Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
Avoiding long-term ailments including type 2 diabetes, heart disease, and obesity heavily depends on good metabolic health. Among the main determinants of the ability to metabolize is insulin resistance; thereby, by such an insulin response, the insulin and blood sugar become increased in the body due to lesser sensitivity by the body cells to the insulin. As modern lifestyles increasingly involve poor diets, physical inactivity, and chronic stress, the prevalence of insulin resistance in metabolic health has risen sharply. Understanding Role of Insulin Resistance in Metabolic Health is crucial for early intervention and long-term disease prevention.
What Is Insulin Resistance?
Insulin resistance occurs when your muscle, fat, and liver cells become desensitized to Insulin. The key is not as effective and therefore reduced amount of glucose enters the cells despite the presence of insulin. To rectify the problems, your pancreas makes every attempt to produce extra insulin. With time, this increased demand may burn out the pancreas and eventually cause blood sugar to increase and eventually result in type 2 diabetes.
Simple Explanation of How Insulin Works
Insulin is a hormone produced in the pancreas, and it plays a critical role in terms of bioregulation of blood sugar by your body. When you acquire food, then the carbs in the meal are broken down to glucose (sugary substance) and this is discharged to your circulation. Insulin: can be termed as a key: it helps your glucose to be moved out of your blood stream into your muscles, fat and liver cells, where they used up or can also be stored to be used in the future. This keeps the level of blood-sugar in check.
Blood Sugar Regulation
- When the pancreas gets damaged, your body stops producing insulin and as you eat and the blood sugar level augments, pancreas releases some insulin.
- The cells absorb glucose under the influence of insulin and the carbs are decreased in the body.
- In the presence of excess glucose, the excess glucose is stored in the liver as glycogen later being required.
- In case the blood sugar gets too low, another kind of hormone, known as glucagon, informs the liver of the situation and makes it shed the glucose that is previously stored and puts your blood sugar level back to normal level.
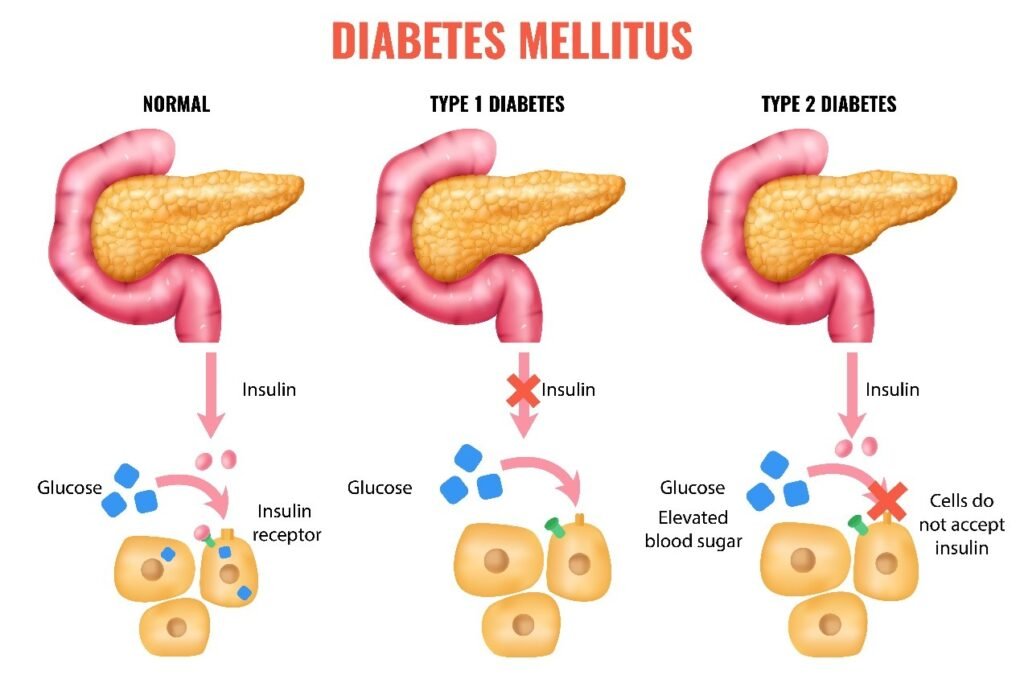
Difference Between Insulin Resistance and Type 1 Diabetes
| Aspect | Insulin Resistance (mainly Type 2 Diabetes) | Type 1 Diabetes |
| Insulin function | Cells ignore insulin or respond poorly | Pancreas cannot make insulin |
| Blood sugar regulation | Body makes insulin, cells do not use it well | No or very little insulin produced |
| Cause | Often related to genetics, excess weight, inactivity, poor diet | Autoimmune: Body attacks insulin-producing cells |
| Usual onset | Often adults (but can affect children) | Usually in children & young adults |
| Treatment | Diet, exercise, medications, sometimes insulin | Lifelong insulin injections |
| Relationship | Can lead to prediabetes and type 2 diabetes | Not caused by insulin resistance; but people with type 1 can develop insulin resistance too |
