Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
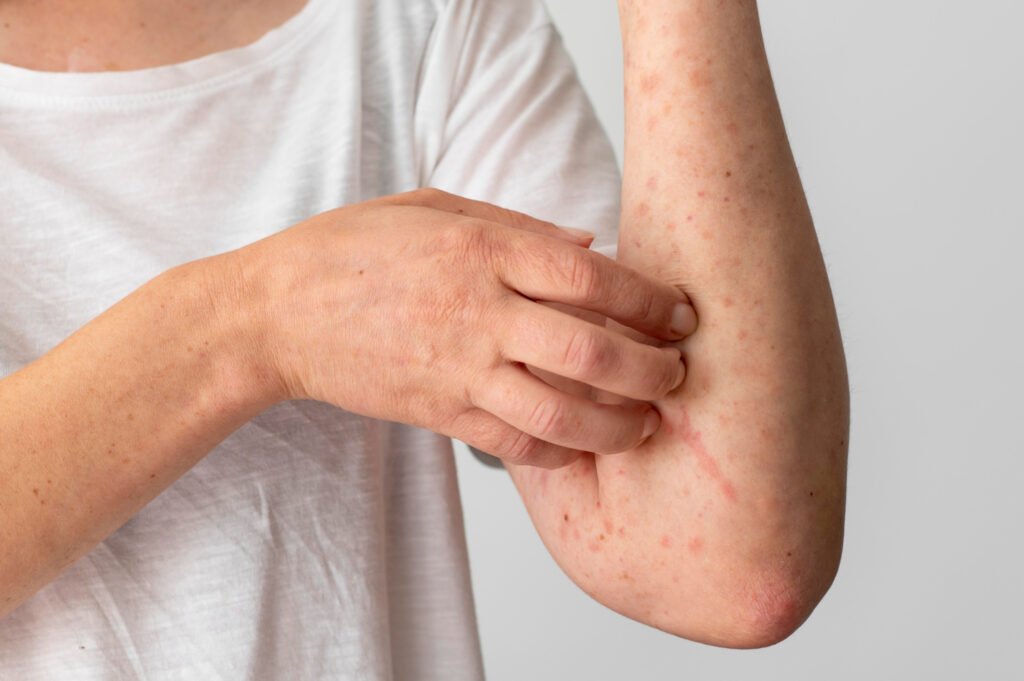
Keratosis pilaris is a painful skin disorder that is quite frequent and has harmless, small rough bumps on the skin surface. It is also known as chicken skin and is typical on upper arms, thighs, cheek or buttock and may cause unevenness of the skin or skin drought. Although keratosis pilaris is not harmful, most individuals desire to have smooth and clear skin. The first step in managing this condition is to understand its causes, symptoms and treatment options.
What Is Keratosis Pilaris?
Keratosis Pilaris is a common, harmless skin condition characterized by small, rough bumps on the skin, often described as “chicken skin.” These bumps are caused by excess keratin, a protein that forms hair, nails, and skin’s outer layer, accumulating and plugging hair follicles. It typically appears on the upper arms, thighs, buttocks, and sometimes the face. The bumps can be skin-colored, red, brown, or white and the skin may feel dry and rough. Keratosis Pilaris is often seen in children and adolescents and generally improves with age, sometimes fading by early adulthood. While it is harmless and usually does not require treatment, moisturizing the skin and gentle skincare routines can help manage symptoms, especially dry skin. The condition has a genetic component and tends to worsen with dry skin or in cold weather but improves in warm weather.
Symptoms and How to Recognize It
Keratosis Pilaris is known to have some typical symptoms and visual appearance:
- Goosebump-like, small and painless bumps tend to occur in the upper arms, thighs, buttocks, cheeks, chest, or back. Such bumps are typically rough and may be sandpaper-like.
- The bumps may be of a skin color, red, white, pink, brown, or black, according to the skin of a person.
- The afflicted skin can be dry to rough, itchy or irritated. The bumps may be reddened or a bit inflamed, particularly when scratched.
- Keratosis Pilaris is usually aggravated during dry seasons, especially during winter and usually relieved during warm seasons.
- The disease is prevalent in children, teenagers and, in occasional cases, adults.
- Bumps are not painful but in some instances itching or pain can be experienced.
- An ingrown hair may be found in some bumps.
- The disease produces patches or scattered small bumps as opposed to diffuse rash.
Its characteristic feature which aids in its identification according to its appearance, is the rough, bumpy patches which are often referred to as chicken skin.
Causes and Risk Factors
This is caused by a deposition of keratin, a skin protecting protein, that blocks hair follicles and creates the rough, small bumps known as Keratosis Pilaris. This build-up of keratin is not completely understood as its cause, but genetics leads to it in many cases, and the condition is often familial.
Risk factors that put one in danger of developing keratosis pilaris include:
- Keratosis pilaris in family history.
