cognitive function and a decreased risk of dementia.
- Intake of food high in choline (such as eggs, cruciferous vegetables, and dairy) and omega-3 sources (like walnuts and salmon) as these have been shown to enhance cognitive and memory performance.

Regular Exercise
- Both aerobic and strength training enhance insulin sensitivity (including in brain cells) and reduce dementia risk by rough 20%.
Quality sleep & stress control
- Make getting 7 to 9 hours of good sleep, specifically REM sleep, an obligation for memory consolidation and toxin removal.
- To maintain neurological function, reduce stress before bed by practicing mindfulness, meditation, or gentle stretching.
Final Thoughts
The terminology Type 3 Diabetes is applied in two different contexts: One explaining insulin resistance in the brain as associated with the development of Alzheimer, and the other one as a form of diabetes (type 3c) due to damage of the pancreatitis. Both raise very serious medical issues despite only Type 3c being an officially accepted illness. Knowledge can be utilized to determine appropriate intervention and care by identifying these differences.