Key Terms
- Insulin function: Transports sugar out of the blood into the cells to stabilize blood sugar and energy.
- Blood sugar regulation: Insulin and glucose delivery to the body to maintain the level of energy and prevent injury of excessive or insufficient amount of blood sugar.
In Summary: The primary tool that the body uses in balancing blood sugars is the insulin. Insulin resistance implies that cells do not react well to insulin thus leading to an increase in the level of blood sugar. This contrasts with type 1 diabetes, in which insulin production cannot happen at all.
Causes and Risk Factors
1. Obesity and Visceral Fat
- Excess body fat, but excess visceral body fat (stored around the belly organs) increases the chances of the individual having insulin resistance. Visceral fat transports fatty acids and inflammatory messages to the liver through the portal vein, inhibiting the insulin signaling, contributing to metabolic disorder.
- Our own health is also related to obesity and other related conditions that a person may be having like metabolic syndrome, fatty liver or type 2 diabetes; the effect of obesity is relatively stronger when the fat is around the middle part of the body than when they are just beneath the skin surface.
2. Sedentary Lifestyle
- One of the factors that contribute to insulin resistance is a sedentary lifestyle. Sedentary behaviors reduce energy burning, alter the usual metabolism of fats, and reduce the sensitivity of insulin. Sedentary activities incurred in brief durations can lead to direct impairment of insulin activities in the body.
- Exercise can make cells react to insulin and use glucose better and therefore regulate blood sugar better.
3. High-Carb/High-Sugar Diets
- Refined carbohydrates, and sweet nourishments, will increase the sugar levels in the blood rapidly and require another portion of insulin, and in the long run, this will exhaust the system making insulin insensitive.
- Persistent excessive intake results in the release of high amounts of insulin (hyperinsulinemia), which can decrease insulin receptor amounts and capacity or stimulate a metabolic disorder.
4. Chronic Stress and Poor Sleep
- Chronic stress stimulates such hormones as cortisol and epinephrine and may diminish the effects of insulin, elevate blood sugar, in extreme cases, causing insulin resistance itself.
- The lack of sleep not only changes the natural rhythms of the body but also uplifts stress hormones which make the body not very sensitive to insulin, in some cases in a matter of days. The situation can be aggravated by poor sleep and stress which tend to support each other.
5. Genetic Predisposition and Hormonal Factors
- Genetics: Having a history of type 2 diabetes, insulin resistance or having such ailments as PCOS (polycystic ovary syndrome) in the family makes one susceptible. Some of the ethnicities are associated with increased genetic threat too.
- PCOS: Even in the absence of overweight, women with PCOS tend to experience a great deal of insulin resistance. High insulin can stimulate over production of androgen intensifying metabolic and reproduction symptoms.
