Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Good diabetes management calls for tight control of blood glucose levels; therefore, insulin distribution helps greatly in attaining that balance. Often known as insulin pump therapy, continuous subcutaneous insulin infusion (CSII) has become a sophisticated treatment that closely mimics the natural release of insulin. CSII provides better flexibility, accuracy, and comfort for people living with diabetes—particularly those who trying to keep regular glucose levels with conventional injections.
What is Continuous Subcutaneous Insulin Infusion (CSII)?
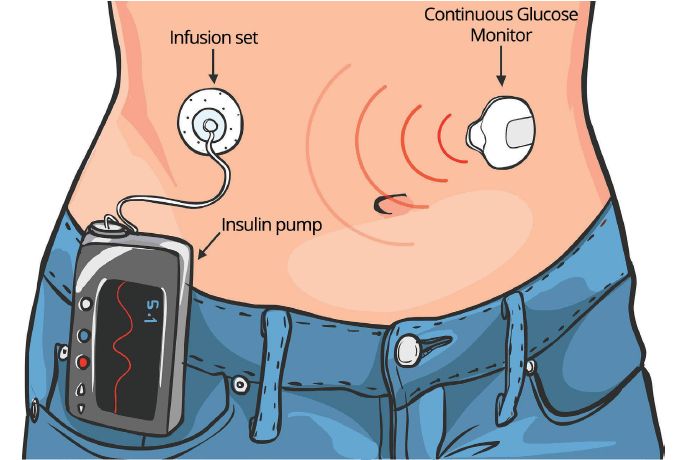
Through the skin (subcutaneous tissue), Continuous Subcutaneous Insulin Infusion (CSII) employs a tiny, portable, battery-powered pump to distribute insulin. Providing a constant background (basal) rate of insulin with additional doses (boluses) given for meals, it is meant to replicate the body’s own insulin release. Compared to several daily injections, this strategy provides more flexibility and better glycemic control.
How it works
- Usually, on the abdomen, a cannula is inserted under the skin and linked to an infusion set via a little, wearable pump.
- The pump is set to constantly provide a regular, low dose of insulin (basal rate) during both day and night.
- The pump can also be manually programmed by the user to administer a greater insulin dose (bolus) to help with meals.
- Modern hybrid closed-loop systems may interact with a continuous glucose monitoring sensor to automatically modify the basal rate.
Benefits of Continuous Subcutaneous Insulin Infusion
- Closely reproduces the way the pancreas releases insulin naturally.
- According to the National Institutes of Health (NIH) and Springer, studies demonstrate better glycemic profile and lower HbA1c may result from improved blood glucose regulation.
- More freedom in meal timing and daily activities is provided by greater flexibility.
How CSII Differs from Traditional Insulin Therapy
In its delivery method, insulin kind, and flexibility, continuous subcutaneous insulin infusion (CSII), or insulin pump treatment, sets itself apart from conventional insulin therapy—multiple daily injections (MDI). CSII employs one type of rapid-acting insulin given continuously via a pump and catheter unlike MDI, which combines numerous daily injections of long- and quick-acting insulin.
Key differences between CSII and MDI
| Feature | Continuous Subcutaneous Insulin Infusion (CSII) | Multiple Daily Injections (MDI) |
| Delivery method | An automated pump delivers insulin continuously through a small catheter placed under the skin. The pump provides a continuous trickle of insulin (basal rate), which the user can program to vary throughout the day. | Injections are manually administered using syringes or insulin pens. This method involves injecting long-acting insulin (basal) one to two times per day and rapid-acting insulin (bolus) with each meal. |
| Mimics physiological insulin | CSII more closely mimics a healthy pancreas by providing a steady supply of insulin tailored to an individual’s specific needs. This can result in less fluctuation in blood glucose levels. | This method attempts to mimic the body’s normal insulin production but is less precise and flexible than CSII. The duration of long-acting insulin and timing of meals are crucial to this process. |
| Flexibility | Offers greater flexibility with meals, exercise, and daily routines. Users can easily adjust basal rates for activities or sickness and deliver extra insulin (bolus) for meals on demand. | Requires a more rigid schedule. Insulin injections and meals must be timed consistently, which offers less flexibility in day-to-day life. |
| Hypoglycemia risk | Can potentially lower the risk of severe hypoglycemia, as the pump can be programmed to suspend insulin delivery if glucose levels drop too low. | Severe hypoglycemic events may be more frequent when compared to CSII, especially in those with frequent blood sugar lows. |
| Glycemic control | Can lead to better overall glycemic control, with studies often showing a lower HbA1c and better time-in-range for CSII users, especially in patients with suboptimal control on MDI. | Offers good glycemic control for many but can be less effective for those with highly variable blood glucose levels. |
| Patient commitment | Requires a high level of motivation, education, and commitment from the patient. Users must constantly manage the device, including changing the infusion set every few days and monitoring glucose levels frequently. | Also requires commitment to a strict schedule, but the daily tasks are generally less demanding than managing a pump. However, dosing errors can have serious consequences. |
| Cost and convenience | Has a higher upfront cost for the pump, plus ongoing expenses for supplies like reservoirs and infusion sets. The pump is a continuous device that must be worn almost constantly. | Involves lower initial costs, and ongoing expenses are limited to insulin vials/pens and needles. Some individuals prefer not to wear a device and prefer injections. |
Potential Risks and Limitations
Possible dangers of Continuous Subcutaneous Insulin Infusion (CSII) are metabolic problems such as diabetic ketoacidosis (DKA) from pump failure or set issues and skin Problems, including lipohypertrophy at the infusion site, infection, and irritation. Limitations include the risk of weight gain, the inconvenience for activities such as sports or showering, and the possibility of patient-related problems such as adverse psychological effects and user error.
