Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Diabetic neuropathy is the altogether most widespread and acute issue of diabetes that affects a great number of people in the world. It happens when nerves are damaged by excess blood sugar making them accompanied by pain, numbness, or weakness in the hands and feet. In addition to pain, the condition may impede everyday functions and lead to serious health complications when ignored. This knowledge will be critical to the treatment of diabetic neuropathy and the long-term health care of diabetic patients.
What is Diabetic Neuropathy?
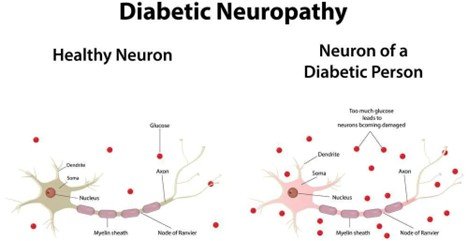
Diabetic neuropathy is the result of nerve damage that develops because of sustained elevated glucose levels over time and affects the transmission of signals between the brain, spinal cord, and the rest of the body. It can impact sensory nerves (which sense), motor nerves (which operate muscles), and the autonomic nerves (which regulate uncontrolled motions like heart rate and digestion).
Causes of Diabetic Neuropathy
Diabetic neuropathy occurs chiefly because of long-term chronically raised blood sugar level (hyperglycemia) in people with diabetes. This high blood sugar breaks nerves and damages small blood vessels (capillaries) that carry oxygen and nutrients to the nerves, causing nerve damage and dysfunction.
Additional contributing causes and risk factors include:
- Ineffective blood sugar management puts the chances and severity of nerve damage at risk.
- Chronic period of diabetes with the risk growing the longer the individual has diabetes.
- Hypertension and elevated cholesterol level, which aggravate damage of the blood vessels and nerves.
- Kidney disease (diabetes nephropathy) harbors toxins that cause further damage to womb nerves.
- The result of being overweight or even being obese constitutes metabolic stress.
- Smoking, an activity that constricts blood vessels and decreases blood flow to nerves.
- High triglycerides or fats in the blood harm nerves.
- Some genetic predispositions that can pre-dispose one into risk of nerve damage.
Symptoms
Symptoms of diabetic neuropathy vary according to the nervous system affected. Our diabetic neuropathy comes in four specific types, each with their specific symptoms:
Peripheral Neuropathy (Most Common)
- Numbness or reduced ability to feel pain or temperature changes, especially in the feet and legs.
- Tingling or burning sensations.
- Sharp, stabbing pains or cramps.
- Muscle weakness.
- Heightened sensitivity to touch, where even the lightest touch like a bedsheet can cause pain.
- Significant foot complications like ulcers, infections, damage to the bones or joints.
- Symptoms can begin in the feet and legs and become more intense at night.
Autonomic Neuropathy
- Influences autonomic functions (those effected by ANS)
- Its symptoms are a lack of warning of low blood sugar (hypoglycemia unawareness), dizziness or fainting when standing because of blood pressure drop (orthostatic hypotension), bladder and bowel problems, stomach problems like nausea, vomiting, constipation or diarrhea, slow emptying of the stomach (gastroparesis).
- Sexual dysfunction like erectile dysfunction as well as vaginal dryness
- Variations in the faculties of sweating and impaired reaction of the heart rate.
Proximal Neuropathy (Diabetic Amyotrophy)
- Sudden, sharp pain in the hips, thighs, buttocks or legs, usually unilateral.
- Weakness of the muscles and distress in getting up after sitting posture.
- Symptoms are contagious and Iggy: they get better eventually.
Focal Neuropathy (Mononeuropathy)
- It involves destruction of one nerve or sets of nerves.
- Acute pain or weakness of a particular body part like the face, torso, arm or leg.
- Symptoms are possible to be double vision, lack of the ability to move facial muscles, pain or weakness of a particular limb or an area, and carpel tunnel syndrome symptoms.
Symptoms appear slowly in most cases and are mild or severe. Preventing progression starts by early detection and treatment to control symptoms.
Risk Factors for Developing Diabetic Neuropathy
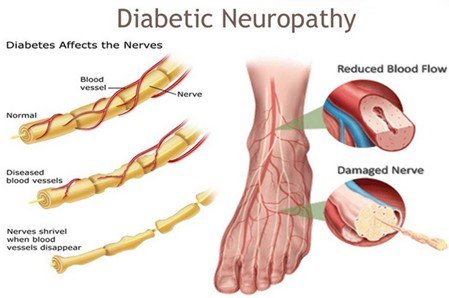
The main risk factors for developing diabetic neuropathy include:
- Ineffective blood sugar control: High, consistent levels of glucose worsen and increases the likelihood of nerve damage. The chronic elevated A1C levels are strongly associated with neuropathy.
- Long term diabetes: The risk is greater with the number of years the person has diabetes, often after 10-15 years.
- Kidney disease: Diabetic kidney damage causes toxins to be built up in the blood, which destroys nerves.
- Obesity or overweight: Obesity or being overweight increases the risk of neuropathy.
