Dr. Ahmad Shahzad
Founder | Lyallpur Diabetes Foundation
Consultant Diabetologist | Educator | Advocate for Preventive Care
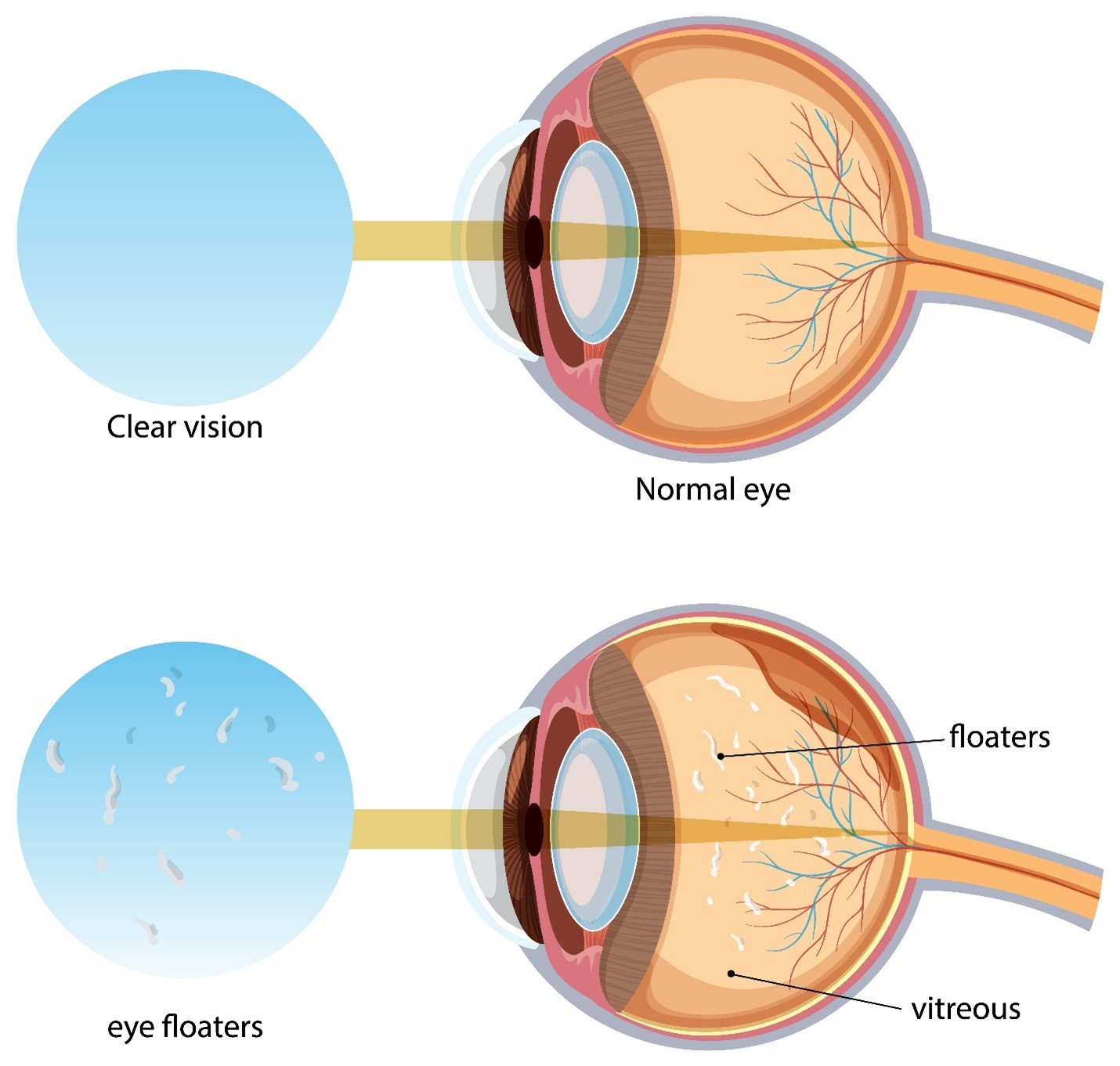
Having diabetes does not only mean checking the blood sugar levels but also being attentive to your health and particularly the eyes. Unconsciously, high blood sugar levels can destroy small blood vessels in the eyes, causing such diseases as diabetic retinopathy, macular edema, cataracts, and glaucoma. Eye check-ups are essential to measure diabetes, as it is important to identify these problems at an early stage, and to avoid vision impairment and improved long-term health results.
