Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Having diabetes does not only entail checking blood sugar but also taking care of the feet. Foot ulcers are among the worst complications diabetics can get, as they may become infected and result in amputation without treatment. The positive is that this risk can be significantly decreased with proper foot care. Daily foot checks and healthy habits can help people with diabetes to keep their feet safe and enjoy a higher quality of life.
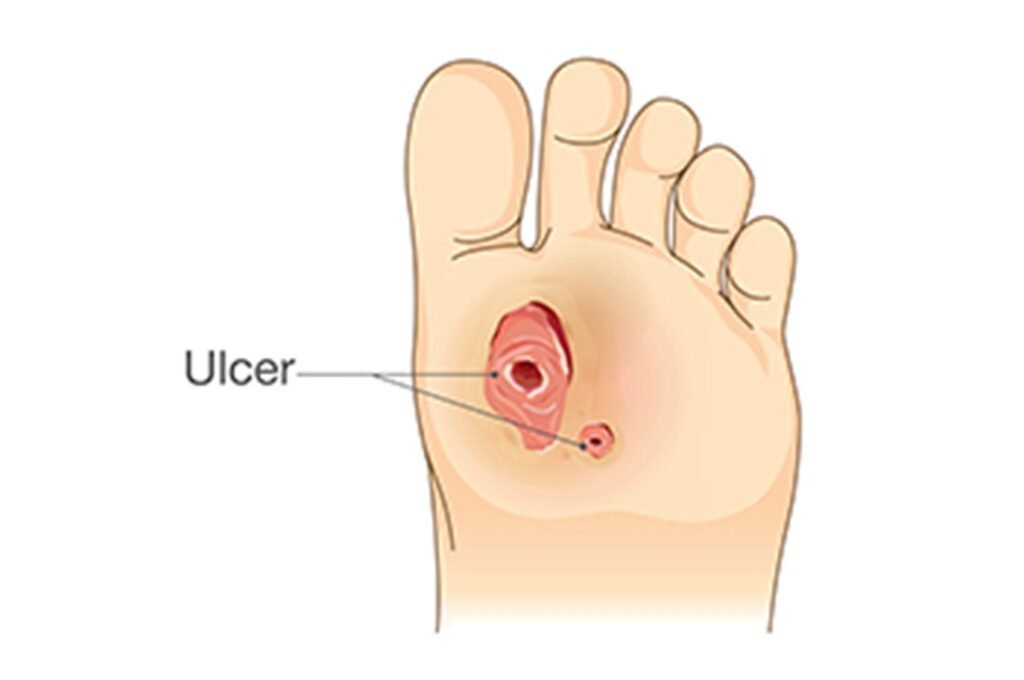
Understanding Diabetic Foot Ulcers
A diabetic foot ulcer is an exposed wound or sore on a foot whose underlying cause is diabetes. It occurs because of the combination of multiple factors such as peripheral neuropathy (damage to nerves), poor circulation (ischemia), foot defects and recurring pressure or trauma. Neuropathy decreases sensation, i.e. injury or pressure, which leads to the ulcer not being noticed and untreated. Low circulation also worsens recovery and risks infection. They are severe complications of diabetes and may result in infection, hospitalization, and amputation unless timely and adequately treated.
Why Foot Care Matters for Diabetics
Foot care is very important to individuals with diabetes since diabetes can lead to nerve damage (neuropathy) and poor circulation, both of which increase the likelihood of foot injuries not being noticed and not healing. Damage of nerves lowers the sensation of pain, heat, or cold, thus simple cuts, blisters, or sores may turn into severe infections before they are noticed. Healing and the ability to combat infection are further affected by poor blood flow. Consequently, ulcers, infections, and even amputations may result when diabetic foot wounds are not properly tackled.
Good foot care prevents these complications by promoting early detection of injuries through daily inspection, skin hygiene and moisture, foot protection through footwear and socks, and frequent check-ups. Socking and shoing feet prevent unseen trauma injuries even at home. Better foot health is also facilitated by management of blood sugar and general control of diabetes. Various studies indicate that active foot care and early interventions decrease the chances of severe infections and amputations. Foot care will therefore be critical component of diabetes self-management to sustain mobility and quality of life.
Essential Foot Care Practices to Prevent Ulcers
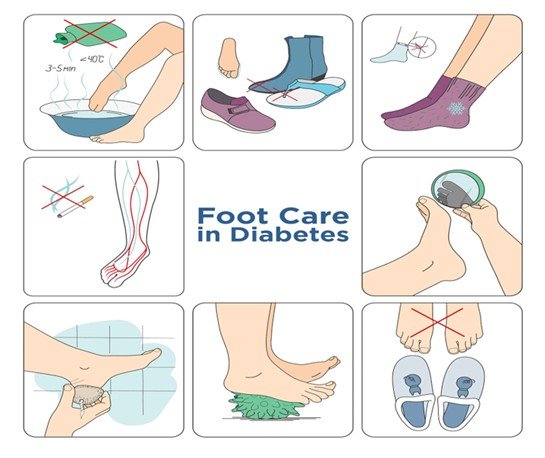
Essential foot care practices to prevent diabetic foot ulcers include the following key measures:
- Daily Foot Inspection: Inspect both feet daily to observe any cuts, blisters, redness, swelling or any evidence of injury or infection. Look at the soles with a mirror. Early diagnosis aids in the treatment of problems before they aggravate.