- Smoking: Smoking constricts blood vessels and hinders blood flow to the nerves, injuring them and slows wound healing.
- Blood pressure and high cholesterol: Both are associated with the damage of vessels aggravating the health of nerves.
- Age: The older age promotes the potential of nerve damage.
- Other causes: Diabetic complications like eye damage (retinopathy) and changes in metabolism like dyslipidemia would also put you at risk.
Diagnosis
Diagnosis of diabetic neuropathy entails a mixture of clinical assessment, patient history, and specialized tests to support nerve damage and the measuring of the side effects.
Clinical Evaluation
- Specific symptoms history, such as numbness, tingling, burning, pain, muscle weakness.
- Physical assessment with special emphasis on sensation (light touch, pinprick, vibration, heat), reflexes (reflexes (specifically, ankle jerks), and strength tests.
Screening Tools
- Michigan Neuropathy Screening Instrument (MNSI): A combination of both patient questionnaire and physical examination to screen peripheral neuropathy.
- Symptomatology The Neuropathy Symptom Score (NSS) and the Neuropathy Disability Score (NDS) evaluate symptom severity and neurological function.
Electrophysiological Tests
- Nerve Conduction Studies (NCS): This is considered the gold standard, and it is used to measure the strength and speed of electrical messages in peripheral nerves. Handy especially in large fiber neuropathy.
- Electromyography (EMG): The electrical activity of a muscle, and the signal transmitted by a nerve to the muscle, can be measured.
Quantitative Sensory Testing (QST)
Tests the response of the small and large nerve fibers using stimulus of vibration, temperature and pressure. It helps diagnose the early nerve damage.
Specialized Tests
- Skin biopsy to measure intra-epidermal nerve fiber density (IENFD), which is especially useful to diagnose the small fiber neuropathy.
- Corneal confocal microscopy (CCM) as a promising non-invasive technique to image small nerve fibers in the cornea.
Additional Tests
- Blood tests to eliminate other non DPP causes of neuropathy (ex. vitamin deficiencies, thyroid function).
- Evaluation of blood sugar control and diabetes complications.
Treatment
There is no cure to diabetic neuropathy, and treatment is aimed at controlling symptoms, halting illness, and enhancing quality of life.
Key Treatment Approaches
Blood Sugar Control
- In type 1 diabetes, tight control of glucose slows, or even halts, the progression of nerve damage. The data on type 2 diabetes is inconclusive, but it is generally accepted that blood sugar should be kept within individualized target ranges (usually A1C at 7.0 percent or below).
Pain Management
- Medications for neuropathic pain include:
- Antidepressants: Duloxetine, amitriptyline.
- Anticonvulsants: Pregabalin, gabapentin (FDA-approved).
- Opioid-like drugs (used cautiously): Tramadol, tapentadol.
- Topical agents: Capsaicin cream, lidocaine patches.
- Neuromodulation methods such as spinal cord stimulation are emerging possibilities of severe, refractive pain.
Symptom Relief and Supportive Care
· Heralded conditions such as blood pressure and cholesterol and obesity management contribute to the health of nerves overall.
· Occupational therapy, along with physical therapy, may increase mobility and functioning.
· The symptoms and overall, wellbeing are alleviated by lifestyle changes such as stopping smoking, exercising and adopting proper diet.
Pathogenetic Treatments (Targeting Underlying Nerve Damage)
- Antioxidants such as alpha-lipoic acid.
- Benfotiamine to prevent vascular damage.
- Inhibitors of the polyol pathway include aldose reductase inhibitors that are under development.
Advanced Therapies
Pancreas or islet cell transplantation in type 1 diabetes has limited nerve functional improvement but is impeded by its availability and risks.
You may also like to read: Metabolic Acidosis
Complications of Untreated Diabetic Neuropathy
- Loss of Sensation and Injuries: The loss of feeling in feet and legs nerve damage does not notice cuts, blisters, and sores easily.
- Infections and Ulcer: A sore with minor infection heals slowly and, in some cases, leads to gangrene and amputation.
- Autonomic Dysfunction: Cause of bladder problems, blood pressure, digestive problems (gastroparesis, diarrhea, constipation), and sexual dysfunction.
- Risk of falls: Lightheadedness, muscle loss, and poor coordination result in an increased risk of falls and injuries.
- Cardiovascular Issues: Cardiovascular Issues: May initiate heart rhythm disorders and silent heart attacks.
- Disability and Chronic Pain: Chronic nerve pain affects daily functionality, mobility and mental health.
- Increased Risk of Death: The patients with neuropathy, particularly those with ulcers on their feet are at risk of dying prematurely.
Bottom Line
Diabetic neuropathy is a severe consequence of diabetes which may severely affect the quality of life when not approached early. People with diabetes can enhance nerve protection by knowing their risk factors, spotting warning signs, and addressing them to prevent chronic complications. Controlling blood sugar, a healthy lifestyle, and adherence to the recommendations of a medical worker are steps to reduce risks. Diabetic neuropathy can be managed with prevention and proper care and live a healthy and safe life.