Why Are Eye Exams Essential for People with Diabetes?
Diabetics should get eye tests because diabetes may severely damage the eyes, particularly the tiny blood vessels in their retinas, resulting in diabetic retinopathy- the most common reason behind diabetic patients losing their vision. The early signs of this and other eye diseases caused by diabetes including macular edema, cataracts, glaucoma and dry eye can be detected by regular diabetic eye tests. Timely diagnosis through thorough examinations with retina dilation can either avoid or at least postpone loss of sight by laser treatment or injection. Diabetics are highly advised to undergo annual ocular check-ups despite possibly having normal eyesight since monitoring eye health is the best way to address risks.
Why Eye Exams Matter in Diabetes
- Diabetes may lead to leakage, bleeding, and loss of vision in the retinal blood vessels.
- The retinopathy of diabetes occurs in approximately 1 of 3 individuals with diabetes and typically does not have any symptoms at an early stage.
- Annual eye test with pupil dilation makes sure that the retina is well inspected to identify any changes at an early stage.
Preventive Role of Eye Exams
- Early diagnosis results in intervention that could prevent blindness.
- Eye tests also identify other eye problems that are related to diabetes such as cataracts and glaucoma.
- Normal blood sugar level and frequent check-ups help to avoid eye complications.
Common Eye Conditions Linked to Diabetes
Common eye conditions linked to diabetes include:
· Diabetic Retinopathy: It is the most prevalent disease that is caused by diabetes which involves a high sugar level damaging the blood vessels of the retina, resulting in leaking, swelling, and new abnormal blood vessels growing. It may result in blindness and loss of vision.
· Diabetic Macular Edema: This is a form of diabetic retinopathy in which the patient experiences fluid accumulation in the macula (central part of the retina that provides the ability to see finer details) resulting in swelling and distortion of vision. It causes moderate to severe vision loss in diabetes.
Glaucoma: Diabetics are at a higher risk of having glaucoma, a disorder of high pressure that destroys the optic nerve and may cause loss of sight.
Blurred vision: High blood sugar may lead to the swelling of the lens, which will temporarily blur vision until the levels of sugar come to normal.
Cataracts: Diabetes makes the lens inside the eye cloud because in diabetes; cataract develops at an earlier age than non-diabetic people do.
The eye conditions usually have no symptoms in their early stages, so regular eye examination is essential in detecting and treating them to avoid loss of eyesight.
What Happens During a Diabetic Eye Exam?
During a diabetic eye exam, several key steps are performed to thoroughly assess the health of the eyes and detect any diabetes-related damage:
- Visual Acuity Test: During the test, the eye chart begins by testing the acuity of the eye on both short-range and long-range vision (Snellen chart).
- The Special eye drops are applied to enlarge the pupils (widen the eye) so that the eye doctor can have a clearer look at the retina and optic nerve at the back of the eye. Such dilation can lead to blurred vision and sensitivity to light in a few hours.
- Retina and Optic Nerve Examination: The doctor examines the retina, blood vessels and optic nerve, and other internal organs in the eye using a magnifying lens and a bright light or special imaging cameras to detect diabetic retinopathy, macular edema, and other complications.
- Tonometry: this is a test used to measure the pressure in the eye to rule out glaucoma that is more prevalent in diabetic patients.
- Advanced Imaging (when necessary): An imaging method such as Optical Coherence Tomography (OCT) and retinal photography is used to give detailed cross-sectional and photographic images of the retina to detect minor changes or problems in blood vessels.
- Slit Lamp Examination: Slit lamp Microscope is used to observe the internal structures and the surface of the eye carefully.
The doctor then talks about the results of the exam and can prescribe treatments or care. It is recommended that patients come with someone to drive them back home because of temporary blurred vision, dilation causes, and bring glasses or contact lenses, sunglasses and questions about their vision and diabetes.
You may also like to read: Diabetic Retinopathy
How Often Should People with Diabetes Get Eye Exams?