- Foot Hygiene: Wash feet with lukewarm water daily, dry them completely between toes, and keep skin moist to avoid cracks. Do not keep feet long soaked or rub them with harsh chemicals.
- Dress Shoes: Use well-fitting shoes that are not tight or loose and high-heeled shoes. Wear clean and dry socks in place of tight bands and never walk barefoot to avoid injury.
- Frequent Nail Maintenance: Clip toenails in a straight line and do not dig into corners to prevent ingrowth and infection of nails.
- Pre-ulcerative Signs: Calluses, blisters, fissures, fungal infection, ingrown nails should be treated promptly and with proper care or professional assistance.
- Pressure Offloading: Special footwear, insoles or orthotics are used to alleviate pressure in specific areas that may have foot deformities or those with a history of ulcers.
- Blood Sugar and Health Control: Achieve a good level and control of diabetes and vascular risk factors such as smoking cessation to promote healing and prevent complications.
- Foot Screening and Education: Professional foot examinations and patient education on foot care lower risk of ulceration by supporting good habits and watching at-risk feet.
The combination of these practices decreases the chances of getting foot ulcers, helps avoid minor injuries that evolve, and reduces the complications of infections and amputations.
Warning Signs Not to Ignore
Warning signs not to ignore for diabetic foot ulcers include:
- Redness and Tenderness: Early inflammation with resultant skin redness and swelling with or without pain or discomfort on touch.
- Swelling: Localized swelling of the foot or ankle may be accompanied by warmth and tightness.
- Constant pain or discomfort: Worsening pain with pressure or walking.
- Cracked or Dry Skin: Undue dryness that results in cracked skin is a source of infection.
- Blisters: Can begin in white or fluid-filled blisters which can progress into ulcers when left untreated.
- Open Sores or Wounds: A sore that does not heal or becomes worse, may drain fluid or pus.
- Slow Wound Healing: Wounds or ulcers that do not end in weeks.
- Drainage on Socks or Shoes: Pus, blood, or fluid noticeable on sock or shoes showing an infected ulcer.
- Skin Color: Discoloration (brown, black, blue, red, or purple) of the skin can result in poor circulation, tissue death, or gangrene.
- Foul odor: A malodorous smell can indicate an infection or necrosis of tissue.
- Fever and Chills: Body systems symptoms of spreading infection.
Early detection and prompt medical care is critical to avoid severe infection, complications and even amputation. All these symptoms should be evaluated urgently by a healthcare expert in diabetic foot management.
You may also like to read: Pathophysiology of Diabetic Nephropathy
Lifestyle Habits That Support Foot Health
Foot lifestyle choices in diabetic patients aim to prevent injury to feet, preserve skin integrity, and improve general circulation. Key habits include:
- Foot care and inspection: my plan is to inspect my feet daily (cuts, blisters, redness or swelling), to identify issues early. Feet must be washed everyday using mild soap, lukewarm water and dried thoroughly between toes to avoid fungus. Wetting the skin frequently can help to avoid dryness and cracking, but lotion should not be used between toes to prevent moisture build-up.
- Wear Shoes and socks: It is important to always wear shoes that offer protection and support, even in the house. Socks must be clean, dry, well-fitting and ideally of moisture-wicking materials like wool or synthetic blends. Wear shoes to avoid unnoticeable wounds.
- Nail Care: Cut toenails straight and file the sharp edges to prevent ingrown toenails that may lead to infection.
- Blood Sugar Control: Proper glycemic management prevents nerve damage and improves circulation, lowering foot complication risks.
- Exercise: Exercise enhances blood circulation to the lower extremities and general nerve condition. Exercise of the feet in comfortable shoes prevents new injuries.
- Stop Smoking: Smoking constricts blood vessels, slows healing, and heightens the likelihood of complications.
- Regular Health Check-ups: The healthcare provider should regularly check the feet annually, and foot orthotics should be prescribed when necessary.
- Keep Feet out of Extremes of Temp: Do not put feet in hot or very cold areas, as the loss of sensation can lead to burns or frostbite.
Adhering to this lifestyle habits can significantly reduce foot complications, ulcers, and even amputations in diabetes by preserving foot health and detecting problems early.
Bottom Line
The complication is diabetic foot ulcers which can be prevented by consistent foot care. Simple routines like my daily checks, hygiene, wearing supportive shoes and regular checkups with the doctor can contribute a lot. Through remaining proactive and sensitive to foot care, diabetics can prevent severe issues, retain their mobility and health, and safeguard their well-being. Your current foot care is a future investment in your health.