- Suffers have dry skin that aggravates the condition.
- Skin disorders, such as eczema (atopic dermatitis) and ichthyosis vulgaris (excessively dry skin disorder).
- Indicating that it may be related to atopic diseases, asthma and hay fever.
- Overweight or obese body condition.
- Flare-ups triggered by hormonal changes during puberty and pregnancy.
- It is more prevalent in children, adolescents, and women.
Keratosis pilaris is not transmissible and occurs predominantly in parts of the body having hair follicles except the palms and soles. It can also be caused by vitamin A deficiency and treatment with vitamin A can be helpful. The condition normally manifests in childhood or adolescence and may pass by adulthood, though in a few cases.
Treatment and Management Options

The treatment of Keratosis Pilaris is aimed at modifying the looks and skin feel as it has no cure. Management generally entails:
- Moisturizing: It is essential to use moisturizers that are rich in emollients to hydrate and make dry and rough skin soft.
- Exfoliation: Topical creams of lactic acid, salicylic acid, urea, or alpha hydroxy acids aid the exfoliation process of the dead skin cells and keratin plugs, making the skin smoother.
- Topical retinoids: Retinoids like tretinoin or adapalene that are used by prescription stimulate cell turnover and diminish bumps.
- Topical steroids: Short term use to treat redness and itch when flare-ups occur but not as long-lasting treatment.
- Light skincare: Do not use hard soaps, tidy cleansers, tepid water and should not scrub (this will aggravate irritation).
- Lifestyle changes: Loose, breathable clothing, not shaving infected areas until healed, humidifiers in dry climates, washing bedding regularly, to minimize irritation.
- Light and laser therapies: In cases of severe or stubborn conditions, dermatologists can administer laser treatment or phototherapy to reduce redness, inflammation, and texture issues.
- Surgery: Surgical procedures can be done in rare cases such as hair or keratin plugs extraction, microdermabrasion or chemical peels.
The process of improvement typically requires weeks of regular treatment, and regular maintenance treatment is frequently required to avoid relapse. The condition can usually be alleviated by age and can be resolved on its own.
You may also like to read: Diabetic Foot Infections
Home Remedies vs. Professional Treatments
Here is a comparison table of home remedies versus professional treatments for keratosis pilaris:
| Treatment Type | Description | Pros | Cons |
| Home Remedies | Moisturizing, gentle exfoliation with lactic acid, salicylic acid, urea, alpha hydroxy acids, natural oils, oatmeal baths, dry brushing, lifestyle changes (gentle cleansers, loose clothing, humidifiers) | Inexpensive, easy to use at home, generally safe, improves hydration and texture gradually | May take weeks to see results, less effective for severe cases, some natural remedies lack strong evidence |
| Topical Keratolytics | Creams with acids (AHA, BHA), urea to exfoliate and soften skin | Effective for mild-moderate symptoms, reduces keratin plugs | Can cause dryness, irritation, increased sun sensitivity |
| Prescription Retinoids | Tretinoin, adapalene to promote skin cell turnover | More effective for moderate to severe keratosis pilaris | Possible redness, peeling, irritation, sun sensitivity |
| Laser and Light Therapy | Nd:YAG laser, pulse dye laser, IPL to reduce redness and inflammation | Fast improvement, reduces redness and bumps, good for severe or resistant cases | Expensive, multiple sessions needed, side effects like redness, swelling |
| Dermatological Procedures | Microdermabrasion, chemical peels, manual extraction | Improves texture, removes keratin plugs | Can be irritating, may require multiple sessions, possible downtime |
Final Thoughts
Keratosis pilaris can be irritating, yet it is a noninfectious and quite widespread skin disease. Through soft exfoliation, frequent moisturising and the proper skin-care products, this can be significantly enhanced, and bumps kept within a healthy control. It is all about consistency – and if OTC remedies don’t work, a dermatologist can refer you to even more specific options that help make your skin smoother and healthier.
FAQs
What can be mistaken for keratosis pilaris?
- Acne Vulgaris.
- Eruptive Vellus Hair Cysts.
- Folliculitis.
- Keratosis Follicularis (Darier Disease)
- Kyrle Disease.
- Lichen Nitidus.
- Lichen Spinulosus.
- Milia.
What foods make keratosis pilaris worse?
Diet is not a causative factor of keratosis pilaris, but foods that cause inflammation may trigger or exacerbate the symptoms; therefore, it is recommended to avoid inflammatory-causing foods. Individuals with keratosis pilaris must not take dairy products, soy, peanuts, trans fats, sugar, or processed food.
Is KP related to gut health?
Keratosis Pilaris: Little heaps on the upper arm, thigh, or cheek can be an indicator of gluten intolerance and/or gut imbalance.
Why did I suddenly develop KP?
Keratosis Pilaris may be more likely to suddenly occur in patients with dry skin, eczema, asthma, excess body weight or hay fever.