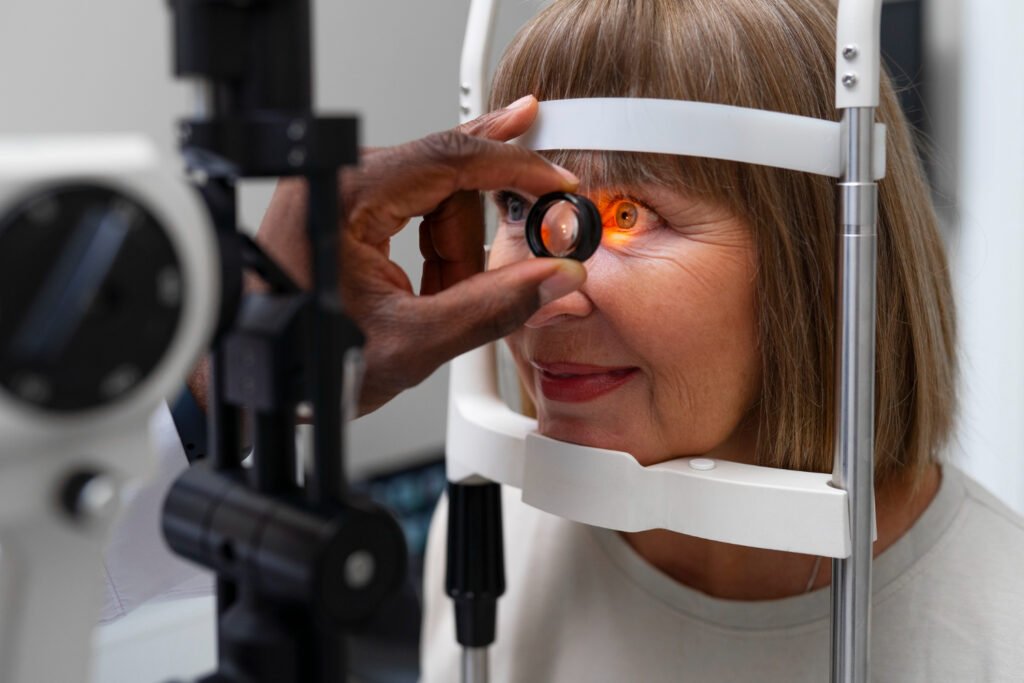
People with diabetes should get eye exams regularly to monitor and prevent diabetes-related eye complications. The general recommended frequency is:
- For Type 1 Diabetes: The first comprehensive eye exam should be within five years after diagnosis, then annually thereafter.
- For Type 2 Diabetes: The first comprehensive eye exam should be done immediately upon diagnosis, with yearly follow-ups.
- Pregnant women with diabetes should have an eye exam as soon as possible after pregnancy is confirmed and may require more frequent exams during pregnancy.
- If diabetic eye disease is detected, more frequent exams will be recommended as needed.
Annual dilated eye exams are crucial because diabetes-related eye conditions often have no early symptoms but can progress silently to serious vision loss. Consistent yearly screening helps in early detection and timely treatment, which can prevent up to 95% of diabetes-related vision loss. Sometimes, based on individual risk and exam results, doctors may extend the exam interval to every 1-2 years, but annual exams remain the standard guideline.
Final Thoughts
In conclusion, regular eye exams are an essential part of diabetes management, helping to detect complications early and protect long-term vision. By combining routine checkups with healthy lifestyle choices and proper diabetes control, individuals can significantly reduce their risk of vision loss. Prioritizing eye care not only safeguards sight but also supports overall well-being in the journey of living with diabetes.
FAQs
Q: Why are eye exams important for diabetics?
A: As a person with diabetes, your annual eye exam is the best way to determine if your blood glucose (blood sugar) levels are affecting the health of your eyes. Even if your vision is completely normal and your eyes feel fine, you could be experiencing the earlier stages of a diabetes-related eye condition.
Q: What are the objectives of diabetic eye screening?
A: The NHS Diabetic Eye Screening Program aims to reduce the risk of sight loss among people with diabetes by the prompt identification and effective treatment of sight-threatening diabetic retinopathy, at the appropriate stage of the disease process.
Q: How to protect eyes from diabetes?
Ways you can help prevent eye problems caused by diabetes include:
- Control your blood sugar. Your doctor can provide directions on how to keep your blood sugar normal and avoid fluctuations that can lead to diabetic eye diseases.
- Lower your blood pressure and cholesterol.
- Stop smoking.
- Avoid harmful rays.
Q: What’s the best vitamin for diabetic eyes?
A: Various studies have indicated that vitamins C, D, E, B1, folate, B12, lipoic acid, lutein, n-acetyl cysteine, and betaine may help to improve endothelial functioning, prevent neuronal damage, reduce blood pressure, and enhance visual acuity.