You may also like to read: Role of Diet in Diabetes Management
Practical Tips for CSII Users
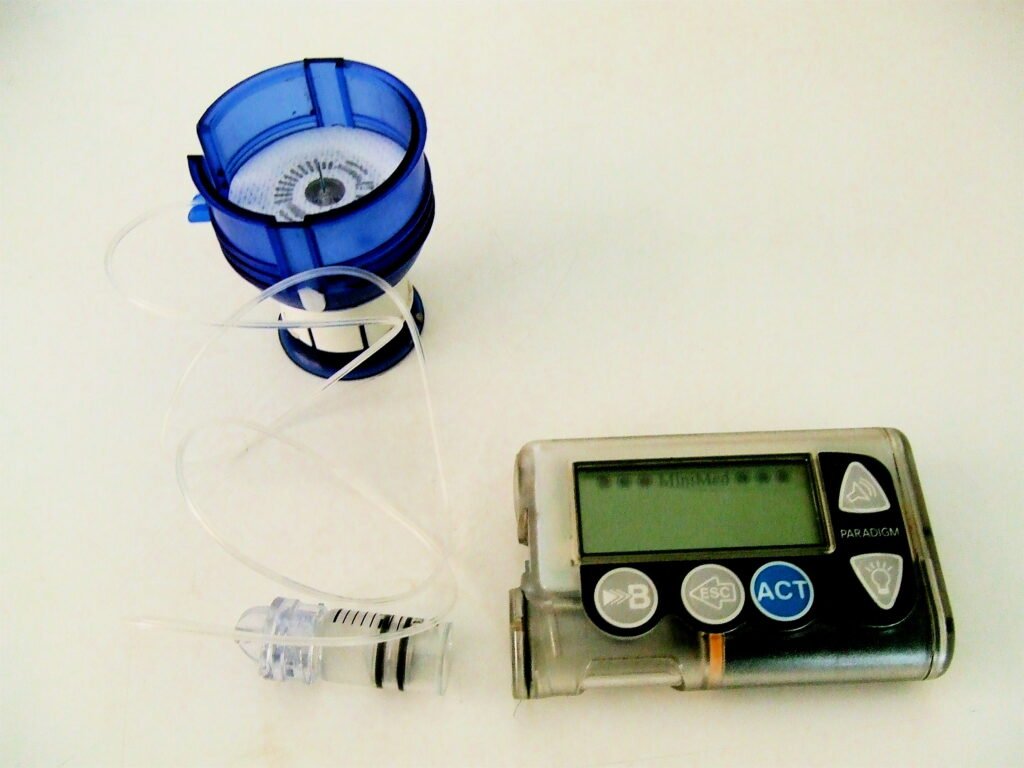
Practical suggestions for Continuous Subcutaneous Insulin Infusion (CSII) users include regular rotations of insertion sites, adequate understanding of often monitoring blood glucose levels, your pump’s configurations, and a backup plan for pump breakdown. Always keep rapid-acting carbohydrates available, understand how to manage hypoglycemia, and check in often with your medical team.
Site management and hygiene
- Before replacing an infusion set, wash your hands thoroughly with soap and water.
- More frequently, if the site becomes inflamed, switch your infusion set every 2 to 3 days.
- To prevent irritation and guarantee even absorption, turn your infusion sites. Although the thigh or hip can also be used, the stomach is a frequently used and good area.
- Get ready to contact a doctor if you see symptoms of infection, like hardness, redness, or discomfort by preparing the new collection on a clean surface.
Pump management and safety
- Keep track of your baseline rates, insulin-to-carb ratios, and correction factors in case you have to go back to manual injections.
- Get to know your pump’s alerts and what they signify. Keep in mind that the pump might not alert for a failed location that stops giving insulin.
- Never separate the pump for longer than an hour without a different insulin supply to prevent diabetic ketoacidosis (DKA).
- Shield the pump from strong radiation and electromagnetic fields, as this can damage the device.
Blood sugar monitoring and treatment
- To avoid ketosis, monitor your blood glucose levels four times a day at least.
- Before altering your pump settings, always address a low blood sugar (hypoglycemia).
- Always have fast-acting carbs for treating hypoglycemia.
- Include how to give glucagon or glucogel if necessary when sharing knowledge on how to treat a hypo with relatives or friends.
Patient and caregiver collaboration
- Include the user of the pump in their own diabetes management since they know their own body and have the expertise on their own condition.
- Ensure your healthcare staff is familiar with CSII technology and that you can communicate effectively with them.
Final Thoughts
A contemporary, adaptable, and exact way of treating diabetes is constant subcutaneous insulin infusion. It helps people reach better glucose management and higher quality of life by offering constant insulin delivery and adjustable dosing. Although CSII calls for adequate education, consistent monitoring, and dedication, its advantages typically outweigh the difficulties for those looking for a more natural and efficient means to control diabetes.
FAQs
What is the 3 hour rule for insulin?
Rapid-acting insulin (also known as Insulin Stacking) starts working around 15 minutes after injection, reaches its peak in about one hour, and Still works 2 to 4 hours. The three-hour restriction avoids “insulin stacking” and low blood glucose (BG) or hypoglycaemia.
Does CGM have a needle?
Does a CGM contain needles? Your CGMs’ accompanying CGM applicator has a little needle used to install the gadget to the rear of your arm. Once in place, a little filament linked to the sensor stays under your skin so the gadget can determine your glucose levels using interstitial fluid.
Which insulin is best for diabetes?
Long-acting or intermediate-acting insulin
Once or twice daily, this kind of insulin is taken. They might advise a kind of long-acting insulin (brand names Levemir, Lantus, Toujeo, Tresiba, If you either have frequent low blood sugar (hypoglycemia, or hypos), Semglee or Abasaglar.