- Other Hormones: There are also disorders of elevated cortisol levels (e.g. Cushing syndrome), and some drugs that may lead to insulin resistance by interfering with regular insulin action.
You may also like to read: Metabolic Syndrome
Health Complications of Unmanaged Insulin Resistance

Untreated insulin resistance is a significant danger to long term health, as the insulin resistance can harm many body parts and systems. These problems are fundamental aspects of the metabolic disease and are reasons why early identification is vital and beneficial.
Hyperglycemia and Progression to Type 2 Diabetes
When the cells fail to respond to the insulin properly, blood sugar (glucose) remains in a high level, and this is termed as hyperglycemia. At one time or another, the pancreas may not respond to the increased demand of insulin leading to a prolonged high level of sugar in the blood that with time leads to a diagnosis of type 2 diabetes. Chronic hyperglycemia can predispose to damage of blood vessels, nerves, kidneys, eyes and immune system, and substantially diminishes the quality and span of life.
Atherosclerosis and Cardiovascular Disease Risk
Frequently, insulin resistance is coupled with a high blood sugar level, an increase in the level of triglyceride, a reduction in HDL (good cholesterol) and increased blood pressure. These changes in metabolism dissolve the wall of blood vessels and accelerate the growth of atherosclerotic masses (fatty lumps stiffened by the arteries). This means that insulin resistant individuals have a high risk of contracting cardiovascular diseases such as heart attack, stroke, as well as associated diseases of peripheral arteries. This forms one of the reasons why metabolic syndrome (its close relative is insulin resistance) is one of the most serious predictors of heart disease.
Frequently, insulin resistance is coupled with a high blood sugar level, an increase in the level of triglyceride, a reduction in HDL (good cholesterol) and increased blood pressure. These changes in metabolism dissolve the wall of blood vessels and accelerate the growth of atherosclerotic masses (fatty lumps stiffened by the arteries). This means that insulin resistant individuals have a high risk of contracting cardiovascular diseases such as heart attack, stroke, as well as associated diseases of peripheral arteries. This forms one of the reasons why metabolic syndrome (its close relative is insulin resistance) is one of the most serious predictors of heart disease.
Liver Conditions: NAFLD and MASLD
Nonalcoholic fatty liver disease (NAFLD) or as recently renamed metabolic dysfunction steatotic liver disease (MASLD) is a condition that develops when there is too much fat in the liver. Insulin resistance stimulates the rate of fat breakdown in adipose tissues and transports greater quantities of fatty acids to liver thereby overloading the hepatic capacity to oxidize them. Failure to manage this accumulated liver fat may escalate it into plain steatosis and further to more serious inflammation and scarring (nonalcoholic steatohepatitis or NASH) that may further result in liver cirrhosis or liver cancer.
Hormonal Imbalances and Fertility Issues
Deviation in normal hormone signaling is also caused due to insulin resistance especially in cases of certain illnesses like poly cystic ovary syndrome (PCOS) in women. Hormone imbalances cause too much of the male hormones (androgens) to be produced, which results in late or missed periods, infertility and increase in hair growth. There is also an impaired fertility issue since chronic insulin resistance (not confined to PCOS) can lead to general reproductive hormonal imbalances. Low testosterone and fertility issues may be caused in men through insulin resistance.
Conclusion
Insulin resistance is the primary mechanism that interrupts metabolic wellness and is the primary source of the occurrence of severe illnesses like type 2 diabetes, cardiovascular disease, fatty liver, hormonal abnormalities. Being able to identify the symptoms and realizing the effects of insulin resistance are another essential factor in eliminating the long-term effects. Lifestyle changes i.e. enhanced diet, frequent physical activity, weight transportation are important precursors of insulin sensitivity at the early stages or lowering the chances of occurrence of a chronic metabolic disease. People who think that they might be at risk are advised to visit their healthcare workers to get the appropriate assessment and assistance in maintaining their metabolic status successfully.